
TEFCA and Healthcare Data Exchange: How It Impacts Your Integration Strategy
Fragmentation has always been a problem in whole data transformation and building digital infrastructure. While the regulations made the EHRs, APIs, and connecting with health information exchange mandatory, many systems rely on point-to-point integration.
And this creates one significant challenge for healthcare CTOs, because interoperability exists, but data is not exchanged efficiently. This is where the TEFCA healthcare data exchange comes into the picture.
The Trusted Exchange Framework and Common Agreement (TEFCA) is a framework introduced by the Assistant Secretary for Technology Policy (ASTP). This framework is the base for taking fragmented systems to a nationwide, network-based model of interoperability.
To put it simply, TEFCA is the network of networks or a national data floor, where healthcare data moves seamlessly between multiple systems or organizations. Now, as 2026 is reaching its mid-term, this shift is already happening rapidly.
Many healthcare organizations have connected to Qualified Health Information Networks (QHINs) and are creating a nationwide health information exchange model. Most importantly, for healthcare CTOs and healthcare IT developers, the TEFCA directly impacts how interaction strategies are designed.
That’s why in this blog, we will break down the TEFCA common agreement technical requirements and how TEFCA impacts healthcare integration strategy.
Let’s see how aligning with the TEFCA simplifies architecture and helps you build long-term interoperability.
What Is TEFCA & How It Transforms Data Exchange?
As mentioned in the introduction, the TEFCA is a nationwide initiative introduced by the ASTP, formally known as the Office of the National Coordinator for Health Information Technology. This framework mainly focuses on allowing standardization along with secure and scalable healthcare data exchange across networks.
At a high level, TEFCA defines a framework for how organizations connect, exchange data, and establish trust. With this framework, one of the biggest challenges is the lack of consistency in health information exchange models.
Moreover, the TEFCA consists of two core components. The first is the Trusted Exchange Framework, which defines the principles for interoperability. The second component is the Common Agreement, which defines legal and operational rules for healthcare providers.
However, it is not just an HIE network but a network-of-networks that is not limited by region, vendor ecosystems, or custom integrations. This reduces fragmentation and expands access beyond siloed exchange environments.
If you align your EHR and healthcare systems, then building interoperability into the core capability becomes easier. Moreover, it also helps you comply with information blocking regulations, FHIR-based APIs, and standardized datasets such as USCDI.
In short, the Trusted Exchange Framework and Common Agreement (TEFCA) is the shift from isolated, point-to-point integrations to standardized and scalable interoperability.
TEFCA Readiness Snapshot (5-Min Self-Assessment)
Assess NowThe Architecture of TEFCA: Understanding QHINs
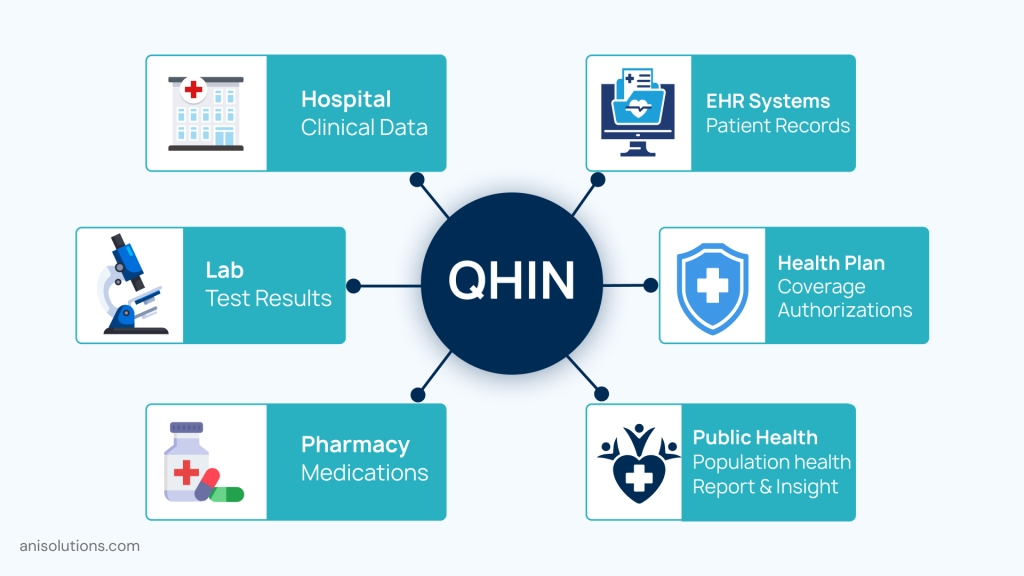
At the center of the TEFCA framework is the Qualified Health Information Network (QHIN), which makes the TEFCA network-of-networks. This is the infrastructure layer that makes the nationwide data exchange possible.
Moreover, a QHIN is a designated network that is built with a common set of technical, operational, and governance standards. More importantly, these are not just centralized networks, but a federated network where multiple networks connect and exchange health data seamlessly.
The biggest advantage of QHIN is the single on-ramp approach. This approach eliminates the need for traditional point-to-point integrations, reducing the efforts and time needed to build and maintain each custom interface.
If we put it more simply, the healthcare organization is no longer needed to connect separately with labs, pharmacies, or other healthcare providers. With TEFCA, healthcare providers can get access to multiple networks by just connecting to a single QHIN. Furthermore, these QHINs can connect with each other seamlessly, creating a nationwide data exchange at scale.
All this changes how interoperability is built into the healthcare systems, as organizations can easily leverage a network-based architecture, where data exchange is standardized and scalable.
In short, for healthcare CTOs, QHINs mean a fundamental shift from building connections to creating a network-based infrastructure, simplifying interoperability.
The Common Agreement: Technical, Governance, & TEFCA Compliance Framework
The Common Agreement is the legal framework of the TEFCA. This is the component that decides legal and operational requirements for participating in this framework. In simple words, this is the foundation that enables healthcare organizations to exchange data under a unified framework.
This agreement defines how healthcare organizations connect with QHINs, their responsibilities, and how data can be accessed and shared across the network. The focus of these rules is to standardize the networks rather than letting organizations decide their own exchange role, preventing fragmentation.
| Area | What It Covers | Why It Matters for CTOs |
| Technical | Data exchange standards, interoperability protocols, and security requirements | Directly impacts system design and TEFCA-ready architecture |
| Governance | Roles, responsibilities, and participation rules | Ensures consistent interaction across networks |
| Privacy & Security | Data access controls, consent, and compliance safeguards | Supports regulatory alignment and patient trust |
| Operational | Onboarding, workflows, and network participation processes | Affects implementation timelines and scalability |
The technical side of the Common Agreement defines the use of FHIR-based APIs and standardized data sets such as USCDI for maintaining data consistency across systems. This helps in aligning systems with broader interoperability.
Whereas, on the governance part, it establishes a shared trust model, ensuring that data is shared securely without negotiating individual agreements each time. Moreover, it states how the authentication and authorization work and which identities are authorized for data access in the systems.
More importantly, it leads to TEFCA compliance, which requires healthcare organizations to align their systems, workflows, and policies with the requirements defined in the Common Agreement.
That’s why, for healthcare CTOs, the TEFCA, although not a mandatory requirement yet, is a blueprint for how data exchange will happen in the near future.
TEFCA Compliance Checklist for CTOs (2026 Edition)
Get NowHow TEFCA Impacts Your Integration Strategy?
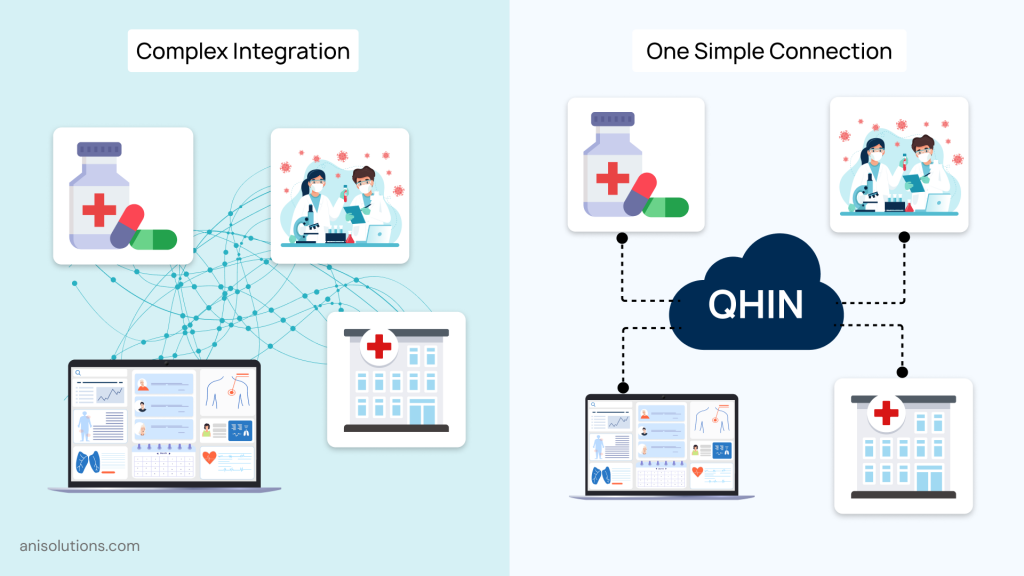
Traditionally, the EHRs are connected with other systems through point-to-point integration. While it works for a small network, as the hospitals expand, each new connection needs a custom interface and API connections. And this becomes hard to maintain at scale and in the long run.
However, the TEFCA shifts this approach because it not only brings a new framework but also redefines how healthcare organizations integrate systems. This framework connects systems with a network-based architecture.
With this approach, instead of building new connections, you can connect with multiple systems at once through OHINs. This gives you access to a broader ecosystem, reducing integration costs and introducing a more standardized way to exchange data across the network.
This is a shift that changes how the EHRs are designed, impacting how a healthcare CTO builds an integration strategy. For instance, transitioning to a TEFCA-ready infrastructure requires an API-first, FHIR-aligned architecture that supports standardized data exchange.
Moreover, it also requires aligning with identity management, access controls, and governance frameworks with nationwide interoperability expectations. One more critical change is how you select a vendor, as not all vendors support TEFCA-based exchange, and a wrong choice can mean limited scalability as the ecosystems evolve.
Strategic Benefits: Why Providers Should Join a QHIN
Adopting TEFCA is not just a requirement or experiment; it is increasingly becoming a strategic advantage for early adopters.
One of the biggest benefits of joining a QHIN for providers is the reduced integration complexity. Rather than building multiple connections and new custom APIs to connect with labs, pharmacies, or other healthcare providers, you can easily access them all through a single network. This, along with simplifying infrastructure, also lowers the long-term maintenance costs.
Another benefit is faster and more consistent access to patient data across healthcare organizations. By connecting with a QHIN, you can easily exchange patient records from external providers or have a faster care transition, improving clinical visibility and reducing care delays.
Moreover, you get much more efficient workflows from an operational perspective as everything is standardized. This way, care teams spend less time managing interfaces and more time on care delivery and coordination.
There are also some long-term advantages with the healthcare industry moving toward a nationwide health information exchange model. So, the healthcare organizations that adopt early have an advantage in scaling interoperability, aligning with evolving regulatory requirements, and avoiding costly rework in the future.
In short, for healthcare leaders, joining a QHIN is not only about connectivity, but also about building a foundation for scalable, future-ready interoperability.
QHIN ROI Calculator and ROI Framework PDF
Download NowChallenges & Considerations in TEFCA Adoption
While it is beneficial to adopt the TEFCA framework, it is not as easy as it seems and has multiple challenges that need to be addressed carefully. And for many organizations, this shift requires both technical readiness and operational alignment.
The first hurdle is transitioning from legacy systems, as they were not designed for integration with FHIR-aligned and network-based data exchange. In these systems, ensuring compatibility with QHIN connectivity and standardized data often requires careful planning and investment.
After this, the second challenge is governance and compliance. Many healthcare organizations have their own exchange and governance policies, and that’s why aligning with standardization rules for data sharing and access can be difficult.
Additionally, not all vendors have TEFCA-ready architectures for their systems, which can limit options or delay the implementation timeline. Moreover, if you choose the wrong development partner, it can compromise long-term scalability and interoperability.
Finally, expanding data exchange across networks needs robust security, consent management, and access controls for ensuring compliance and maintaining patient trust. However, building all this can take time and complicate the implementation.
In short, the key challenge is not whether to adopt TEFCA, but how to do it without compromising existing operations and long-term scalability.
Preparing Your Organization for TEFCA Participation
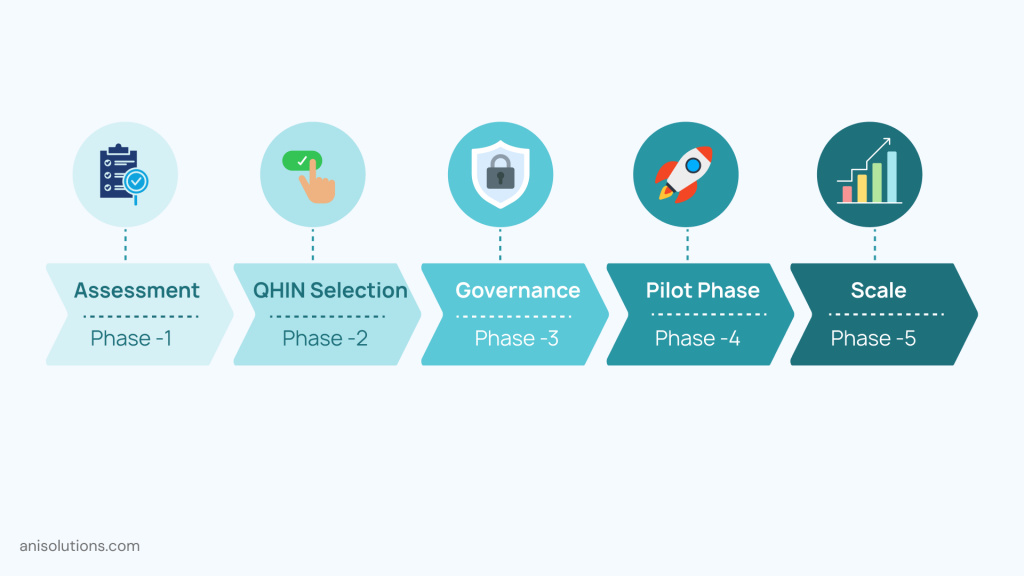
Adopting TEFCA requires more than technical integration—it demands a strategic, phased approach that aligns infrastructure, governance, and vendor ecosystems.
The first step is assessing your current interoperability landscape. This includes evaluating existing EHR capabilities, integration architecture, API readiness, and alignment with standards such as FHIR. Identifying gaps early helps define the scope of changes needed for TEFCA participation.
Selecting the right QHIN partner is equally critical. Different networks may vary in terms of capabilities, coverage, and onboarding support. Choosing a QHIN that aligns with your organization’s data exchange needs and long-term strategy can significantly impact implementation success.
Organizations must also update internal data governance and compliance frameworks. This involves aligning policies with TEFCA’s Common Agreement, including data access rules, privacy safeguards, and operational responsibilities across teams.
A phased adoption approach is often the most effective. Rather than attempting a full-scale transition, many organizations begin with pilot use cases—such as specific data exchange workflows or limited network participation—before expanding gradually.
Equally important is aligning internal stakeholders. IT, compliance, clinical operations, and leadership teams must work together to ensure a smooth transition without disrupting existing workflows.
Ultimately, successful TEFCA adoption is not about rapid implementation—it’s about building a scalable foundation for nationwide interoperability. Organizations that take a structured, strategic approach will be better positioned to adapt as the TEFCA ecosystem continues to evolve.
TEFCA Implementation Roadmap (90-Day Plan)
Click HereConclusion: The End of Data Silos
In a nutshell, the TFCA is the foundation for taking healthcare from a fragmented and point-to-point integration approach to a more interoperable and seamless data exchange. Moreover, it is one of the best ways to ready your healthcare systems for future interoperability and data-driven care.
That’s why the healthcare organizations that adopt this framework early will have a significant head start over the organization that realizes its importance too late. So, if you have not aligned your EHR with the TEFCA common agreement requirements yet, then it’s time to do so now.
We at A&I solutions can help you in building an integration strategy along with the EHR aligned with the TEFCA. Click here to book your consultation and start the free assessment right away.
Frequently Asked Questions
TEFCA (Trusted Exchange Framework and Common Agreement), introduced by the Office of the National Coordinator for Health Information Technology, enables standardized, nationwide health data exchange. It shifts interoperability from fragmented, point-to-point integrations to a network-based model, improving scalability, consistency, and cross-organizational data access.
Traditional HIEs are often regional or vendor-specific, relying on custom integrations and inconsistent standards. TEFCA introduces a network-of-networks model, enabling nationwide connectivity through shared governance and standardized protocols, reducing fragmentation and eliminating the need for multiple one-off integrations.
A QHIN is a TEFCA-designated network that enables organizations to exchange data under a common framework. It acts as a single on-ramp, allowing participants to connect once and access multiple networks, enabling scalable, secure, and standardized nationwide data exchange.
The Common Agreement defines technical, operational, governance, and privacy requirements for data exchange. It standardizes how organizations connect, share data, and ensure compliance, including security protocols, permitted use cases, and responsibilities—creating a consistent, trusted framework across all participating networks.
TEFCA participation is currently voluntary. However, due to alignment with federal interoperability initiatives and evolving regulations, it is becoming a de facto standard. Organizations that do not align early may face increased integration complexity and limited access to nationwide data exchange networks.
TEFCA shifts integration from point-to-point connections to network-based architecture. Organizations must adopt API-first, FHIR-aligned systems and design for QHIN connectivity, reducing integration overhead while enabling scalable, standardized data exchange across a broader healthcare ecosystem.
Joining a QHIN reduces integration complexity, enables faster access to patient data, and improves care coordination. It also supports scalable interoperability, aligns with nationwide exchange initiatives, and positions providers to adapt efficiently as healthcare moves toward standardized, network-based data sharing.
Preparation involves assessing current infrastructure, ensuring FHIR and API readiness, selecting the right QHIN partner, and aligning governance policies with TEFCA requirements. A phased approach—starting with pilot use cases—helps organizations transition without disrupting existing workflows while building long-term interoperability capabilities.
- On April 7, 2026
- 0 Comment


