The Real Cost of EHR Development: A Complete Breakdown & Budgeting Guide
One of the most asked questions in any EHR demo or discovery call is ‘how much does developing a custom EHR cost us?’
And most likely, the reason you are here is that you also want to know how much budget you will need and where you can save money. But before directly diving into the budgets and factors that affect the costs, we need to clarify a misconception.
In our meeting, what we have observed is that many healthcare organizations just look at the label price of any EHR to make the choice. However, this is the mistake that later balloons the budget in the custom EHR software development.
Because many hidden factors that are not mentioned in the pricing quotes affect the cost of developing EHR systems. For instance, the off-the-shelf EHRs show low licensing costs, but they don’t explicitly mention the integration costs that can go into thousands of dollars or the ongoing maintenance costs.
Whereas, in custom EHR software, the hidden costs come from extended timelines, specialized talent requirements, and additional features. That’s why, rather than just looking at prices, you need to look at the value and long-term ROI for deciding on the development partner and EHR systems.
If you want to have a clear understanding of how much EHR development costs, then you need to know more about what drives the cost. When you know those factors, then the EHR project budget planning becomes more realistic, and you can adapt to changes on the go, rather than stopping the entire development process.
That’s why, in this blog, we will walk you through the EHR development cost breakdown with each factor that contributes to development costs. Most importantly, we will explore the strategies to control the budgeting without compromising development quality, safety, and ROI in the long-term.
So, let’s get started without further ado!
Calculate Your Custom EHR Budget in Just a Few Minutes with These Questions
Click HereWhat Drives the Overall EHR Development Cost?
When it comes to the cost of EHR development, one biggest mistakes is assuming it is going to be fixed, as it isn’t and never will be. The reason for this is that, unlike off-the-shelf EHRs, which come with a price tag, custom EHR development costs change with what you build, how you build it, and how far you want to scale it.
Moreover, each clinic operates differently, has specific workflows, integration, and feature needs, changing the EHR development costs. Here are some of the key cost drivers that shape the EHR software development cost:
- Scope & Future Depth: Deciding the scope of the EHR software development before starting the process is crucial to controlling the budget. If you know which features to add, how to store data, and how to build workflows, then it costs much less and helps you adapt better to the changes. So, deciding whether to start with basic features gives you the flexibility to add some advanced features later in the development if the budget is sufficient.
- Compliance & Regulatory Readiness: Another factor that has high costs is compliance and regulatory features. When you follow HIPAA and ONC standards, you need to add audit trails, role-based access controls, and end-to-end encryption, which increases complexity and cost. That’s why considering these costs helps you plan the costs effectively.
- Integration & Interoperability: When you are connecting different systems such as labs, billing, pharmacies, and more, you need an API-first architecture for seamless integration. This increases the development costs and complexity of the development process.
- Scalability & Future Readiness: The healthcare landscape is always evolving, and the EHR needs to be designed to keep pace with these changes. Additionally, the systems must be able to function in multi-location environments, and this increases the upfront investment but prevents the expensive reworks in the future.
One more factor that can derail the EHR budgeting process is only considering the surface-level estimate. However, you also need to include the time before starting development and after development is completed.
To calculate the real development costs, you need to also add the costs of discovery workshops, workflow mapping, compliance validation, and other development phases. And when you consider ongoing costs and the other cost drivers, you can easily plan budgets and avoid overruns during the development process.
Comprehensive Cost Components in an EHR Development Project

The EHR development costs are not only made up of the development costs mentioned in the earlier point. The whole budget has different components, and each part brings different costs and increasing complexity.
For instance, for planning the entire development process, you need professionals who understand the healthcare domain, and this increases the costs later in the project if ignored. So, like this, there are many cost components that directly influence the overall EHR development costs.
This section breaks down these factors and how they impact the final costs:
- Team Expertise & Planning Effort
One of the most underestimated parts of the development cost of EHR systems is the expertise required to develop the EHR and plan the entire process. The EHR development is different from the generic software development as it requires specialized developers, QA engineers, healthcare-specific architects, and compliance specialists who understand the workflows and regulatory requirements.
This phase is what lays the foundation for successful EHR development, and rushing this without properly building the team can lead to misaligned features, rework, and increased timelines. And this significantly impacts the EHR development costs during the process.
- UX/UI Design for Clinician-Centric Workflows
When designing the interfaces for the EHR, it is important to remember that it’s not just about aesthetics; it also needs to be easy to navigate. Because if designed poorly, it increases documentation time, clinicians’ burnout, and training costs, indirectly increasing the cost of EHR ownership.
If you want a clinician-centric UX requires role-based interfaces, optimized charting flows, reduced clicks, and context-aware data presentation. So, designing and validating these workflows involves usability testing with real clinicians, iterative prototyping, and accessibility considerations, contributing to the EHR development cost, but preventing costly usability issues after implementation.
- EHR Software Development & Customization
The core EHR software development cost is driven by architecture choices and customization depth. With backend development, the costs come from data models, APIs, audit logs, access control, and scalability planning, whereas frontend development focuses on responsive, role-based design.
This increases the costs and complexity of specialty-specific workflows and adds automation rules. However, building flexibility into the system early reduces future redevelopment costs while stabilizing the EHR development cost breakdown over time.
- Feature Complexity & Functional Modules
In EHR, not all features have the same costs, as it changes according to the complexity of the feature. If you want basic modules for patient demographics and appointment scheduling, they cost less, but when it comes to advanced features like e-prescribing or predictive analytics, it inflates the costs of developing an EHR.
Each added feature introduces dependencies, testing environments, and compliance considerations. And organizations that fail to prioritize the features needed early face scope creep, one of the biggest drivers of EHR development cost.
- Integrations & Interoperability
This component of the EHR development process is one of the most expensive and technically demanding. It needs expertise in HL7 and FHIR standards, along with an understanding of how to seamlessly connect labs, pharmacies, billing systems, and other external systems to EHRs.
Along with this, it also needs data migration, normalization, validation, and interoperability testing, which requires money and efforts both. Moreover, this integration needs ongoing maintenance, increasing the cost of developing the EHR system.
- Compliance, Security, & Quality Assurance
Keeping the systems compliant is a continuous expense for the organization as the regulations change constantly. So, you need to add the costs of updating HIPAA, ONC, and other regulations regularly, along with the audit trails, role-based permissions, encryption, and penetration testing.
Planning the compliance proactively reduces long-term risk and prevents expensive remediation. On the other hand, if you depend on reactive compliance fixes, it can lead to hefty fines if the system does not meet compliance requirements, increasing the cost of developing EHR software.
- Data Migration & System Transition
Migrating legacy data to a new system is one of the riskiest and most expensive phases in the development process. It includes multiple steps from secure data extraction and mapping to validation and reconciliation, and all of this requires specialized tooling and careful execution to protect patient data integrity.
With large datasets, inconsistent legacy formats, and regulatory constraints, increase in both effort and cost. Poorly planned migrations frequently result in delayed implementation timelines, extending the EHR software development timeline and increasing overall project cost.
- Training, Adoption, Maintenance & Ongoing Support
The cost of EHR systems doesn’t stop at launch, as training clinicians, managing adoption challenges, monitoring performance, and supporting users all contribute to recurring costs. And these ongoing maintenance typically accounts for 15-15% of the initial EHR development cost per year. If you ignore this, it leads to underfunded support models and degraded system performance over time.
How Development Timeline Directly Impacts EHR Cost?
In EHR projects, every additional week is not a delay in deployment but also an increase in staffing costs, ROI delay, and extended compliance oversight. That’s why it is important to follow the EHR software development timeline if you want to maintain your budgets properly.
However, most healthcare organizations focus on deciding the scope, but underestimate the importance of careful development planning. That’s why poor planning leads to delays in every stage from discovery to implementation, increasing the cost of EHR software development.
- The Relationship Between Timeline, Resources, & Budget
EHR development budgets are closely tied to how long specialized resources remain engaged. The developers, QA engineers, architects, and compliance specialists who have experience in healthcare software development are paid based on the time and effort spent.
When timelines extend, the costs of EHR increase because of prolonged adoption of high-cost resources, extended testing cycles, constant reworks due to changing requirements, and increased project management and coordination effort.
Even when the feature scope remains unchanged, a longer timeline almost always results in a higher EHR development cost.
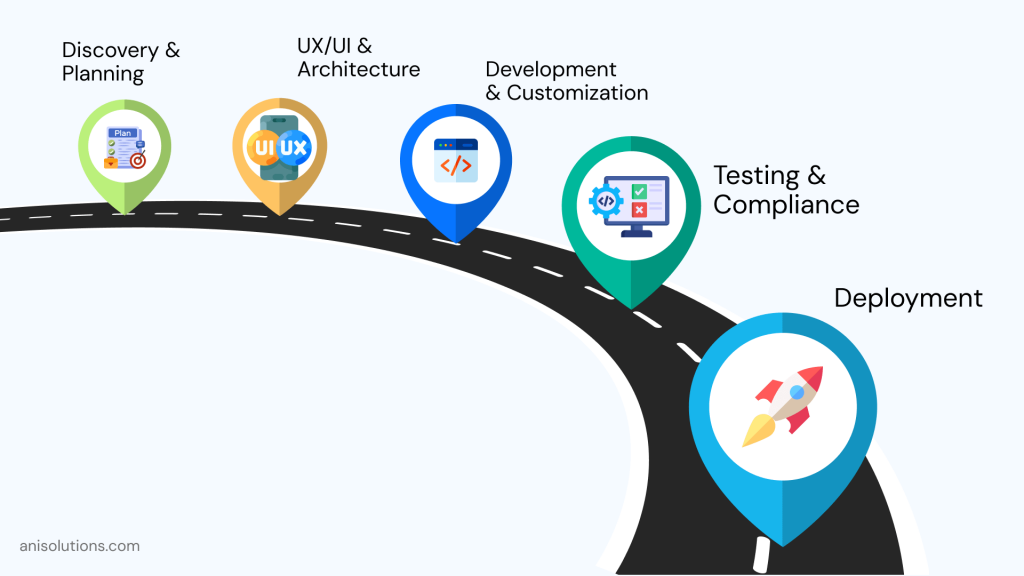
- Typical Phases in an EHR Software Development Timeline
Understanding where time is spent helps explain why EHR timelines vary widely across organizations.
1. Discovery & Planning: This phase starts from workflow analysis and requirement validation, to compliance assessment and technical scoping. Each part needs to have it’s own designated timeframe for the development to proceed on time.2. UX/UI & System Architecture Design: In this phase, time must be allocated for developing responsive interfaces for role-based workflows, prototyping, usability validation, and backend architecture planning.3. Core Development & Customization: With feature implementation, integrations, data handling, and system configuration, you must consider this before planning the development timeline to avoid scope creep later in the development.4. Testing, Compliance & Validation: In this phase, the time must be allocated carefully to test functionality, compliance, and validation of the patient data after migration. If this is rushed, then it can lead to security issues and risk data integrity issues.5. Deployment, Training & Stabilization: This is the final phase of the development process with ongoing time for go-live support, clinician onboarding, performance tuning, and issue resolution.So, if you are delayed in even one phase, then the entire process can extend by weeks or months, inflating the EHR software development timeline and increasing the overall cost of EHR implementation.
- Common Timeline Delays That Escape EHR Cost
Most EHR budget overruns come from a few recurring issues:
1. Incomplete or evolving requirements during the discovery phase2. Late identification of compliance or security gaps3. Underestimated integration complexity4. Data migration challenges from legacy systems5. Delayed stakeholder feedback and approvalsEach of these issues can prolong resource engagement and increase the development cost of EHR systems.
- Why Shorter Timelines Don’t Always Mean Lower Cost
Aggressively compressing timelines can be just as costly as delays because when the steps are rushed, the chances of missing something increase. These shortcuts frequently result in higher post-launch support costs, adoption challenges, and expensive rework, ultimately increasing long-term EHR development costs.
In short, you need a well-planned timeline that balances speed with quality and cost in the long run.
Download the EHR Budget Planner to Avoid Budget Overruns Before You Start
Click HereEstimating the Cost of Developing an EHR System
Another challenging part of EHR planning is estimating the cost of developing an EHR system. The reason is that, unlike general software, the EHRs are shaped by clinical workflows, compliance needs, integrations, and long-term scalability goals. That’s why early numbers often change as projects move from assumptions to execution.
Understanding why estimates vary and what influences them is key to building a realistic EHR development cost breakdown.
- Why Early EHR Cost Estimates Are Often Inaccurate
Initial estimates are usually based on partial information, which most of the time is inaccurate. Moreover, in the discovery phase, many technical and operational details are unclear, leading to optimistic projections and not realistic estimates.
Furthermore, there are some common reasons why early estimates shift, including incomplete or evolving clinical requirements, underestimated integration efforts, compliance scope creep after security reviews, and changes in timeline due to stakeholder feedback or approvals.
These factors directly impact the EHR software development costs even when the original scope appears unchanged.
- EHR Development Cost by System Type
The most effective way to estimate cost is to align expectations with the type of EHR system being built. Below is a high-level comparison to guide planning.
| System Type | Typical Scope | Timeline Range | Estimated Cost Range | Best Fit For |
| MVP EHR | Core charting, scheduling, and basic reporting | 4–6 months | Low to mid six figures | Startups, pilot programs |
| Mid-Scale EHR | Custom workflows, integrations, and compliance-ready | 6–10 months | Mid to high six figures | Growing practices, multi-specialty clinics |
| Enterprise EHR | Advanced analytics, interoperability, scalability | 10–18+ months | Seven figures | Large networks, value-based care models |
These ranges reflect EHR development cost scenarios and should be treated as directional, not fixed pricing.
- One-Time Development Cost vs Ongoing Operational Cost
A common budgeting mistake is focusing only on the build cost while ignoring long-term ownership. The one-time development cost includes costs associated with discovery, planning, and UI/UX design, along with core development and customization.
Moreover, integrations and data migration are one-time development costs where you don’t have to invest continuously. But there are also ongoing operational costs that include hosting, infrastructure, maintenance, support, compliance updates, and security monitoring.
Without investing in ongoing maintenance, the EHR can fail and can’t keep up with the changes in the healthcare landscape. However, if you don’t manage this well over time, these recurring expenses can equal or exceed the initial cost of EHR development.
- Factors That Commonly Change EHR Cost During Execution
Even with careful planning, certain factors frequently impact budgets. Some of the common ones are scope expansion due to new feature requests, additional integrations added mid-project, and unexpected data migration complexity.
By identifying these variables early makes EHR project budget planning far more predictable.
Cost-Saving Strategies Without Compromising Quality

Reducing EHR development cost does not mean cutting corners. In practice, the most expensive EHR projects are often the result of poor sequencing, rushed decisions, and avoidable rework, not overengineering. Effective cost control focuses on building smarter, not cheaper.
Below are proven strategies that help manage the cost of developing an EHR system while maintaining quality, compliance, and long-term ROI:
- Adopt an MVP-First Development Approach
An MVP-first strategy is one of the most reliable ways to control early-stage EHR software development costs. Rather than building feature-heavy systems upfront, teams focus on essential clinical workflows, core documentation, and compliance-ready foundations.
This approach:
1. Limits initial scope and investment2. Accelerates go-live timelines3. Enables real-world validation before scalingOrganizations that skip MVP planning often overspend early and still face redesigns later, increasing overall EHR development costs.
- Prevent Rework Through Strong Upfront Decisions
One major but invisible cost driver is rework because poorly defined requirements, rushed UX decisions, or late compliance changes force teams to rebuild core components. So, investing time in discovery, workflow mapping, and technical validation significantly reduces the development cost of EHR systems by avoiding downstream corrections and timeline extensions.
- Leverage Pre-Built EHR Software Modules Strategically
Not every feature needs to be built from scratch or custom-built. Using pre-built EHR software modules for standard functionality, such as scheduling, audit logs, or basic reporting, can substantially reduce development time and effort.
This strategy:
1. Lowers initial build cost2. Shortens the EHR software development timeline3. Frees resources for high-impact customizationThe key is balancing reuse with customization, where differentiation truly matters.
- Phase Integrations Instead of Building Everything at Once
Integrations are complex and expensive; attempting to connect all external systems upfront often delays launch and inflates the cost of EHR development. A phased integration approach allows teams to prioritize high-value connections first and defer non-critical integrations, making EHR project budget planning more predictable and controlled.
- Design for Scalability from Day One
Cutting costs by ignoring scalability creates expensive problems later. Systems not designed for growth often require re-architecture as usage expands. While scalability planning may slightly increase initial EHR development cost, it significantly reduces the total cost of ownership over time.
Get the EHR Cost Risk Checklist for Preventing Hidden Cost Surprises
Get NowRole of AI in Optimizing EHR Development Cost
AI is often discussed as a feature to add to EHR systems, but its most immediate value lies elsewhere. When applied correctly, AI acts as a cost-optimization enabler, helping teams reduce waste, improve accuracy, and prevent expensive rework across the EHR development lifecycle.
When used strategically, AI can directly influence the EHR development cost breakdown, not by replacing teams, but by making them more efficient and predictable.
- AI-Driven Requirement Analysis & Feature Prioritization
One of the earliest cost risks in EHR projects is an unclear or overextended scope. AI-assisted requirement analysis helps identify overlapping features, low-impact requests, and workflow inefficiencies during discovery.
By analyzing historical project data, clinical workflows, and usage patterns, AI tools can support smarter feature prioritization, ensuring effort is focused where it delivers the most value. This reduces unnecessary build work and lowers the cost of developing an EHR system from the outset.
- AI-Assisted Testing and Quality Assurance
Testing and QA consume a significant portion of EHR software development costs, especially in compliance-heavy environments. AI-driven test automation can accelerate regression testing, identify edge cases, and flag anomalies earlier in the cycle.
This reduces manual testing effort, shortens feedback loops, and prevents late-stage defect discovery, one of the most expensive contributors to extended timelines and rising EHR development costs.
- Predicting Timeline and Cost Risks Using AI Insights
AI models trained on delivery data can help predict timeline slippage and cost escalation risks before they become critical. By analyzing velocity trends, integration complexity, and change frequency, teams gain early warnings of potential overruns.
This allows proactive adjustments such as scope realignment or phased delivery—keeping the EHR software development timeline and budget under control.
- AI as an Enabler, Not Just a Product Feature
The most effective use of AI is often invisible to end users. Rather than rushing to embed AI features into the EHR itself, organizations gain more value by using AI to optimize planning, development, testing, and delivery processes.
This approach improves efficiency without introducing unnecessary complexity or regulatory risk, ultimately lowering long-term EHR development costs.
Measuring Value Beyond Cost: ROI of Custom EHR Development

While focusing on EHR development cost is important, it only gives an incomplete picture. You also need to understand the value an EHR delivers in the long-term. This is where return on investment (ROI) becomes a far more meaningful metric than development cost alone.
Custom EHR systems are designed to align with clinical workflows, operational goals, and long-term growth strategies. By making ROI measurable across both financial and clinical dimensions, you can show the benefits of an EHR system.
- Why Development Cost Alone Leads to Poor Decisions
Organizations that select EHR systems based purely on price often encounter hidden expenses over time. Off-the-shelf solutions may appear economical initially, but limitations around customization, interoperability, and workflow alignment create inefficiencies, workarounds, and recurring operational costs.
Whereas custom EHR systems focus on eliminating friction rather than adapting processes to software limitations. This shift reduces long-term operational strain and improves the overall return on the cost of developing an EHR system.
- Operational Efficiency as a Core ROI Driver
One of the strongest ROI contributors is improved operational efficiency. Custom EHRs streamline documentation, reduce duplicate data entry, and automate routine clinical and administrative tasks.
These efficiencies result in:
1. Reduced clinician documentation time2. Higher patient throughput without increasing staff3. Fewer errors and less rework across care processesOver time, these gains help offset the initial EHR development cost while improving staff satisfaction and productivity.
- Financial & Revenue Cycle Impact
ROI also comes from stronger financial performance. Custom EHRs integrate more seamlessly with billing and reporting workflows, improving charge capture and reducing claim denials. Clean data exchange and accurate documentation support faster reimbursements and better financial visibility.
Additionally, scalable architecture prevents the need for frequent system replacements as organizations grow, protecting long-term investment value.
- Clinical and Strategic Value Over the Long Term
Beyond financial returns, custom EHRs support better care coordination, improved data accessibility, and more consistent clinical decision-making. These benefits enhance patient outcomes and support value-based care initiatives.
From a strategic perspective, owning a custom EHR enables greater control over innovation, integrations, and data strategy—advantages that compound ROI over the system’s lifecycle.
Plan Your EHR Development Timeline with Our EHR Development Guide
Click HereStrategic Budget Planning for Sustainable EHR Development
Successful EHR initiatives are rarely funded with a single, fixed budget. Instead, they rely on phased, flexible budget planning that evolves as requirements, compliance needs, and scalability goals become clearer. Treating EHR development as a one-time capital expense is one of the fastest ways to derail timelines and inflate long-term costs.
Strategic EHR project budget planning focuses on allocation, governance, and sustainability, ensuring the system can grow without triggering repeated reinvestment cycles.
- Why EHR Budget Planning Should Be Phased, Not Fixed
Early estimates are inherently directional. As discovery deepens and integrations, compliance, and data migration requirements surface, budgets must adapt. Phased budgeting allows organizations to commit funds incrementally—aligning spend with validated scope rather than assumptions.
This approach:
1. Reduces financial risk2. Improves cost predictability across phases3. Prevents overcommitting the budget before requirements stabilizePhased planning also supports faster decision-making when priorities shift during development.
- Allocating Budget Across Core EHR Investment Areas
A sustainable EHR budget must balance immediate build needs with long-term operational realities. The table below illustrates how budget allocation is typically structured in well-planned EHR initiatives.
| Budget Area | Typical Allocation Focus | Planning Priority | Risk If Underfunded |
| Core development | Feature build & customization | Immediate | Delivery delays |
| Compliance & security | HIPAA, audits, safeguards | Non-negotiable | Regulatory exposure |
| Integrations | Labs, billing, third-party tools | Phased | Data silos |
| Scalability & architecture | Growth readiness | Strategic | Costly rework |
| Maintenance & support | Post-launch stability | Ongoing | System degradation |
This structure helps leadership visualize where investment is required—and where cutting costs introduces long-term risk.
- Importance of Contingency and Buffer Planning
Unexpected changes are inevitable in EHR projects. Regulatory updates, integration complexity, or data quality issues can quickly impact scope and timelines. Allocating contingency buffers early, rather than reacting later, keeps projects moving without financial disruption.
Well-planned buffers protect delivery momentum and reduce the need for emergency approvals or scope compromises.
- Budget Governance for Long-Term Sustainability
Sustainable EHR budgeting doesn’t end at go-live. Ongoing governance ensures funds are available for enhancements, compliance updates, performance optimization, and user adoption support.
Organizations that treat EHRs as living platforms, rather than completed projects, achieve stronger long-term ROI and avoid repeated reinvestment cycles.
Common Mistakes That Increase EHR Development Cost

Many EHR projects exceed budget not because of technical difficulty, but due to avoidable strategic and planning errors. Understanding these common pitfalls can help organizations control EHR development costs and prevent expensive course corrections later.
- Underestimating Compliance and Security Requirements
Compliance is often treated as a final checkpoint instead of a foundational requirement. Delaying HIPAA safeguards, audit logging, role-based access, or security testing leads to rework and remediation, significantly increasing the development cost of EHR systems. Proactive compliance planning is always less expensive than reactive fixes.
- Ignoring Scalability During Early Development
Building an EHR only for current needs may reduce initial cost, but it creates long-term risk. Systems not designed for growth often require costly re-architecture when patient volume, locations, or data complexity increase. This oversight dramatically inflates the total cost of developing an EHR system over time.
- Choosing Vendors Based Only on Initial Pricing
Selecting development partners solely on low upfront cost often results in poor planning, limited healthcare expertise, and weak compliance practices. These gaps lead to delays, quality issues, and higher long-term EHR software development costs—offsetting any initial savings.
- Treating EHR Development as a One-Time Initiative
An EHR is not a static product. Organizations that fail to plan for ongoing maintenance, compliance updates, and system enhancements often face performance degradation and rising support costs. Sustainable EHR project budget planning accounts for continuous improvement, not just launch.
- Overlooking Integration and Data Migration Complexity
Integrations and legacy data migration are frequently underestimated. Late discovery of interoperability challenges or poor data quality can stall timelines and increase costs rapidly, impacting the overall EHR development cost breakdown.
Avoiding these mistakes doesn’t require more spending, just better planning, realistic expectations, and informed decision-making.
Conclusion: Mastering Your EHR Development Cost Breakdown
Understanding the true EHR development cost breakdown is not about chasing the lowest price. It’s about making informed, strategic decisions that balance quality, compliance, scalability, and long-term value.
As this guide has shown, EHR costs are shaped by far more than development effort alone. Planning depth, timeline management, integration strategy, compliance readiness, and ongoing support all play a critical role in determining total cost and ROI.
Organizations that succeed with EHR development treat it as a long-term platform investment, not a one-time IT project. By identifying cost drivers early, phasing budgets intelligently, and avoiding common pitfalls, healthcare teams can build EHR systems that support growth, efficiency, and better patient outcomes, without constant budget overruns.
If you want to understand how much it will cost you to build your own EHR, click here to book your free consultation with our expert and get clarity tailored to your organization.
Frequently Asked Questions
Q. How much does it typically cost to build a custom EHR system in 2026?
In 2026, a custom EHR system typically costs between mid-six to seven figures, depending on scope, compliance needs, integrations, and scalability. MVP builds cost less, while enterprise-grade systems require higher long-term investment.
Q. What are the primary factors that cause EHR development costs to fluctuate?
EHR development costs fluctuate due to changes in scope, compliance requirements, integration complexity, data migration needs, development timeline extensions, and late-stage feature additions discovered during implementation or testing phases.
Q. Is a custom EHR more cost-effective than an off-the-shelf solution in the long run?
Yes, custom EHRs are often more cost-effective long term by eliminating workflow inefficiencies, reducing recurring license fees, enabling scalability, and avoiding expensive workarounds that off-the-shelf systems typically require.
Q. What is the average cost of ensuring HIPAA and ONC compliance during EHR development?
Compliance costs vary, but HIPAA and ONC readiness typically account for a meaningful portion of development effort, covering security controls, audit trails, testing, and documentation—costs that rise significantly if addressed reactively.
Q. How do third-party integrations (HL7/FHIR) impact the overall EHR project budget?
HL7 and FHIR integrations increase budgets due to data mapping, validation, interoperability testing, and ongoing maintenance. Each additional integration adds complexity, extends timelines, and increases long-term support and monitoring costs.
Q. What percentage of the budget should be allocated for post-launch maintenance and support?
Post-launch maintenance typically requires 15–25% of the initial EHR development cost annually, covering performance monitoring, security updates, compliance changes, user support, and incremental feature enhancements.
Q. How does the choice of development team location affect EHR software development cost?
Development team location impacts cost through labor rates, healthcare domain expertise, time zone coordination, and regulatory familiarity. Lower-cost regions reduce hourly rates but may increase coordination, compliance, or communication overhead if not managed well.
Q. What are the hidden costs of data migration when transitioning to a new EHR system?
Hidden data migration costs include data cleansing, mapping inconsistencies, validation errors, legacy system limitations, compliance safeguards, and extended testing—often leading to timeline delays and unexpected budget increases.
Q. Does integrating AI and machine learning features significantly increase the initial investment?
AI features can increase upfront costs, but using AI for planning, testing, and risk prediction often reduces overall EHR development cost by preventing rework, accelerating timelines, and improving delivery predictability.
Q. How can a practice estimate the ROI of a custom EHR to justify the development spend?
ROI can be estimated by measuring efficiency gains, reduced administrative workload, improved revenue capture, lower long-term licensing costs, scalability benefits, and avoided system replacement—evaluated across the full EHR lifecycle, not just initial spend.
In 2026, a custom EHR system typically costs between mid-six to seven figures, depending on scope, compliance needs, integrations, and scalability. MVP builds cost less, while enterprise-grade systems require higher long-term investment.
EHR development costs fluctuate due to changes in scope, compliance requirements, integration complexity, data migration needs, development timeline extensions, and late-stage feature additions discovered during implementation or testing phases.
Yes, custom EHRs are often more cost-effective long term by eliminating workflow inefficiencies, reducing recurring license fees, enabling scalability, and avoiding expensive workarounds that off-the-shelf systems typically require.
Compliance costs vary, but HIPAA and ONC readiness typically account for a meaningful portion of development effort, covering security controls, audit trails, testing, and documentation—costs that rise significantly if addressed reactively.
HL7 and FHIR integrations increase budgets due to data mapping, validation, interoperability testing, and ongoing maintenance. Each additional integration adds complexity, extends timelines, and increases long-term support and monitoring costs.
Post-launch maintenance typically requires 15–25% of the initial EHR development cost annually, covering performance monitoring, security updates, compliance changes, user support, and incremental feature enhancements.
Development team location impacts cost through labor rates, healthcare domain expertise, time zone coordination, and regulatory familiarity. Lower-cost regions reduce hourly rates but may increase coordination, compliance, or communication overhead if not managed well.
Hidden data migration costs include data cleansing, mapping inconsistencies, validation errors, legacy system limitations, compliance safeguards, and extended testing—often leading to timeline delays and unexpected budget increases.
AI features can increase upfront costs, but using AI for planning, testing, and risk prediction often reduces overall EHR development cost by preventing rework, accelerating timelines, and improving delivery predictability.
ROI can be estimated by measuring efficiency gains, reduced administrative workload, improved revenue capture, lower long-term licensing costs, scalability benefits, and avoided system replacement—evaluated across the full EHR lifecycle, not just initial spend.
- On February 17, 2026
- 0 Comment