
Integrating with the Top 5 EHR Platforms: A Side-by-Side Technical Comparison
FHIR API adoption has grown significantly, nearly reaching 70%, as per the Office of the National Coordinator for Health IT (ONC). But adoption is not the same as standardization in system integration.
Yet, many healthcare organizations assume that the adoption of FHIR APIs means a standardized integration process.
Although FHIR was designed to make this possible, we are not quite there yet.
While major EHR platforms such as Epic, Oracle Cerner, and athenahealth support a modern, API-driven ecosystem, the reality changes when developers step into implementation.
They find:
- Different API architectures across different vendors.
- Inconsistent FHIR implementation.
- Restricted access models and onboarding processes.
- Long approval cycles and certification requirements.
All of this turns what developers thought of as a technical integration into a multi-layered operational challenge with compliance, vendor policies, and workflow alignment. And the real challenge is not standard availability, it is how standards such as FHIR are implemented in different EHRs.
To solve this issue, it is important to understand how these platforms differ when it comes to integrating with them.
Whether it is Epic, Cerner, or athenahealth, every EHR platform is designed differently with its own workflows and integration model. That’s why, only looking at any one platform is not going to answer the question.
So, this EHR integration platforms comparison guide takes a different approach. We will break down the differences with a side-by-side technical and strategic comparison of top EHR vendors.
By the end of this, you will have an understanding of how to integrate with top EHR platforms like Epic, Cerner, and athenahealth, along with how to approach EHR interoperability with a realistic, future-ready mindset.
Because integration is no longer only a feature—it’s the foundation for modern healthcare ecosystems.
How to Evaluate EHR Integration Platforms?
As I said in the introduction, not all EHR platforms are integrated the same way. That’s why it’s important to have a clear evaluation framework before we dive into the EHR integration platform comparison.
While evaluating EHR integration platforms, there are four core criteria that you should look for:
| Criteria | What to Evaluate | Why It Matters |
| API Architecture | FHIR R4 (HL7), HL7 v2, REST vs proprietary APIs | Determines integration flexibility, scalability, and long-term interoperability |
| Developer Experience | Sandbox access, documentation, SDKs, and onboarding process | Directly impacts development speed, cost, and time-to-market |
| Data Accessibility | Clinical and financial data access, FHIR resource coverage (Patient, Observation, Encounter, etc.) | Enables real-world use cases like care coordination, analytics, and automation |
| Security & Compliance | OAuth 2.0, SMART on FHIR scopes, HIPAA, USCDI | Ensures secure data exchange and alignment with regulatory requirements |
These four criteria are the foundation of a successful EHR integration.
- API Architecture: This decides how easily a system can connect and scale over time. Because even if the systems support EHR interoperability standards, how they implement them is completely different, along with integration workflows.
- Developer Experience: If the developer experience, such as access to a sandbox, proper documentation, and an onboarding process, impacts the development timeline and cost. And this changes with each EHR vendor creating different development environments and costs.
- Data Accessibility: Without easy data availability and accessibility, the integration is not successful. However, while most EHR platforms use FHIR APIs, the data depth and access levels differ, limiting the accessibility and immediate usability of data.
- Security & Compliance: Most EHR platforms support security and compliance through OAuth 2.0 authentication, SMART on FHIR authorization, and HIPAA. They differ in scope, token management, and data-sharing permissions.
In short, although many EHR platforms support FHIR APIs, it is important to evaluate how they do it by checking their implementation standards, access controls, and accessibility to data. Without evaluating these criteria, organizations may underestimate the integration complexity, leading to costly and lengthy implementations.
EHR Integration Evaluation Checklist
Download NowTechnical Comparison: A Top EHR Vendors Side-by-Side Breakdown
After understanding the evaluation criteria, the next step is applying them in the real-world context. When we apply it to the top EHR vendors, the difference between them becomes clear for actual implementation.
Here is a quick snapshot of the top EHR vendors comparison for API architecture, FHIR depth, developer access, and overall integration experience:
| Platform | API Type | FHIR Depth | Sandbox Access | Performance | Best Fit |
| Epic Systems | Controlled FHIR APIs + proprietary | High (with custom profiles) | Limited, approval-based | Moderate | Enterprise hospitals |
| Oracle Cerner | Hybrid (FHIR + proprietary Millennium APIs) | Medium–High | Available but varies | Moderate | Large health systems |
| athenahealth | REST + FHIR APIs | High | Strong, developer-friendly | High | Cloud-first practices |
| eClinicalWorks | Mixed (FHIR + legacy APIs) | Medium | Limited | Moderate | Mid-sized clinics |
| NextGen Healthcare | Mixed APIs | Medium | Limited | Moderate | Ambulatory care |
In healthcare, one of the biggest misconceptions is that FHIR creates a standardized experience. For instance, Epic has deep support; however, it heavily relies on controlled access and custom extensions.
Whereas, athenahealth API integration provides a more standardized and developer-friendly experience. That’s why a technical comparison of EHR FHIR APIs, Epic vs Cerner vs athenahealth, is essential.
Because in practice, integration success depends more on how each platform implements them than on standards.
The Enterprise Tier: Epic, Oracle Health, & Athenahealth
In the top EHR vendors for enterprise-level integration, Epic Systems, Oracle Cerner, and athenahealth are the biggest players. However, each vendor offers a different API architecture, interoperability, and developer experience. Here is how each system differs:
Epic Systems: The Enterprise Benchmark
In all the EHR platforms, the biggest share is held by Epic Systems, making Epic FHIR API integration one of the most essential for enterprise healthcare environments. Its integration is built around a controlled developer environment (App Orchard) with tight control for APIs, documentation, and production systems.
Moreover, it works on FHIR R4 and highly structured clinical data, ensuring consistency across workflows. However, there are some cons also, such as formal onboarding, approvals, and strict adherence to vendor guidelines.
Additionally, Epic uses custom FHIR profiles and extensions, meaning developers have to adapt to implementation standards to fit Epic’s ecosystem.
Strengths:
- High data consistency and structured clinical workflows.
- Scalable for enterprise hospital systems.
- Strong governance and security.
Limitations:
- Restricted API access and sandbox availability.
- Longer onboarding and certification cycles.
- Vendor-controlled integration model.
Oracle Health (Cerner): The Millennium Platform
Another EHR vendor is Oracle Health, previously known as Cerner. The biggest advantage of this platform is its flexible integration compared to Epic. The Cerner Millennium API integration makes it easy to combine FHIR APIs with legacy standards such as HL7 v2, creating a hybrid architecture.
This hybrid architecture allows developers more flexibility to build modular integrations and access a wider range of data sources. One more advantage is that Cerner provides a more accessible sandbox environment, enabling faster development cycles.
But this platform also has a trade-off in consistency, as FHIR implementation varies across deployments, creating variability in performance and API behavior.
Strengths:
- Flexible API ecosystem with hybrid integration options.
- More accessible developer onboarding and sandbox environments.
- Supports modular and scalable development.
Limitations:
- Inconsistent API behavior across implementations.
- Variability during platform transition to Oracle infrastructure.
- Additional complexity due to the hybrid architecture.
Athenahealth: The Cloud-Native Platform
When it comes to athenahealth, the cloud-based architecture makes it more developer-friendly than both Epic and Oracle Health. The athenahealth API integration is also much faster and more accessible than traditional enterprise systems.
Additionally, it supports REST and FHIR APIs strongly, along with having strong documentation for patient portals and an easier onboarding process. This makes it a preferred choice for digital health companies and SaaS platforms that want a quick-to-scale EHR platform.
One more strong suit of Athenahealth is workflow automation and real-time data exchange. However, when compared to Epic, it may require additional considerations for handling highly complex enterprise workflows.
Strengths:
- Developer-friendly APIs and faster onboarding.
- Strong support for REST and FHIR standards.
- Ideal for cloud-first and scalable applications.
Limitations:
- May require adaptation for complex enterprise use cases.
- Less control compared to tightly governed systems like Epic.
When you compare these top EHR vendors side-by-side, it becomes clear that there is no one-size-fits-all solution.
- Epic focuses on control and data consistency.
- Cerner balances flexibility with complexity.
- Athenahealth emphasizes speed and developer experience.
For healthcare organizations, it is important to understand how each system’s architecture, governance, and API strategy align with integration goals. Because the success of how to integrate with top EHR platforms like Epic, Cerner, and athenahealth depends on how each platform implements and controls it.
Epic vs Cerner vs Athenahealth: Integration Comparison Sheet
Get NowThe Mid-Market Layer: eClinicalWorks & NextGen
While in large enterprises, health systems Epic, Cerner, and athenahealth dominate, there are also a significant number of ambulatory and mid-sized clinics using eClinicalWorks and NextGen Healthcare.
However, here also, these systems integration requirements and interoperability capabilities are different. Let’s have an overview of how they work:
- Integration Across Ambulatory Systems
The mid-market platforms do not have their own custom APIs most of the time, and they often evolve through a mix of FHIR APIs and legacy standards such as HL7 v2. As a result, eClinicalWorks NextGen EHR integration includes working with a mix of FHIR APIs, legacy HL7 v2 interfaces, and partially documented APIs. This leads to fragmented integration with a lack of standardization.
- Variability in API Maturity & Interoperability
Both eClinicalWorks and Next Gen Healthcare support EHR interoperability standards, but the maturity and consistency of implementation might differ. The FHIR support may be limited to specific resources, and API documentation may not be complete, along with restrictions on using sandbox environments. However, these systems may offer quicker access, but healthcare organizations have to manage inconsistencies more frequently.
- Role of CommonWell & Carequality Networks
The CommonWell Health Alliance and Carequality are frameworks to exchange data across providers. eClinicalWorks and Next Gen Healthcare use it to close gaps in interoperability and enable data exchange beyond the range of their APIs. But these frameworks are not full system integration but act as a bridge to retrieve patient data and don’t replace the API-based integration.
- Challenges in Data Consistency & Standardization
The key limitation in mid-market integration is data variability along with differences in data mapping, coding standards, and FHIR resource coverage. And these limitations can lead to inconsistencies across the system, impacting care coordination, reporting accuracy, and scalability of digital health solutions.
In short, mid-market EHR vendors have an advantage in flexibility and accessibility; however, the trade-offs are consistency and standardization. If you implement these solutions, then the challenge is to balance faster onboarding with effective data normalization and interoperability.
Multi-EHR Integration Architecture
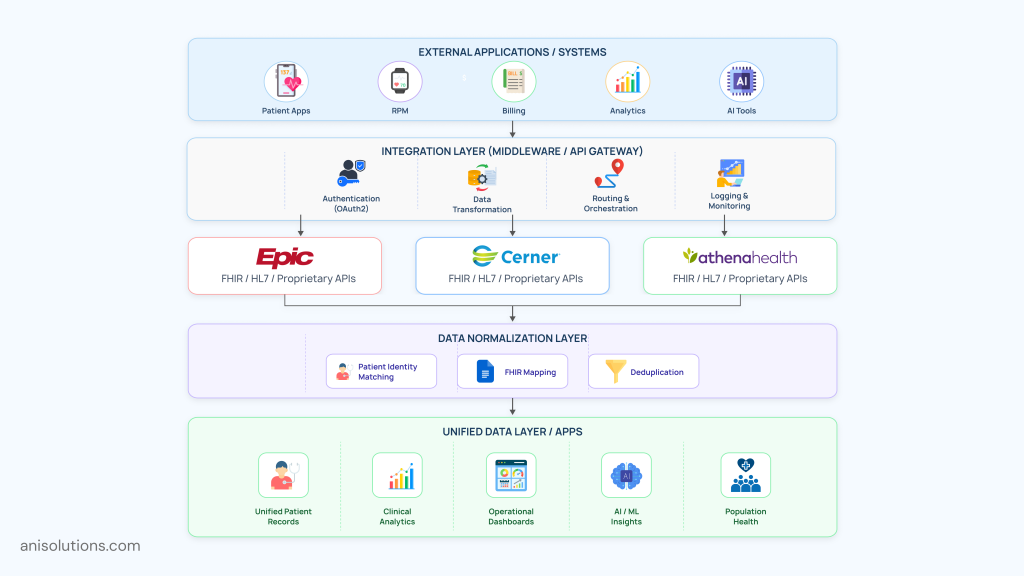
In the modern healthcare landscape, it is not enough to integrate with any one EHR vendor. With the increasing need for connecting with AI-driven tools and analytics, RPM tools need to work across multiple systems for better results.
And that’s what multi-EHR integration architecture helps with: it connects different systems, including Epic, Cerner, and athenahealth, through a centralized integration layer. If you use it, the need for separate integrations for each platform is eliminated.
The integration layer alone handles all patient authentication, routing to the right EHR, and data transformation, enabling seamless connection with external applications.
However, it is not a flawless solution as there are challenges while handling patient identity authentication. Moreover, the data from different systems must be routed carefully to be used meaningfully in a unified storage.
Additionally, aligning data with each system’s EHR interoperability standard is not possible without proper data normalization. If this is not done carefully, it can lead to inconsistencies and unusable data.
Most importantly, the multi-EHR integration approaches must be adapted as per the scale, complexity, and use cases of the healthcare organization and EHR systems. Here is a snapshot of the approaches:
| Approach | Description | Best Use Case |
| Middleware | Central integration engine (e.g., interface engines) handling data transformation and routing | Legacy + hybrid environments with HL7 and FHIR |
| API Gateway | Unified API layer managing authentication, access control, and orchestration | Scalable, modern healthcare platforms |
| Event-Driven Architecture | Real-time data streaming using events and messaging systems | Analytics, automation, and real-time decision support |
What many healthcare organizations do is treat each EHR integration separately; multi-EHR integration architecture shifts this approach. It unifies multiple EHR integrations into a single integration layer, reducing duplication, improving scalability across platforms, enabling consistency across platforms, and supporting advanced use cases such as AI.
2026 Readiness: Future-Proofing EHR Integration
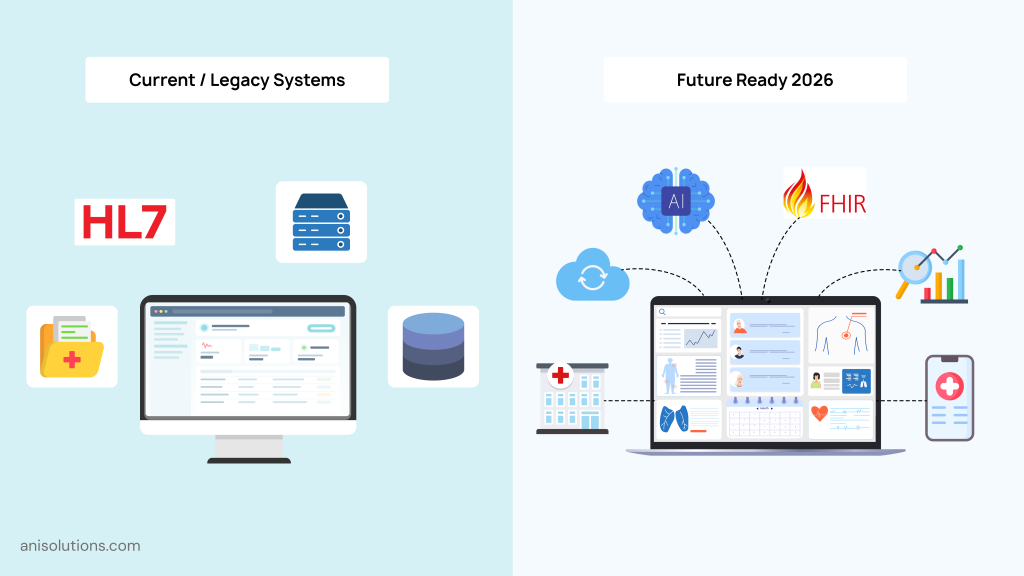
The healthcare landscape is always changing, and EHR integration is rapidly evolving with new standards and emerging technologies. A decade ago, HL7 v2 was the best EHR interoperability standard for healthcare data exchange.
However, today, FHIR APIs have become the best solution for exchanging patient data. That’s why healthcare organizations must design EHR integration that not only meets current requirements but is also ready for future changes to stay competitive in this evolving healthcare integration.
- Compliance & Emerging Standards
One of the fastest-changing parts of healthcare is compliance and EHR interoperability standards. These standards are designed to improve interoperability and data accessibility, and USCDI is one such rapidly changing standard. There are new versions of USCDI that define data elements to exchange, and USCDI v4 adds expanded clinical classes and improved data standardization across care settings. For organizations, this means readying systems to adopt expanding datasets and evolving standards without repeated reworks.
- Scalable Integration Strategy
Another future consideration is supporting real-time APIs and batch data processing without compromising performance. These two handle two different functions. The real-time APIs enable instant clinical updates and care coordination, whereas batch processing handles reporting and population health management. An integration strategy needs to ensure that systems are built in a way that allows for adjustments to these two components.
- Designing for Advanced Use Cases
In current healthcare, the decision-making process is dependent on predictive analytics, AI-driven CDS, and automated workflows. To support these use cases, the integration architecture must provide consistent and normalized data, enabling event-driven data flows. This is where multi-EHR integration architecture becomes essential.
- Developer Considerations
For healthcare organizations to keep pace with the evolving healthcare landscape, the developers must quickly adapt to changing APIs, standards, and vendor ecosystems. Best practices from an EHR integration developer guide for healthcare systems include:
- Designing integration with modularity and abstraction layers.
- Avoiding vendor lock-in through standardized interfaces.
- Monitoring API changes and version updates, especially FHIR releases.
- Building for scalability and maintainability, not just immediate functionality.
However, future-proofing EHR integration does not mean predicting every change, but building systems that can adapt to change and scale without compromising interoperability.
EHR Integration Strategy Guide (2026 Ready)
View NowConclusion: Choosing the Right EHR Integration Strategy
The healthcare integration is deeper than just selecting one EHR vendor and connecting systems with them. Every EHR platform has a different integration model, EHR interoperability standards, and developer experience.
To build a successful integration, you need to understand how each system works and then adjust the implementation strategy to adapt to that platform. If you consider the differentiating interoperability requirements the same for EHR platforms such as Epic, Cerner, and athenahealth, then the risks of integration failure increase.
Moreover, the integration models and standards do not remain the same; they evolve over time. And only healthcare organizations that build systems that are able to adapt to these changes quickly and efficiently are going to thrive in the modern healthcare environment.
At A&I Solutions, we understand how to integrate with top EHR platforms like Epic, Cerner, and athenahealth, and even unify them with a multi-EHR integration architecture to improve interoperability and data accessibility.
So, if you want to use multiple EHR platforms without the hassle of managing separate integrations, then connect with us and let’s build your multi-EHR integration.
Frequently Asked Questions
An EHR integration platform is a middleware layer that connects healthcare applications with EHR systems. It manages APIs, data transformation, authentication, and routing. Instead of building separate integrations for each EHR, it provides a unified interface that enables scalable, secure, and efficient data exchange across multiple healthcare systems.
Focus on API architecture (FHIR, HL7), developer experience (sandbox, documentation), data accessibility, and security compliance. Evaluate how each platform implements standards, not just whether it supports them. These factors determine integration complexity, scalability, and the effectiveness with which systems support real-world clinical and operational workflows.
Epic Systems offers deep but controlled FHIR APIs with custom profiles. Oracle Cerner provides a hybrid approach with variable implementation. athenahealth delivers more standardized, developer-friendly APIs with easier access, making integration faster but sometimes less enterprise-focused.
Key standards include FHIR (modern API-based exchange), HL7 v2 (legacy messaging), and SMART on FHIR for authentication. USCDI defines required data elements. Together, these standards enable structured data exchange, though implementation varies across EHR vendors.
Epic FHIR API integration operates within a controlled ecosystem that requires onboarding via App Orchard. Developers access structured clinical data using FHIR APIs, often with custom extensions. While highly scalable and secure for enterprise workflows, integration involves approvals, certification, and strict compliance with Epic’s governance model.
Cerner Millennium API integration involves a hybrid architecture combining FHIR and proprietary APIs. Challenges include inconsistent API behavior across deployments, variability in data mapping, and complexity during the Oracle cloud transition. While flexible, developers must manage multiple integration layers and adapt to evolving platform changes.
Athenahealth API integration is considered developer-friendly due to its REST-first architecture, strong FHIR support, and accessible developer portal. It offers faster onboarding, better documentation, and easier access to sandboxes. This reduces development time and complexity, especially for SaaS and cloud-based healthcare applications.
A multi-EHR integration architecture connects multiple EHR systems through a unified integration layer. It is needed when applications must work across different platforms, such as Epic, Cerner, and Athenahealth. This approach enables data normalization, scalability, and consistent workflows across diverse healthcare environments.
Use a centralized integration layer such as middleware or an API gateway. This layer handles authentication, data transformation, and routing across EHR systems. Standardizing data using FHIR and implementing normalization ensures consistent outputs, enabling a single system to interact with multiple EHR platforms efficiently.
Although all major vendors support FHIR, implementations differ in resource coverage, custom profiles, and access controls. Some platforms restrict endpoints or extend standard resources, while others offer broader access. These differences affect integration complexity, data consistency, and the ease with which applications can scale across systems.
A technical comparison highlights differences in API structure, access models, and FHIR implementation depth. It helps organizations assess integration effort, scalability, and developer experience. This ensures platform selection aligns with technical requirements, reducing risk and improving long-term interoperability outcomes.
EHR API integrations must comply with HIPAA, OAuth 2.0 authentication, and SMART on FHIR authorization. Standards like USCDI ensure data consistency. Additionally, audit logging, access controls, and encryption are essential to maintain secure and compliant healthcare data exchange.
- On April 23, 2026
- 0 Comment


