FHIR API Integration for Healthcare: The Complete Implementation Playbook
Interoperability is no longer an option, but a necessity. However, achieving this interoperability is nearly impossible without using FHIR API integration.
This is why APIs are no longer just a trend shift but are increasingly becoming the backbone of healthcare organizations. In fact, a report by the Office of the National Coordinator for Health Information Technology (ONC) states that nine out of 10 hospitals are using APIs to exchange data and connect with external systems.
But what is surprising is that out of these, nearly 70% of hospitals are using a standardized API, mostly the FHIR healthcare standard. This shift is driven by the limitations of HL7 v2 and regulatory push by compliance, including the 21st Century Cures Act and the ONC Health IT Certification.
Earlier, most of the healthcare systems and EHRs were built on HL7 v2. However, it was a message-based standard and was hard to scale, and required custom interfaces and point-to-point integration, which limited smooth healthcare data exchange.
Moreover, with the 21st Century Cures Act, the healthcare API integration based on FHIR standard has become a regulatory requirement. The law enforces open access to patients and information blocking prevention rules, which depend on how seamless your data exchange is.
That’s why, in 2026, the real question is not whether to implement FHIR APIs. But how to implement them? Because if you adapt it too late, then the gap gets too large between healthcare organizations that have already adapted to it.
In this FHIR API implementation guide, we will break down how to implement FHIR API integration in healthcare while not limiting your scalability, interoperability, or compliance.
FHIR API Integration Fundamentals & Architecture
When you are implementing FHIR API integration, one thing you must understand is that it is not just a healthcare data exchange standard. It is an architecture that enables scalable, real-time, and standardized data exchange between multiple healthcare systems.
To break it down simply, the FHIR is the data structure, and APIs are what transport the structured data. With FHIR, the systems can easily request what they need and when they need it without any delays. However, all this works on the three core components. Let’s take a brief look at those components:
- FHIR Resources: These are the building blocks of data structures as they break a complete patient record into modular parts for faster and seamless data exchange. For instance, the data gets separated into patient, observations, medications, and encounter details for specific data sharing, rather than sharing entire patient records.
- RESTful APIs: The Representational State Transfer Application Programming Interfaces enable real-time and standardized data exchange between healthcare systems using simple web-based requests. This makes it easier for EHR developers to build data pathways. For instance, the GET command retrieves data from patient records, or the POST command creates new data in the patient profile.
- FHIR Profiles (US Core): This is the core of the FHIR API integration, as it gives the consistency needed for the healthcare data transfer. Because the raw FHIR is flexible and does not have the consistency needed in healthcare, these US cores define required data fields, data formats, and coding systems, keeping the language the same across every system.
After understanding these components, let’s move to the FHIR integration architecture. The architecture requires several layers working together to exchange data seamlessly.
- FHIR Server: This is the foundation, as it stores and exposes healthcare data in FHIR format, along with acting as the central access point for APIs in the architecture.
- API Gateway: This is the front door to the FHIR server, as it verifies and routes the requests before they go to the server. Moreover, it also controls the traffic to prevent any server crashes. More importantly, it helps in enforcing security, such as authorization and token validation, to ensure data security and privacy.
- Authentication & Authorization Layer: This is the layer that ensures FHIR API security, where only authorized users and systems get access to the sensitive patient data. In this layer, mostly OAuth 2.0 and SMART on FHIR are used for creating a safety net in the healthcare systems.
- Middleware/Integration Layer: This is the transformation layer of the entire FHIR API integration, as it translates legacy formats such as HL7 v2 into FHIR resources and connects these systems to modern applications.
In short, by understanding and implementing this correctly, you can move beyond fragmented integrations, enable real-time data access, and build future-ready healthcare systems.
Strategy: Choosing the Right Healthcare Data Exchange Standard
Although transitioning to FHIR APIs is becoming necessary, not all healthcare organizations can do so instantly. The time to adopt a data exchange approach, whether it is FHIR, HL7 v2, or hybrid, varies based on system infrastructure, integration complexity, and long-term interoperability goals.
Here’s a table that gives an overview of each approach:
| Feature | FHIR APIs | HL7 v2 | Hybrid Approach |
| Data Format | Structured (JSON/XML) | Message-based (text) | Mixed |
| Integration Style | API-driven | Interface-based | API + Interfaces |
| Real-Time Access | Yes | Limited | Partial |
| Scalability | High | Low | Moderate to High |
| Implementation Effort | Moderate | High (custom work) | Moderate |
| Use Case | Modern apps, interoperability | Legacy workflows | Transition phase |
If you choose FHIR APIs, it can enable real-time and scalable data exchange in your system. This is why it is the best choice for modern applications, patient engagement tools, and scalable integrations.
Whereas, HL7 v2 is mostly used in legacy systems from a decade or two back. This healthcare data exchange standard is reliable for internal workflows but has limited flexibility and scalability.
However, most of the healthcare organizations are using a hybrid approach, as many hospitals use legacy systems. That’s why FHIR APIs are added as an integration layer over HL7 v3 infrastructure. This allows them to continue their operations and enable interoperability at the same time, without slowing down the clinical workflows.
In short, selecting the right strategy is not about eliminating HL7 v2 but about reducing disruption, minimizing risk, and balancing current system limitations with future interoperability needs.
Real-World Use Cases of FHIR API Integration
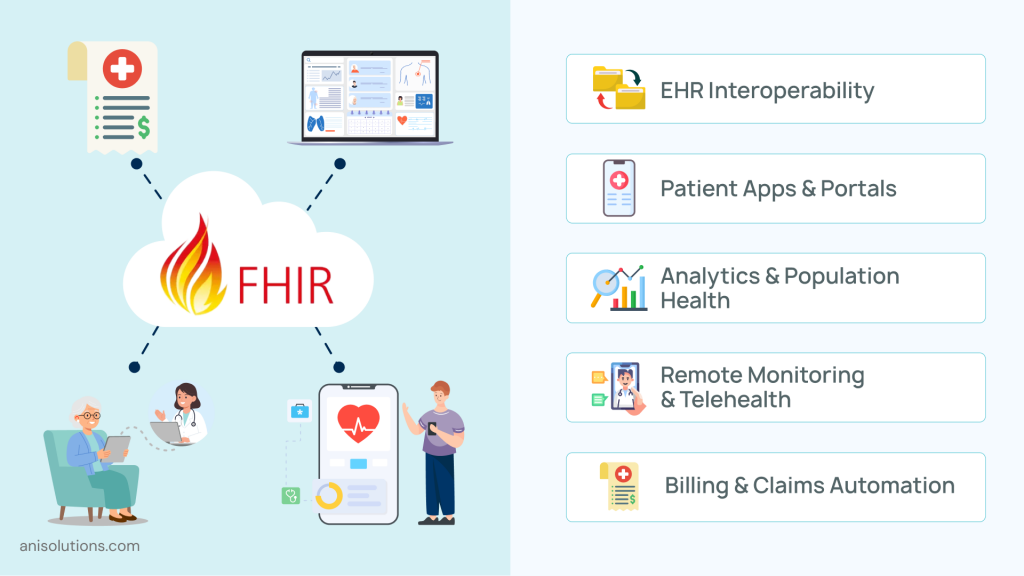
FHIR API integration delivers the most value when applied to real clinical and operational workflows, not just system connectivity. Moreover, it is much easier to understand how it works with some use cases. So, here are five high-impact use cases that demonstrate how organizations are leveraging FHIR APIs in practice.
- EHR-to-EHR Interoperability: FHIR APIs enable seamless data exchange between different EHR systems, allowing providers to access patient records across organizations. This improves care continuity, reduces duplicate tests, and ensures clinicians have complete patient information at the point of care.
- Patient-Facing Applications: With FHIR-based APIs, healthcare organizations can securely share data with mobile apps and patient portals. Patients can access their medical history, lab results, and medications in real time, supporting engagement and compliance with patient access regulations.
- Population Health & Analytics: The FHIR APIs support bulk data access for analytics platforms, enabling organizations to identify trends, manage risk, and improve outcomes at scale. This is critical for value-based care models where performance depends on data-driven insights.
- Remote Patient Monitoring (RPM) & Telehealth: FHIR integration allows wearable devices and telehealth platforms to transmit real-time patient data directly into EHR systems. This enables continuous monitoring, early intervention, and better chronic care management without increasing provider workload.
- Revenue Cycle & Claims Automation: FHIR APIs streamline data flow between clinical and billing systems, reducing manual entry and errors in claims processing. This leads to faster reimbursements, improved coding accuracy, and better financial performance.
Implementation Playbook: How to Implement FHIR API Integration
While it is important to understand the technical side of the FHIR API integration, it’s also important to understand how to implement it successfully. And a successful implementation requires a tried and tested approach, balancing clinical workflows, system limitations, and compliance requirements. Here is a step-by-step FHIR API integration guide:
- Define Clear Use Cases: The first step is to identify the problems you need to solve and understand all the use cases carefully and clearly. You need to understand whether you need APIs for patient data access or EHR interoperability. This is a crucial step because if you don’t have a clear understanding of the APIs you build, they don’t align with business goals and fail to deliver measurable results.
- Choose the Right FHIR Version & Standard: After identifying use cases, the next step is to finalize the FHIR version, and here, mostly the FHIR R4 is used. Additionally, you need to adopt standardized FHIR profiles such as US Core to maintain consistency, as FHIR is too flexible, and these profiles are essential to maintain the same meaning and data structure across systems.
- Map Legacy Data to FHIR Resources: This is the most complicated part of the whole implementation process, as many systems rely on HL7 v2 or custom interfaces. It is quite difficult to map these formats to FHIR resources, and it requires careful alignment of data fields and clinical meaning.
- Design Scalable APIs & Architecture: In this step, you define how your APIs will function, from endpoint and data access patterns to error handling. Moreover, the design of architecture also happens in this part, and a well-designed architecture always has FHIR servers and API gateways ensuring long-term scalability, performance, and seamless integration with third-party applications.
- Implement Security & Compliance: With this step, the patient data is secured by implementing authorization and authentication using standards such as OAuth 2.0 and SMART on FHIR. The system ensures compliance with regulations with role-based access, end-to-end encryption, and audit logging for all API requests.
- Testing & Validation: Having working APIs does not mean true interoperability, which is why it is important to test the APIs to validate whether they share data correctly across systems. The essential part is conformance and interoperability tests for avoiding integration failures after deployment.
- Deployment, Monitoring, & Optimization: Implementing FHIR API integration is not a one-time process, as after deployment, you need to constantly monitor performance, usage, and errors. With this governance, you can gather feedback and optimize integration to evolve with new use cases and regulations.
FHIR API Security & Compliance
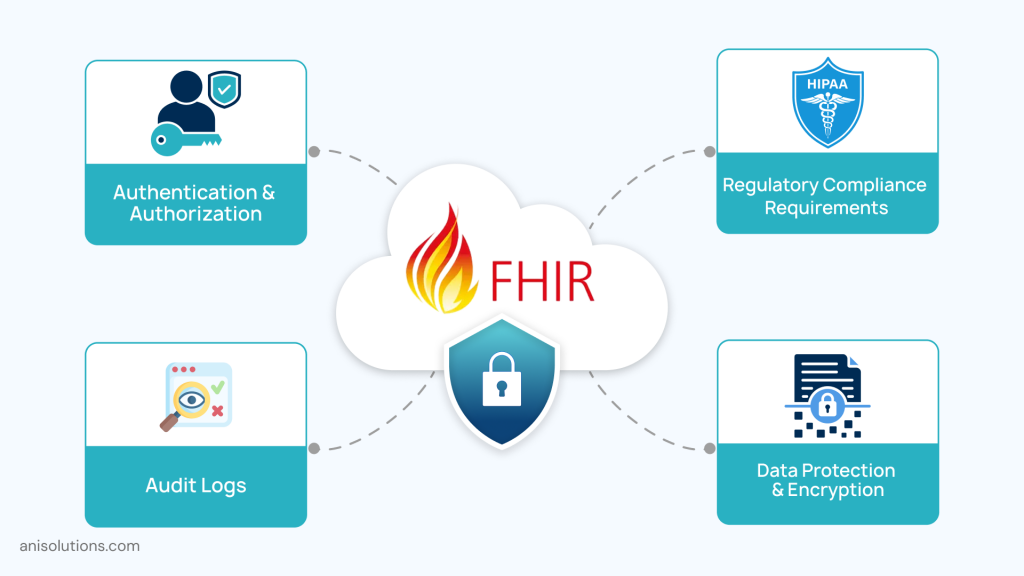
In healthcare, the responsibility of protecting sensitive patient data lies with the healthcare organizations. This is why it is important to embed FHIR API security and compliance into the architecture. Here is what you need to add without failing during the FHIR API implementation:
- Authentication & Authorization: This limits access to patient data as only authorized persons can view, share, and edit the patient data. The FHIR APIs use standards such as OAuth 2.0 and SMART on FHIR to achieve this.
- Data Protection & Encryption: With end-to-end encryption using standards like HTTPS and TLS, the data is protected during transmission and prevents any unauthorized interception, maintaining privacy and trust across the network.
- Regulatory Compliance Requirements: Another important point is to align the integration with the 21st Century Cures Act and HIPAA for secure handling of data, along with preventing both intentional and unintentional information blocking.
- Zero-Trust Security & Audit Logging: You also need to adopt a zero-trust policy and thoroughly validate every device connecting to the network. Moreover, auditing each access to the patient record and any changes made is also important for maintaining accountability in case of a data breach.
SMART on FHIR: Enabling the Healthcare App Ecosystem
When it comes to SMART on FHIR, it defines how applications securely access and use that data across different systems. This is an important part of EHR API integration, and together they are the foundation for a modern, app-driven healthcare ecosystem.
With SMART on FHIR, you get a framework for smooth third-party applications to integrate with EHRs in an easy and efficient way. This eliminates the need for custom integrations for each new connection and deploys across multiple healthcare platforms that support SMART standards.
More importantly, this helps you build applications that work across different EHR systems without costly rework. The second advantage is that it reduces the development time needed with each new innovation, and it also uses OAuth 2.0 for secure access and standardized authentication.
In simple terms, SMART on FHIR can be compared to an app store, where EHRs act as platforms and third-party applications to extend their functionality. This shift allows healthcare organizations to move from static systems to a more flexible, app-based approach to delivering care.
CDS Hooks: Embedding Real-Time Clinical Intelligence
The CDS hooks embed intelligence directly into clinical workflows, allowing healthcare systems to deliver real-time, context-aware insights. They operate on an event-driven model, meaning when a specific event happens within EHR, such as prescribing medications, a trigger is activated.
After the trigger is activated, it sends relevant patient data through FHIR-based APIs to an external decision support service. Then the service analyzes the data and returns actionable insights, such as alerts, suggestions, or clinical guidance, directly within the clinician’s workflow.
With this approach, the continuity of care and existing process remain undisrupted. And rather than requiring clinicians to search for information across multiple systems, CDS hooks provide timely recommendations within the same interface, improving efficiency and reducing cognitive load.
In short, CDS hooks FHIR to enable real-time clinical insights and help reduce medical errors, enhance patient safety, and support evidence-based decision making. They also create a foundation for integrating advanced analytics and AI-driven recommendations into everyday care delivery, transforming healthcare systems into proactive, intelligent environments.
Bulk FHIR: Scaling Data for Population Health

As healthcare is moving beyond individual patient interactions, the data volume is also increasing. While standard FHIR APIs are ideal for real-time, patient-level access, they are not designed for efficiently transferring massive datasets. This is where bulk FHIR data export comes into the picture.
The bulk FHIR, also known as Flat FHIR, enables organizations to export and process large volumes of healthcare data in a scalable and efficient manner. Instead of making multiple individual API calls, systems can request data in NDJSON format, making it easier to process and analyze at scale.
This capability is particularly important for use cases such as population health management, risk stratification, and quality reporting. Healthcare organizations can analyze trends across thousands or even millions of patient records, enabling more informed decision-making in VBC models.
It also plays a key role in advanced analytics and AI initiatives, where large datasets are required for training predictive models and generating insights. In short, this enables high-volume data access without overloading systems, ensuring both performance and scalability.
AI-Ready Healthcare Data Layer
With healthcare becoming increasingly data-driven and AI-ready, it is also important to make the data usable for analytics and automation. And this is where FHIR APIs make interoperability the foundation of an AI-ready data layer.
The reason for this is that FHIR efficiently structures data into a consistent and understandable format across the system. This standardization is critical for AI systems, which need clean, accurate, and reliable data for generating accurate insights on time.
However, the structured data is not enough as it needs to be understood consistently across all systems. This is where semantic consistency with standards like LOINC, SNOMED CT, and ICD ensures that clinical concepts mean the same in every connected system.
That’s why FHIR and standardized terminologies create a data layer that is interoperable and AI-compatible. This enables use cases such as predictive analytics, risk stratification, clinical decision support, and personalization.
Challenges & Best Practices in FHIR API Integration
While FHIR API integration enables scalable interoperability, real-world implementation comes with challenges that require careful planning and execution.
Data Mapping & Semantic Inconsistency: Mapping legacy data (such as HL7 v2 or custom databases) to FHIR resources is one of the most complex aspects of implementation. Inconsistent data formats, missing fields, and varying clinical terminologies can lead to inaccurate or incomplete data exchange.
- Best Practice: Adopt standardized profiles like US Core and use middleware to normalize and transform data. Aligning with coding systems such as LOINC and SNOMED CT ensures semantic consistency.
Legacy System Constraints: Most healthcare organizations still rely on legacy systems that were not designed for API-based interoperability. Replacing these systems entirely is often not feasible due to cost and operational risks.
- Best Practice: Implement a hybrid approach by layering FHIR APIs on top of existing systems. This enables modernization without disrupting critical workflows.
Versioning & Standard Variability: Different FHIR versions and inconsistent implementations across vendors can create compatibility issues. “FHIR-enabled” systems may still interpret data differently.
- Best Practice: Standardize on a specific FHIR version (such as R4) and enforce consistent implementation using defined profiles and validation frameworks.
Security & Compliance Complexity: FHIR APIs expose sensitive patient data, making security and regulatory compliance a major concern. Misconfigured access controls or weak authentication can lead to serious risks.
- Best Practice: Implement OAuth 2.0 and SMART on FHIR for secure access, along with encryption, audit logging, and strict role-based permissions.
Performance & Scalability Challenges: Handling large volumes of API requests, especially in real-time and bulk operations, can impact system performance if not designed properly.
- Best Practice: Use scalable architecture patterns such as API gateways, caching, and asynchronous processing (e.g., Bulk FHIR) to maintain performance under load.
Conclusion: Future-Proofing with a Unified FHIR Strategy
In a nutshell, FHIR API integration is not just a technical requirement, but also a strategic decision for healthcare organizations. It helps you build a future-ready healthcare system that can handle data effortlessly and scale as the data volume increases.
Most importantly, it solves the problem of rebuilding the system each time there are new regulatory requirements, healthcare innovation, and support for AI-driven healthcare. Moreover, at the rate of healthcare technology progressing, FHIR API integration gives you a leverage to keep up with the tech for the next decade.
This saves you the time and money to adapt to evolving technology and regulations without adding new custom interfaces and point-to-point integrations each time.
So, if you have not adapted to EHR APIs, then it is time that you integrate FHIR APIs into your EHR systems. Contact our team and let’s get started with designing your healthcare API integration today.
Frequently Asked Questions
FHIR API integration enables healthcare systems to exchange data via standardized FHIR APIs. It allows real-time access to structured patient data, enabling seamless communication between EHRs, apps, and third-party systems while improving interoperability and scalability.
Unlike HL7 v2’s message-based approach, FHIR APIs provide real-time, on-demand access to data using standardized formats such as JSON. This reduces the need for custom interfaces, simplifies integrations, and enables scalable interoperability across systems, making healthcare data exchange faster, more flexible, and easier to implement.
FHIR R4 uses API-driven, resource-based data exchange, enabling real-time interoperability. HL7 v2 relies on message-based communication and custom interfaces. In practice, FHIR supports modern applications and scalability, while HL7 v2 remains embedded in legacy systems for internal workflows.
Successful implementation involves defining use cases, selecting FHIR standards (R4, US Core), mapping legacy data, designing APIs, implementing security (OAuth 2.0), testing interoperability, and continuous monitoring. A structured approach ensures scalability, compliance, and alignment with clinical and operational workflows.
Yes, the 21st Century Cures Act mandates patient data access and prohibits information blocking. FHIR-based APIs are widely used to meet these requirements, making them essential for compliant, standardized, and accessible healthcare data exchange.
SMART on FHIR apps use standardized APIs and OAuth 2.0 authentication to securely connect with EHR systems. They can be embedded within clinical workflows, enabling real-time access to patient data and allowing developers to build interoperable applications that work across multiple EHR platforms.
CDS Hooks are event-driven triggers that deliver real-time clinical recommendations within EHR workflows. When specific actions occur, patient data is sent via FHIR APIs to decision support systems, which return actionable insights, improving care quality and reducing errors.
Bulk FHIR is used when large-scale data access is required, such as population health analytics or AI model training. Unlike standard APIs designed for individual queries, bulk export enables efficient retrieval of massive datasets without overloading systems.
Yes, FHIR reduces long-term costs by minimizing custom interfaces and enabling reusable, standardized integrations. While initial implementation may require investment, it significantly lowers maintenance complexity and supports scalable, future-ready interoperability compared to traditional point-to-point models.
Key challenges include data mapping from legacy systems, inconsistent data standards, version variability, security implementation, and performance scalability. Addressing these requires structured planning, standardized profiles, and a robust integration architecture to ensure reliable, interoperable data exchange.
FHIR APIs enable wearable devices and RPM platforms to transmit patient data directly into EHR systems in real time. This supports continuous monitoring, early intervention, and better chronic care management by integrating device-generated health data into clinical workflows.
FHIR APIs must implement OAuth 2.0, encryption (TLS), role-based access control, and audit logging to comply with HIPAA. These measures ensure secure access, data protection, and regulatory compliance when handling sensitive patient information.
FHIR standardizes healthcare data into structured, machine-readable formats, making it suitable for AI and analytics. Combined with consistent clinical terminologies, it enables predictive modeling, risk stratification, and automated insights, supporting data-driven decision-making and personalized care.
- On April 8, 2026
- 0 Comment