
Efficient Budget Planning for EHR Projects in 2026
When a custom EHR development starts, the first thing that comes to your mind is how much this is going to cost, right?
The answer to this question lies in how strategically you plan your EHR budget. If you treat the EHR budget planning like any other project, then the cost will be significantly higher and completely different from what you initially estimated.
And the reason for this is how EHRs are developed is totally different from other software. The cost of the EHRs depends on the complexity of features, architecture, how many systems you are going to integrate, and finally the compliance requirements.
Each of this factor increases the costs and you have to strategically decide where to invest resources and the prioroties for the development. For instance, you don’t need to build all features together, as first you can add only necessary features and then add other advanced features in phases.
This reduces the total cost of ownership (TCO) by distributing the budget over a period of time. However, if you fail to account for these factors, then it leads to situations scope creep, budget overruns, and finally project failures.
So, to prevent these scenarios, it is important to understand what impacts the healthcare IT budgeting both directly and indirectly. Without this, no matter how well you plan the budget, it will only be effective for short-term success and not sustainable for long-term planning.
But if you understand what makes up EHR implementation costs and how early planning can help you control the budgets, then you can easily estimate medical software development costs.
In this guide, we will explore the foundation for budgeting for custom EHR development while understanding the common pitfalls that lead to higher EHR software costs.
Let’s dive in!
Foundation of Healthcare IT Budgeting
When it comes to strong EHR budget planning, it starts with understanding the foundation. The decisions made in discovery and scoping decide how your EHR project’s cost will look in the first six months. Let’s take a look at what defines the foundation of healthcare IT budgeting:
- Discovery & Scoping to Prevent Scope Creep: This is the phase where most of the budget gets structured as you define the requirements, priorities, and specifications for the custom EHR. However, if you fail to account for this with clarity, then the medical software development cost can go over the original estimate. With each new feature, redesign, or must-have feature added, the EHR software price increases significantly.
- Compliance, Security, & Regulatory Considerations: In healthcare, compliance is not a one-time EHR cost, as regulatory requirements update regularly. And with HIPAA safeguards, audit logging, access controls, interoperability standards, and regulations, the cost of architecture and development. When you account for compliance from day one, instead of an add-on budget, it quickly exceeds the limits.
- Internal Resource & Operational Cost Planning: The EHR implementation cost is also influenced by the internal impact. The design, integration, training, and other operational costs don’t show up on invoices, but they directly affect productivity and timelines. If you ignore this, it leads to unrealistic budgets, so planning this upfront creates more accurate costs and smoother execution.
More importantly, when you plan this early, it gives you the flexibility to adjust the budget. However, during the development process, the changes become expensive and delay timelines. That’s why early planning is the key to controlling EHR software pricing over the long run.
Direct & Indirect Costs in EHR Projects
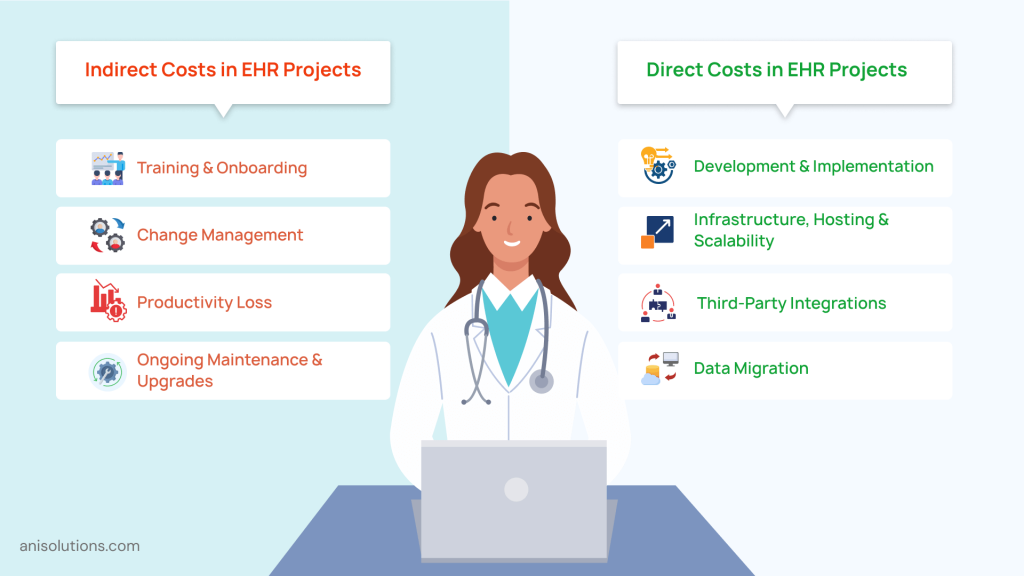
One of the biggest reasons why EHR budget planning exceeds the initial estimate is that organizations only budget for direct costs. But when the hidden costs start to surface, they start draining the finances quickly. That’s why to build a realistic budget, you need to understand both direct and indirect costs:
- Development & Implementation Costs: These are the most visible costs that healthcare organizations account for, and they also take the most of the EHR budget. It includes core development, UI/UX design, clinical workflow configuration, testing, and go-live support. However, the costs vary based on features, complexity, specialty-specific workflows, customizations, and interoperability needs.
- Infrastructure, Hosting, & Scalability Planning: The EHRs grow over time, and these decisions can destabilize the entire EHR development, becoming a recurring financial burden. However, many organizations underestimate how quickly data volume, user load, and traffic grow. If they don’t plan for scalability well, it leads to unplanned infrastructure upgrades, performance fixes, and higher operational costs, increasing initial EHR implementation costs.
- Third-Party Integrations & Data Migration: During custom EHR development, integrations are important for connecting healthcare environments. The cost increases with each integration point, such as connecting labs, pharmacies, imaging systems, billing platforms, payer systems, and external EHRs, which require interface development, testing, and ongoing maintenance. Moreover, data migration is also a costly and risky process, yet a necessary expense. If underestimated, these costs can quickly destabilize the healthcare IT budgeting process.
- Hidden Operational Costs That Impact Total Spend: The most dangerous costs are the ones that are not directly visible. It includes training costs, change management, and handling productivity loss during adoption, and these indirect costs impact the overall EHR software pricing, reducing ROI.
The 2026 EHR Budget Planning Checklist: Avoid Cost Overruns & Scope Creep
Get NowUnderstanding Total Cost of Ownership (TCO) for EHR Systems
In EHR budget planning, one thing that makes the budgeting process more complicated is considering upfront costs similar to the total cost of ownership. Upfront costs include development, configuration, and go-live support. Whereas, the total cost of ownership includes maintenance, compliance, infrastructure growth, training, integration, and operational support.
So, to plan for these costs, a practical way to approach this is by using an EHR total cost of ownership checklist mindset. The table below shows the difference between upfront cost and long-term ownership quickly:
| Cost Category | Upfront Cost Focus | Long-Term Ownership Impact |
| Development & Configuration | Initial build, customization | Enhancements, refactoring, feature expansion |
| Compliance & Security | Baseline HIPAA safeguards | Regulatory updates, audits, security upgrades |
| Infrastructure & Hosting | Initial cloud setup | Scaling, storage growth, disaster recovery |
| Integrations | Interface development | Maintenance, monitoring, version changes |
| Training & Adoption | Initial user training | Ongoing onboarding, retraining, workflow updates |
| Support & Maintenance | Go-live support | Helpdesk, bug fixes, performance tuning |
How AI Supports Smarter EHR Budget Planning?

Developing an EHR is not as simple as storing patient data or compiling features, that’s why budget planning manually becomes difficult. This is where AI comes into the picture and helps in EHR budget planning by improving visibility, predictability, and decision quality in the early development phase.
- AI-Assisted Cost Forecasting & Risk Identification: AI models can easily analyze historical project data, feature complexity, and compliance requirements, and help produce more accurate budget forecasts. More importantly, they help identify risks in budget planning before they turn into budget overruns. This allows healthcare organizations to proactively address risks rather than reacting to challenges mid-project.
- Feature Prioritization to Optimize Budget Allocation: One of the most expensive mistakes is building many features early, so choosing the right features to build early makes budgeting for custom EHR development easier. Here, AI helps prioritize features that are must-haves for the healthcare organization, separating functionality from nice-to-haves, keeping medical software development costs under control.
- Reducing Long-Term Testing & Rework Costs: AI also supports smarter testing strategies, with automated test generation, regression testing, and anomaly detection, reducing manual effort and catching issues early. This significantly reduces rework, minimizes post-implementation fixes, and stabilizes long-term EHR implementation cost.
- AI as a Planning Aid, Not a Replacement for Governance: What many clinicians fear is that AI replaces human oversight; however, it only helps improve accuracy and efficiency, and does not replace governance. If used correctly, AI helps strategically budget for EHR software development by making informed decisions.
Free EHR TCO Calculator: Estimate 5-Year Ownership Costs in Minutes
Estimate NowCommon Budgeting Mistakes in EHR Projects
If you are budgeting based on just assumptions rather than evidence, then even a well-funded EHR project fails. And these assumptions become very costly mistakes in EHR budget planning. Let’s take a look at those mistakes:
- Underestimating Compliance & Integration Costs: Compliance and system integration are must-haves in the EHR systems. However, when you underestimate the importance of the HIPAA safeguards, such as encryption, audit logging, access controls, and interoperability requirements, you introduce ongoing costs and extend the budget beyond initial estimates. Similarly, integrating labs, billing systems, and external systems requires continuous maintenance, adding to EHR implementation costs.
- Ignoring Internal Operational Impact: Budget plans often focus on vendor pricing while overlooking internal costs. Clinicians pulled into design sessions, IT teams supporting interfaces, and administrative staff training all add to costs. When these operational impacts are ignored, healthcare IT budgeting becomes unrealistic, and execution suffers.
- Budgeting Without Aligning Scope, Timeline, & Resources: If the development is misaligned with scope, delivery timeline, and available resources, it leads to budget overruns. That’s why it is crucial to keep the goal realistic and based on the available resources rather than aggressively adding features. Doing this can increase rework and EHR software pricing.
- Treating EHR Software Pricing as Static: EHR costs change with the regulatory changes, technology advancements, and scaling requirements. That’s why it is essential not to assume that the software price will remain the same over time, as this creates gaps in the EHR budget planning process, leading to unrealistic costing.
Conclusion: Building a Realistic & Defensible EHR Budget
Long story short, budgeting is the crucial part for any EHR project as it decides how much you need to invest to get the results you want. However, for effective EHR budget planning, you need to analyze data and make evidence-based decisions.
Moreover, you need to align the budgeting decisions with long-term EHR goals, scope, and prioritize the features that are must-haves. With this strategy, it becomes easier to allocate resources and invest in the right features, rather than overbuilding and overrunning the EHR budget.
So, if you are planning to build your own EHR and need help in planning the budget effectively, then Click here to connect with our experts and get your personalized quotation.
Frequently Asked Questions
Q. What are the primary components of an EHR project budget?
An EHR project budget typically includes development and configuration, compliance and security, infrastructure and hosting, data migration, third-party integrations, training, internal resource allocation, and ongoing maintenance to support long-term system stability and scalability.
Q. How can healthcare organizations prevent budget overruns during EHR implementation?
Budget overruns are best prevented through detailed discovery, realistic scoping, early compliance planning, phased feature delivery, and aligning scope with timelines and resources. Strong governance and regular budget reviews help catch risks before costs escalate.
Q. What is the difference between upfront EHR development costs and total cost of ownership (TCO)?
Upfront costs cover building and launching the EHR, while TCO includes long-term expenses such as maintenance, compliance updates, infrastructure scaling, training, integrations, and operational support throughout the system’s lifecycle.
Q. How much budget should be allocated for data migration and third-party integrations?
Data migration and integrations often consume a significant portion of EHR budgets due to data cleanup, validation, testing, and ongoing maintenance. Underestimating this area is common and frequently leads to unexpected cost increases post-implementation.
Q. How does custom EHR development compare to SaaS licensing costs from a long-term budgeting perspective?
Custom EHR development requires higher upfront investment but offers long-term cost control and flexibility. SaaS models appear cheaper initially but can become more expensive over time due to recurring licensing, user-based fees, and limited customization.
Q. Can AI tools help improve accuracy and forecasting in EHR budget planning?
Yes, AI tools can analyze historical data, project complexity, and risk patterns to improve cost forecasting, highlight budget risks early, and support smarter feature prioritization—while still requiring human oversight for governance and compliance decisions.
An EHR project budget typically includes development and configuration, compliance and security, infrastructure and hosting, data migration, third-party integrations, training, internal resource allocation, and ongoing maintenance to support long-term system stability and scalability.
Budget overruns are best prevented through detailed discovery, realistic scoping, early compliance planning, phased feature delivery, and aligning scope with timelines and resources. Strong governance and regular budget reviews help catch risks before costs escalate.
Upfront costs cover building and launching the EHR, while TCO includes long-term expenses such as maintenance, compliance updates, infrastructure scaling, training, integrations, and operational support throughout the system’s lifecycle.
Data migration and integrations often consume a significant portion of EHR budgets due to data cleanup, validation, testing, and ongoing maintenance. Underestimating this area is common and frequently leads to unexpected cost increases post-implementation.
Custom EHR development requires higher upfront investment but offers long-term cost control and flexibility. SaaS models appear cheaper initially but can become more expensive over time due to recurring licensing, user-based fees, and limited customization.
Yes, AI tools can analyze historical data, project complexity, and risk patterns to improve cost forecasting, highlight budget risks early, and support smarter feature prioritization—while still requiring human oversight for governance and compliance decisions.
- On February 21, 2026
- 0 Comment


