
How to Build A Scalable EHR for Multi-Clinic Systems That Grow With You
Over time, when a clinic grows, new clinicians are onboarded, new locations are added, along with the patient volume. On paper, this means success, but the EHR can’t handle this multi-location expansion as each location has its unique workflows, routines, and data formats.
This complexity means the workflows break, patient records are duplicated, and maintaining data access and separation becomes difficult. So, an EHR designed with a single practice in mind can’t support a multi-clinic network.
When it comes to scaling, the most important pillars are standardization and consistency. As with each location, there are new workflows and different processes. That’s why these factors need to be built into a scalable EHR for multi-clinic systems.
This is where a multi-clinic EHR architecture that supports growth with predictable patterns becomes crucial.
In this blog, we will explore how you can build a scalable EHR for multi-clinic systems and how selecting the right EHR software development company improves the chances of success significantly.
Why Standardization Is the Foundation of Multi-Clinic EHRs?
When a healthcare organization expands, adding new locations to the network, there are always some differences. One location’s document visits are in a different way, while the other has a different intake process. At first, these differences seem manageable, but over time, they slow down operations and care delivery.
Oftentimes, this makes it harder for clinicians to adjust to new locations as they have to relearn everything from scratch. It leads to confusion and burnout, and instead of supporting growth, it hinders progress.
This is where standardization becomes crucial to bring consistency and make everything operate exactly the same way in EHR for multiple clinics. The standardization creates core clinical and administrative workflows that all locations follow. However, this still allows flexibility for clinics where it is needed and makes sense.
Moreover, patient records are maintained in a centralized way and are accessible to all clinics in the network. Meaning, patients can visit any location and the treatment will continue without breaking the journey and redoing all the tests, reducing costs and saving time.
Finally, training new staff and clinicians becomes faster, and moving teams between locations is simpler with an established path for scaling. With a standardized foundation, a multi-clinic EHR becomes much more stable and supports scaling efficiently.
In short, a scalable EHR for multi-clinic settings needs standardization as the base for its architecture to be efficient and effective.
Core Architectural Capabilities of a Multi-Clinic EHR
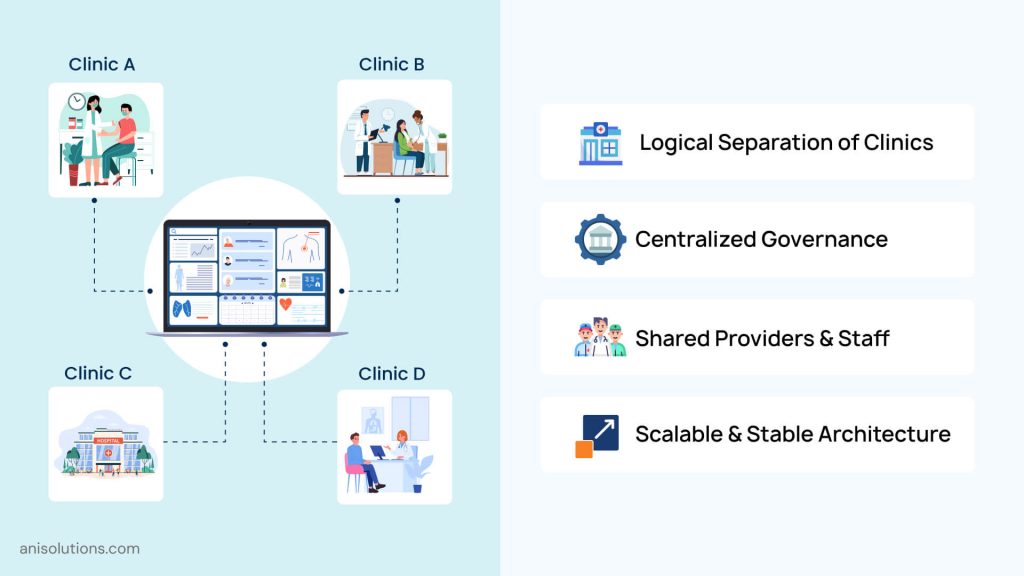
If a healthcare organization wants to grow, it needs a multi-clinic EHR architecture, along with understanding how to scale EHR architecture for multiple clinics. And for all this, there are some critical architectural capabilities that allow multiple clinics to operate within a single system while still keeping it organized, stable, and easy to manage.
- Logical Separation of Clinics:
This is one of the most important architectural capabilities, as it allows multiple clinics to function on the same platform without conflicting. It creates a separate location for schedules, staff assignments, and configuration as per the clinic without needing to separate EHR instances. With this, clinics can use shared infrastructure and data independently.
- Centralized Governance:
A scalable EHR needs to have centralized policies that keep everything working without breaking the balance. You need to define system-wide rules, workflows, and standards to develop a consistent process across locations. But a limited flexibility is also important for local needs. By maintaining this balance, you can ensure expansion does not impact consistency over time.
- Support for Shared Providers & Staff Across Locations:
In multi-clinic settings, clinicians and administrators often work across multiple locations. The multi-clinic EHR must handle this carefully without duplicating user accounts, conflicting permissions, and creating workflow confusion. Without this embedded into the architecture, administrative overhead increases quickly.
- Maintaining System Stability at Scale:
Most of the EHRs are built for a single clinic in mind, so in a multi-clinic EHR, the architecture must be built with predictable performance, meaning that with each new system, the EHR needs to perform the same way. This can be achieved through logical separation and structured data access. Doing this maintains system stability while allowing easier scaling.
While this looks complex to do, this is where an experienced EHR software development company becomes crucial. An experienced partner embeds all these capabilities in the architecture from the start. They clearly understand how to structure clinic hierarchies, data models, and permissions so that adding a new location becomes a simple and low-risk process.
A right EHR architecture from the start gives a clinic a good foundation to scale. Rather than reacting to problems, this allows you to grow confidently in the long term.
Evaluate Your Architecture Capabilities with Our Architectural Framework
Assess NowData Management Challenges When Integrating Multiple Clinics
As clinics grow, managing the data from each location becomes a challenge. And here, understanding which data to share, which is clinic-specific, and how to keep records unified is what determines whether the expansion remains smooth or turns into an operational issue.
The table below explains some of the data management challenges and why it blocks growth:
| Data Challenge | What Happens in Multi-Clinic Systems | Why It Blocks Scaling |
| Shared vs clinic-specific data | Some data needs to be shared across clinics, while other data is location-specific | Poor separation leads to duplication or unintended data exposure |
| Patient record duplication | Patients visiting multiple clinics end up with multiple records | Fragmented records break the continuity of care and reporting |
| Cross-clinic visibility | Clinicians need access to relevant data across locations | Too much access causes confusion; too little limits care coordination |
| Reporting and analytics | Reports pull inconsistent or incomplete data | Leadership loses a reliable view of performance across clinics |
| Data growth over time | Patient and clinical data volumes increase rapidly | Poor data design leads to slow queries and system performance issues |
Designing EHR Architecture That Scales with Growth

When scaling the EHR, it needs to be designed in a repetitive way and in a way that feels like growth, not a disruption. Meaning, while adding a new location should not require complete rework, data restructuring, or workflow optimization each time. So expansion should follow a pattern that architecture already supports.
The first step for this is designing a configuration-driven architecture, not a custom-built one for each new location. If every location needs custom logic or fixes, then scaling becomes slower and riskier with each expansion.
A scalable architecture also supports predictable growth. With this, the systems maintain stability as user numbers, patient records, and clinics grow without compromising performance or reliability. This builds trust and keeps day-to-day operations smooth without clinicians noticing any difference.
More importantly, you must remember that scalability is not a one-time thing; it should be treated as a core capability of EHR. If you try to scale systems before preparing a scalable architecture, then it increases expenses and complexity.
In short, scalability needs to be built into the architecture from the beginning for freedom to grow with technology and expand over time.
Download Our Checklist for Designing Scalable EHR Architecture
Get NowCommon Multi-Clinic Scaling Pitfalls
Even with the right intentions, many healthcare organizations struggle when scaling their EHR across multiple clinics. In most cases, failures don’t stem from a lack of effort; they stem from architectural decisions that don’t account for long-term growth.
- Over-Customizing EHR Behavior for Individual Clinics: When each clinic functions on its own customized workflows, templates, or rules, complexity increases significantly. Over time, maintaining these workflows becomes difficult, and you can’t replicate them, leading to systems that are nearly impossible to scale.
- Tightly Coupling Workflows to Physical Locations: Some EHRs bake location-specific logic directly into workflows. This makes it harder for clinicians to move between clinics and creates friction when new locations are added. As a result, expansion requires more configuration, more training, and more manual oversight.
- Allowing Data Silos to Form During Expansion: As clinics are added quickly, data often becomes fragmented across locations. Patient records, reports, and operational data lose consistency, making it difficult to maintain a single source of information, creating silos.
- Treating Scalability as an Afterthought: Many organizations attempt to scale only after problems appear. This leads to patches, workarounds, and performance fixes that increase technical debt. Most multi-clinic EHR failures come not from growth itself, but from architectural choices made early in development.
So, when you are developing a custom EHR software, always build a scalable architecture rather than retrofitting it later on.
Conclusion: Building an EHR That Grows with Your Healthcare Network
In a nutshell, building a scalable EHR for multi-clinic systems is all about how well the system is designed to handle complexity and manage the data loads. If your EHR architecture is able to manage only a single clinic, you need an expensive or complete overhaul when it’s time to expand.
That’s why the right choice is to build scalability directly into the EHR from the beginning. With this, the expansion becomes predictable, efficient, and far less risky. The result is an EHR that supports long-term growth instead of limiting it.
If you are planning to scale, then click here to book your demo to develop a scalable EHR for a multi-clinic system.
Frequently Asked Questions
Q. What is the best way to manage patient data across multiple clinic locations in a single EHR?
The best approach is to use a unified data model with logical clinical separation. This allows shared patient records while keeping clinic-specific data organized, consistent, and accessible—preventing duplication and ensuring continuity of care across locations.
Q. How can EHR systems maintain consistent performance as clinics and users increase?
Consistent performance comes from a scalable architecture that distributes system load, isolates clinic activity, and handles growing data volumes efficiently. When growth is planned for upfront, adding clinics doesn’t slow down everyday clinical workflows.
Q. Why is a unified patient index critical for multi-clinic and multi-specialty medical groups?
A unified patient index ensures each patient has a single, accurate record across all clinics and specialties. This prevents duplicate charts, improves care coordination, and gives clinicians a complete view of patient history regardless of location.
Q. What are the biggest challenges when integrating a new clinic into an existing EHR system?
The biggest challenges include aligning workflows, mapping data correctly, managing user access, and maintaining consistency without disrupting existing clinics. These issues are often amplified when the EHR wasn’t originally designed for multi-clinic growth.
Q. Can a single EHR support different clinical workflows across multiple clinic locations?
Yes, a well-designed EHR can support different workflows through configurable settings rather than custom code. This allows clinics to adapt processes locally while still following standardized structures across the broader healthcare network.
Q. How does scalable EHR architecture reduce operational complexity for growing healthcare networks?
Scalable architecture simplifies growth by making clinic onboarding repeatable, reducing manual work, and keeping data and workflows consistent. This lowers administrative overhead, minimizes errors, and allows teams to focus on care instead of system management.
The best approach is to use a unified data model with logical clinical separation. This allows shared patient records while keeping clinic-specific data organized, consistent, and accessible—preventing duplication and ensuring continuity of care across locations.
Consistent performance comes from a scalable architecture that distributes system load, isolates clinic activity, and handles growing data volumes efficiently. When growth is planned for upfront, adding clinics doesn’t slow down everyday clinical workflows.
A unified patient index ensures each patient has a single, accurate record across all clinics and specialties. This prevents duplicate charts, improves care coordination, and gives clinicians a complete view of patient history regardless of location.
The biggest challenges include aligning workflows, mapping data correctly, managing user access, and maintaining consistency without disrupting existing clinics. These issues are often amplified when the EHR wasn’t originally designed for multi-clinic growth.
Yes, a well-designed EHR can support different workflows through configurable settings rather than custom code. This allows clinics to adapt processes locally while still following standardized structures across the broader healthcare network.
Scalable architecture simplifies growth by making clinic onboarding repeatable, reducing manual work, and keeping data and workflows consistent. This lowers administrative overhead, minimizes errors, and allows teams to focus on care instead of system management.
- On February 5, 2026
- 0 Comment


