
ONC Interoperability Standards Advisory: A Compliance Checklist for 2026
One of the most pressing issues that healthcare is facing is not data availability but using the available data. As per research by RBC Capital Markets, the healthcare industry creates nearly 30% of the entire world’s data volume.
However, when it comes to moving this data from one system to another, it often doesn’t move in a way that every system consistently understands it or generates insights. The reason for this is siloed systems and a lack of seamless interoperability.
And this is where building interoperability into the core of EHR and healthcare systems becomes important. But every organization has different EHRs and its own custom APIs or proprietary formats that don’t match other systems, creating inconsistencies.
Moreover, in 2026, as care becomes more data-driven, having interoperable systems is not an option anymore. Most importantly, you need to ensure that each integration is standard-driven, scalable, and clinically meaningful.
That’s where the ONC Interoperability Standards Advisory (ISA) comes in. This is a framework developed by the Office of the National Coordinator for Health Information Technology. This framework guides organizations on how to bring consistency into their healthcare data by structuring it in a standard format.
However, shifting legacy systems to modern healthcare platforms is not that easy. They have to build FHIR-based APIs and build systems that match the USCDI v3 for data consistency.
However, doing this while maintaining compliance can be difficult without a proper roadmap.
That’s why we have designed an ONC interoperability standards checklist for 2026 to help you identify gaps and standardize your system with ONC ISA without compromising compliance, long-term interoperability, and scalability.
What Is the ONC Interoperability Standards Advisory (ISA)?
Before we dive into the checklist, let’s first understand what exactly the ONC Interoperability Standards Advisory (ISA) is. If we put it in simple terms, it is a playbook for which standards to use while sharing healthcare data.
It is the framework that, although it is not a regulation, impacts the compliance of the systems. Because regulations like ONC Health IT Certification and the 21st Century Cures Act enforce data standardization. Most importantly, it simplifies the use of healthcare interoperability standards based on the use cases rather than giving a list of standards to implement.
For instance, for patient data access, it recommends HL7 FHIR, and for sharing lab results, it shares LOINC terminology.
Moreover, in the ONC ISA framework, every standard is evaluated on two things: its maturity and adoption level. It has three maturity levels: emerging, pilot, and mature, along with two adoption levels: limited use and industry-wide adoption. An example of this is the FHIR standards for EHRs, which are a mature standard with wide adoption.
In the healthcare landscape, this framework guides every organization for standardization, as every hospital has its unique formats and integration that may or may not match other systems. This guideline eliminates that uncertainty, and it enables true interoperability and brings consistency in understanding the meaning across multiple systems.
ONC ISA Standards Mapping Cheat Sheet
Download NowThe Shift to USCDI v3: Expanding the Data Baseline
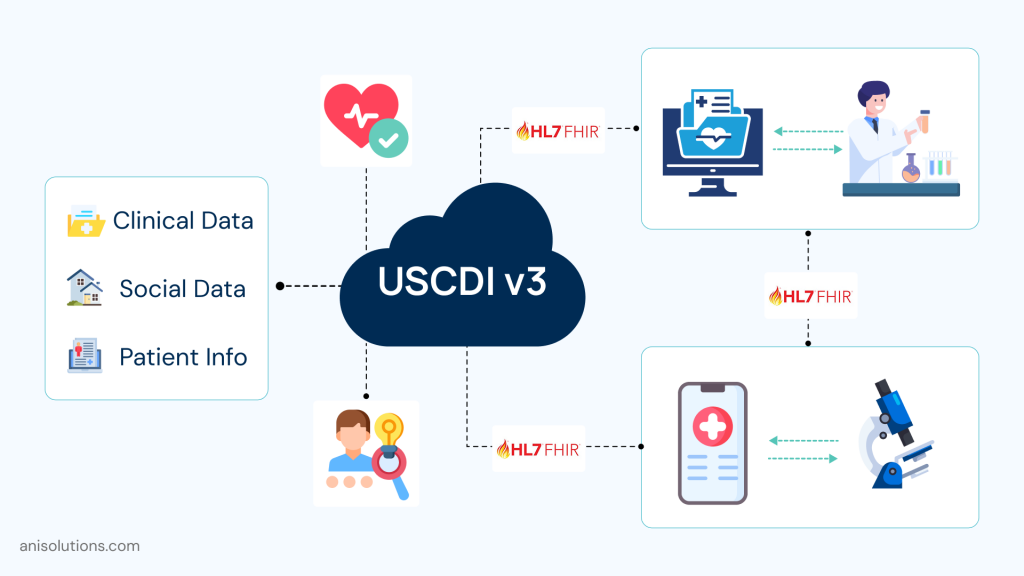
While the Interoperability Standards Advisory for healthcare providers recommends the healthcare interoperability standards to implement the USCDI (United States Core Data for Interoperability), it shows you which data to move.
If we put it more clearly, it defines the core set of data elements that must be available across providers and certified health IT systems. This ensures that data remains consistent and reliable, leading to true interoperability.
One of the advanced versions of this framework is USCDI v3, and it expands the scope of datasets from its earlier versions. This version adds expanded patient data with more details, social determinants of health (SDOH), and care team information to share.
This expansion of data elements changes how healthcare IT teams design the EHR systems. One of the changes is that the data can no longer be unstructured, and it must be standardized and structured to be accessible through standards such as HL7 FHIR.
And healthcare organizations must align their systems by transitioning to USCDI v3 requirements. This means the system must also be updated in data models, APIs, and clinical workflows to ensure that data is captured at the point of care.
In short, USCDI v3 is the new baseline to maintain consistency across healthcare organizations and share data meaningfully.
ONC Certification & API Standards Alignment
The ONC health IT certification is a program by the Office of the National Coordinator for Health Information Exchange (ONC) to ensure that the EHR is built on the healthcare interoperability standards.
This certification baseline is that the system supports standard data sets such as USCDI v3 and provides API-based access to patient health information. However, having the ONC certification does not mean interoperability. If the system is not guided by the ONC Interoperability Standards Advisory (ISA) for healthcare interoperability standards, it should be implemented in the real world.
Another essential component of this is the adoption of FHIR standards for EHR, enabling modern, API-based data exchange. This standard also ensures that the data stored is structured, accessible, and easily exchangeable across multiple systems seamlessly.
So, aligning with ONC certification means supporting HL7 FHIR. USCDI v3 implementation and maintaining consistency across different systems with ONC ISA. Additionally, these factors also allow for long-term scalability, interoperability, and meaningful data exchange.
Assess Your Readiness for USCDI v3 With this Implementation Checklist
Assess NowThe 2026 Compliance Checklist for CTOs
As I said in the intro, aligning EHR with the ONC Interoperability Standard Advisory (ISA) is not an easy task. Because you have to take the legacy system that worked with HL7 v2 to a modern healthcare platform that supports HL7 FHIR-based APIs.
That’s why healthcare CTOs and IT teams need a structured checklist to ensure alignment with evolving healthcare interoperability standards and regulatory requirements. The starting point for this is to assess your current systems and identify gaps and USCDI v3 implementation requirements.
After that, organizations must evaluate their EHRs to see if they support the capture, structure, and exchange of all required data elements, including social determinants of health, clinical notes, and care team information.
To simplify this process, here is the ONC interoperability standards checklist for 2026 to align EHR in a structured way:
| Area | What to Validate | Why It Matters |
| USCDI v3 Alignment | Ensure full support for required data elements | Enables standardized data exchange and compliance |
| ISA Alignment | Align with ONC-recommended healthcare interoperability standards | Ensures real-world interoperability beyond certification |
| API Readiness | Implement fhir standards for EHR with secure APIs | Supports real-time, scalable data exchange |
| Terminology Mapping | Use SNOMED CT, LOINC, and ICD consistently | Ensures data is interpretable across systems |
| Interoperability Testing | Validate send, receive, integrate, and use capabilities | Confirms true interoperability, not just connectivity |
| Governance & Monitoring | Establish data governance and compliance tracking | Maintains long-term interoperability readiness |
| ISA Update Alignment | Review updates regularly | Keeps systems aligned with evolving standards |
| Scalable Integration | Use API-first, modular architecture | Future-proofs interoperability strategy |
This checklist gives you a framework for evaluating whether systems are able to support scalable, standards-driven, and compliant. However, it is a one-time process, as compliance and standards are ongoing processes.
In short, you need to update your strategies to the changing healthcare interoperability standards and frameworks. By doing this, you can have long-term interoperability, performance, and innovation.
FHIR & ONC Certification Validation Toolkit
Check NowCommon Challenges in Implementing Interoperability Standards
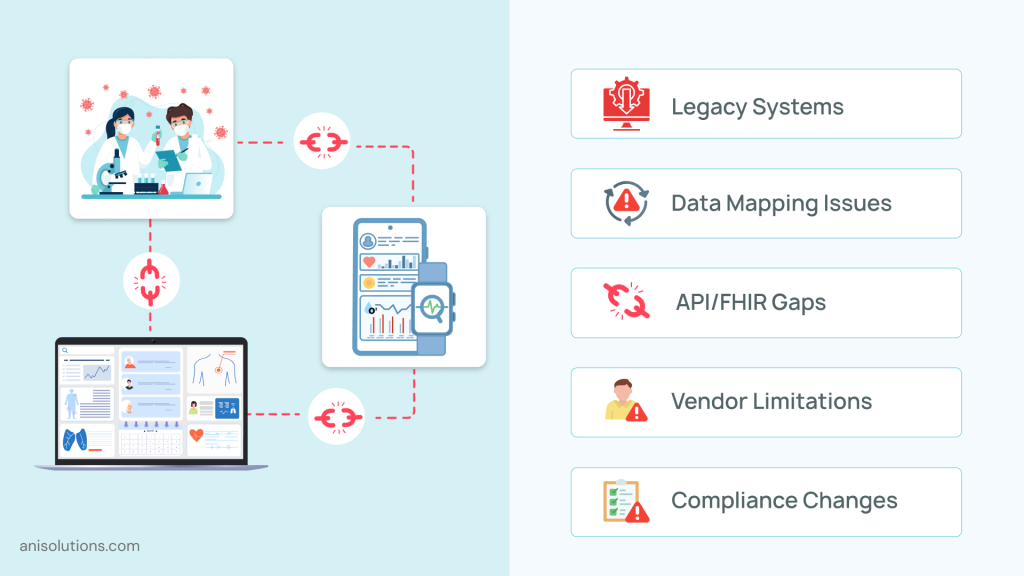
When it comes to implementing the ONC Interoperability Standards Advisory and modern healthcare interoperability standards, it is important to understand that it can face significant challenges.
The first challenge is to modernize the legacy systems due to their limitations. Many hospitals have built custom EHR systems that work on proprietary standards and HL7 v2, and these systems were not designed to support modern API-driven interoperability. So, integrating these systems into the frameworks needs additional transformation layers, which increases complexity and cost.
Another major challenge is data normalization and mapping, as different systems use different data formats. This creates inconsistencies in terminology and structure, leading to mismatched or unusable data. This becomes a hurdle when aligning with the USCDI v3 implementation requirements that require standardization and structured data across networks.
One more challenge is vendor readiness, as not every vendor has the architecture to support APIs, FHIR capabilities, and is built on custom API,s leading to gaps that impact seamless data exchange.
Additionally, evolving frameworks and compliance requirements are also challenges that healthcare organizations face. They need to constantly update their system to stay compliant and keep up with the evolving requirements to stay competitive.
In short, healthcare organizations need to constantly update their integration strategies and build EHR systems that can support long-term scalability and interoperability without rebuilding entire systems with each new update.
Staying Updated with ONC Standards & ISA Changes
As mentioned above, the ONC Interoperability Standards Advisory (ISA) and even USCDI are continuously evolving. For instance, the regulations state to use USCDI v3, but currently, the framework has v6 and v7 in the draft, so your EHR needs to be ready to support v6 and v7 in the near future.
Similar to USCDI, the other healthcare interoperability standards are also always evolving, so you need to monitor the changes continuously. And the best way to keep track of the changes and any new updates is to create a proper structure to keep track of ONC resources or any ISA publications and the Federal Register.
By doing this, healthcare organizations can easily align their systems with the updates, including clinical workflows. Moreover, if you have a regular auditing process to identify gaps and areas of improvement, you can ensure interoperability strategies are aligned with current standards.
In short, maintaining standardization or interoperability is not a one-time process, but an ongoing strategy. Healthcare organizations that continuously monitor the standards and adapt to the changes are better aligned with compliance standards and have a significant competitive advantage over those that adapt too late.
Conclusion: Future-Proofing Your Health IT Systems
In a nutshell, healthcare is increasingly becoming data-driven, and that’s why having systems that make data accessible, exchangeable, and immediately usable is not an option anymore. That’s why standardization is also becoming crucial, along with aligning healthcare systems with the ONC Interoperability Standards Advisor (ISA).
So, if you are using legacy systems, then it is time to upgrade to a more modern and truly interoperable system. And this is possible with implementing API frameworks, USCDI v3, and FHIR standards for EHR.
Want to take your legacy system to interoperability and long-term scalability without compromising compliance and security? Then talk to our EHR integration experts and start your system assessment right away.
Frequently Asked Questions
The Office of the National Coordinator for Health Information Technology Interoperability Standards Advisory (ISA) is a guidance framework that identifies recommended healthcare interoperability standards and specifications. It helps organizations understand which standards to use for specific use cases, ensuring consistent, scalable, and effective data exchange across healthcare systems.
The ONC ISA maps interoperability use cases to recommended standards, helping organizations choose the most appropriate technologies. It evaluates standards based on maturity, adoption, and implementation considerations, enabling healthcare providers and vendors to make informed decisions and align with widely accepted healthcare interoperability standards.
USCDI v3 defines a standardized set of healthcare data elements required for exchange. In 2026, it expands data coverage to include SDOH and clinical notes, improving consistency, enabling better interoperability, and supporting more comprehensive, data-driven care delivery across systems.
ONC Health IT Certification ensures EHR systems meet baseline interoperability requirements, including support for standardized data and APIs. It enforces compliance with regulations, while frameworks like ISA guide implementation. Together, they ensure systems can exchange data effectively and align with evolving healthcare interoperability standards.
Key steps include assessing alignment with USCDI v3, validating ISA-recommended standards, ensuring FHIR API readiness, standardizing terminology, testing interoperability, and establishing governance processes. Regular reviews aligned with ONC updates help maintain compliance and support scalable, future-ready interoperability across healthcare systems.
Common challenges include legacy system limitations, inconsistent data formats, complex integrations, and limited vendor readiness. Organizations also struggle with evolving standards and workflow adoption. These factors make it difficult to achieve seamless interoperability, even when systems meet basic compliance requirements.
Healthcare organizations can track updates through ONC resources, ISA publications, and the Federal Register. Monitoring official announcements and regulatory updates ensures awareness of new standards, certification changes, and evolving interoperability requirements, helping organizations stay compliant and aligned with industry expectations.
Healthcare organizations should review interoperability standards at least quarterly or biannually. Regular audits aligned with ONC ISA updates ensure systems remain compliant, up to date, and capable of supporting evolving data exchange requirements, reducing risks associated with outdated implementations.
- On April 6, 2026
- 0 Comment

