How to Integrate Telehealth, Labs, & Billing with Your EHR: A Workflow-First Approach
Have you heard of a “Toggle Tax”?
Well, even if you haven’t heard of it, you might have already experienced or paid for it in some way. To explain it simply, it is constant switching between different tabs on your EHR. For example, a primary care physician finishes a virtual encounter, switches tabs for reviewing notes, and opens another tab for billing.
This repeated toggling is the toggle tax I am talking about, and the price for this is clinician burnout, missed data, and delayed care decisions. However, the reason for this is not a lack of proper technology, but fragmentation.
When any healthcare organization connects different tools such as labs, telehealth, and billing systems, most of the time, they don’t integrate workflows. And this leads to silos instead of creating a unified workflow.
Because of this, the clinical decisions are delayed, documentation becomes inaccurate, billing workflows get disconnected, and patient experience suffers.
Moreover, traditional EHR integration strategies focus on data exchange and making the system interoperable with FHIR and HL7 standards. Although this is necessary, it only solves half of the problem.
The data flows, but the workflows don’t connect. Meaning, a lab result might reach the EHR, but if the next step, such as clinical review or billing, it becomes noise instead of insights. And this is where the workflow-first EHR integration strategy changes the equation.
In this EHR workflow integration guide, we will break down how to integrate telehealth, labs, and billing with EHR and a step-by-step strategy to turn a disconnected healthcare ecosystem into a truly connected ecosystem.
Because today’s systems don’t need to just exchange data but do it seamlessly, intelligently, and in real time.
The Strategic Blueprint: Designing an EHR Workflow Integration Guide
The real challenge in integrating is not just connecting systems, but designing it for a workflow-first approach. As I said in the introduction, while connecting systems is important, it is also crucial to match the workflows.
However, a workflow-first EHR integration strategy changes as it helps seamlessly integrate telehealth, labs, and billing systems to your EHR. This strategy changes the question from How do we connect systems? To
How should care flow across systems? This is where an effective EHR workflow integration guide comes into the picture.
And this is possible because of a hub-and-spoke architecture, which makes the EHR a central hub. Whereas, modules such as labs, revenue cycle, patient portals, and medical devices act as spokes, connected through FHIR APIs, HL7 ORM/ORU, and middleware.
This transforms the EHR from a data repository to an active workflow engine coordinating clinical and operational actions. Here, each module represents a critical stage in the care journey:
| Module | Purpose | Key Outcome |
| Telehealth | Virtual care delivery | Faster consultations |
| Labs | Diagnostics automation | Faster clinical decisions |
| Revenue Cycle | Billing workflows | Improved cash flow |
| Patient Portal | Patient engagement | Better transparency |
| Devices | Continuous monitoring | Preventive care |
The biggest advantage is healthcare workflow automation. For example, when a telehealth encounter ends, the notes are generated automatically, patient records are updated, and billing claims are triggered, without any manual actions.
However, for a successful integration, you need to identify workflow gaps across processes, including intake, care delivery, and billing. If you fail to map the bottlenecks, it can lead to delays, errors, and revenue leakage in the long-run.
This is where a scalable integration blueprint with API-first design and standardized data models comes in. It helps in integrating AI tools, RPM devices, or third-party apps seamlessly without disrupting existing workflows.
Telehealth EHR Integration: The Digital Front Door
Today, most of the time, care happens virtually, and telehealth tools have become the digital front door for patients. However, in many healthcare organizations, we have worked with telehealth tools that are still treated as standalone tools, and this is where the real issue is.
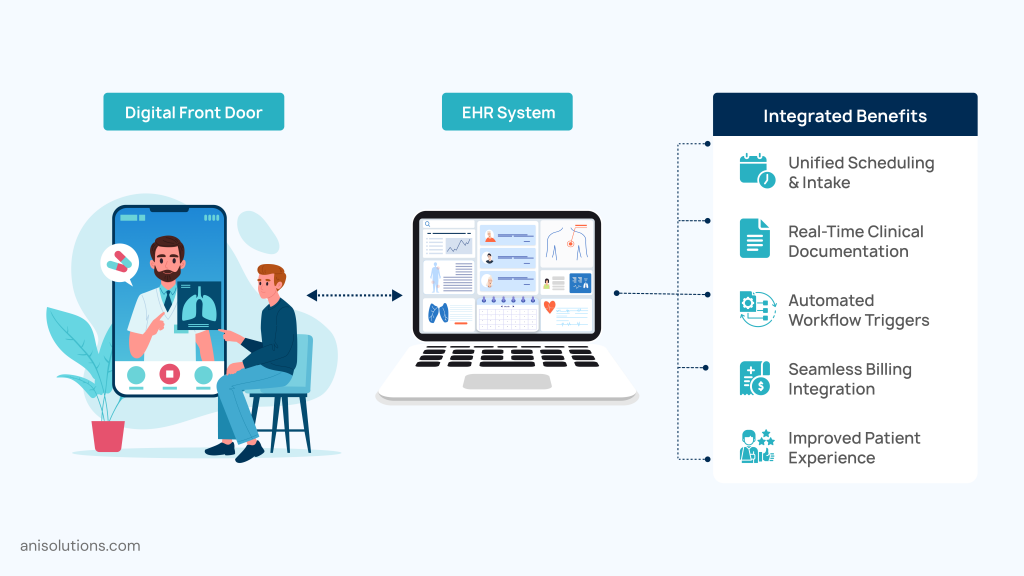
And a well-designed telehealth EHR integration ensures that fragmentation is eliminated by embedding virtual care directly into the EHR workflows. Here’s how this helps in changing the integration:
- Unified Scheduling & Patient Intake: Appointments booked through telehealth platforms are automatically synced with the EHR, ensuring accurate patient records and reducing duplicate data entry.
- Real-Time Clinical Documentation: Notes from virtual consultations are captured and stored directly within the patient’s EHR, often enhanced by AI-driven summarization tools.
- Automated Workflow Triggers: The end of a consultation can trigger follow-up actions such as lab orders, prescriptions, care plan updates, or referral workflows, without manual intervention.
- Seamless Billing Integration: Encounter data flows directly into revenue cycle systems, enabling automated CPT code capture, claim generation, and reimbursement workflows.
- Improved Patient Experience: Patients experience a smoother journey, with fewer delays, better communication, and consistent access to their health information.
With this strategy, you can ensure workflow continuity as a virtual visit is no longer an isolated event. This connects the entire care journey from diagnosis, treatment, and billing.
Lab EHR Integration: The Insight Engine
If telehealth is the entry point, then labs are where evidence-based clinical decisions are taken. Yet, many healthcare organizations’ lab workflows are fragmented, leading to delayed and inaccurate care decisions.
However, lab EHR integration provides a structured way to streamline lab results and create actionable insights at the point of care. It eliminates the fragmentation, longer turnaround times, missed follow-ups, and increased risk of clinical errors.
It uses the HL7 message standards to integrate systems, especially:
- ORM (Order Messages): Used to send lab test orders from the EHR to lab systems.
- ORU (Observation Result Messages): Used to return lab results back into the EHR.
This creates a closed-loop workflow if implemented successfully:
- A provider orders a lab test directly within the EHR.
- The order is transmitted instantly to the lab system.
- Results are processed and sent back automatically.
- Data is structured and attached to the patient’s record in real time.
By following this process, you can eliminate manual data entry, reduce data entry, reduce duplication, and ensure that patient data is updated and accessible. Moreover, it enables workflow automation and prioritization.
- Abnormal result flagging ensures critical values are highlighted immediately.
- Automated alerts and tasks trigger follow-ups, repeat testing, or care plan updates.
- Decision support integration helps providers act faster with contextual insights.
As a result, diagnosis becomes faster, reduces administrative workload, and improves patient safety and outcomes. Most importantly, turns EHRs into an active insight engine that turns clinical data into timely actionable insights.
Revenue Portal FHIR Integration: The Engagement Loop
Another essential integration is billing systems for streamlining revenue cycles and improving financial stability. However, we have seen that healthcare organizations fail to integrate billing workflows into clinical workflows, leading to repeated claim rejection and revenue leakage due to incorrect data.
Without a structured revenue cycle EHR integration, this gap widens, but with a workflow-first approach changes this by integrating clinical events to financial workflows in real-time. This ensures that every encounter automatically triggers revenue cycle actions.
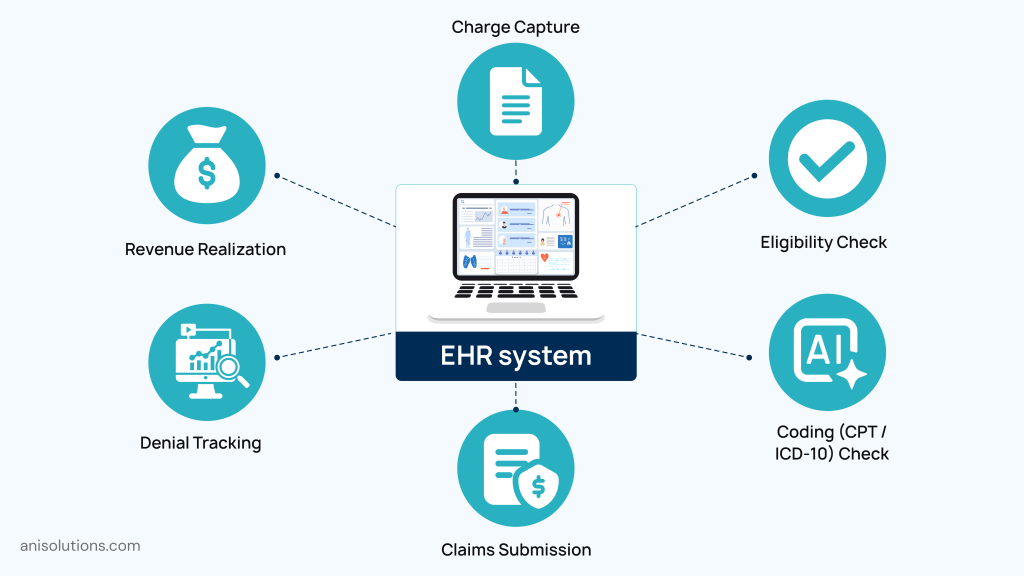
Here’s what it looks like:
- Automated Charge Capture: Procedures, diagnoses, and services documented in the EHR are instantly translated into billable events.
- Real-Time Eligibility & Benefits Verification: Patient coverage is validated during intake or scheduling, reducing claim rejections later.
- Intelligent Coding Support: Systems can suggest CPT and ICD-10 codes based on clinical documentation, improving accuracy and compliance.
- Automated Claims Submission: Clean claims are generated and submitted without manual intervention, accelerating the billing cycle.
- Denial Prevention & Tracking: Built-in validation checks catch errors before submission, while analytics help identify recurring denial patterns.
The key shift is synchronization. When clinical documentation, coding, and billing workflows are connected, there’s no lag between care delivery and revenue realization.
This doesn’t just improve cash flow—it also reduces the burden on staff, minimizes compliance risks, and ensures that providers are accurately reimbursed for the care they deliver.
Because in modern healthcare, efficiency isn’t just about better care delivery, it’s about making sure that care is captured, coded, and compensated without friction.
Patient Portal FHIR Integration: The Engagement Loop
If telehealth opens the door and labs drive decisions, the patient portal is what keeps patients connected throughout the care journey. Yet in many healthcare systems, patient portals remain underutilized—not because they lack features, but because they’re poorly integrated into clinical workflows.
Without effective patient portal FHIR integration, patients experience fragmented access:
- Delayed visibility into lab results or visit summaries
- Limited communication with providers
- Manual processes for scheduling, payments, or follow-ups
This creates frustration for patients and adds unnecessary workload for administrative staff.
A workflow-first approach transforms the patient portal into an active engagement layer, tightly connected to the EHR through FHIR-based APIs. Instead of acting as a passive interface, the portal becomes a real-time extension of the care workflow.
Here’s how that shift plays out:
- Real-time access to health data: Patients can view lab results, medications, visit notes, and care plans as soon as they are available in the EHR.
- Seamless appointment management: Scheduling, rescheduling, and reminders are fully synchronized with clinical systems, reducing no-shows and manual coordination.
- Secure communication channels: Messaging between patients and providers is integrated into the clinical workflow, ensuring conversations are documented and actionable.
- Self-service capabilities: Patients can complete intake forms, update demographics, and make payments without staff intervention, reducing administrative burden.
- Personalized engagement: Automated reminders, follow-ups, and care recommendations can be triggered based on patient data and clinical events.
The key advantage is continuity. Patients are no longer passive recipients of care—they become active participants in an ongoing, connected experience.
From an operational standpoint, this reduces call volumes, minimizes paperwork, and improves efficiency. From a clinical perspective, it enhances adherence, communication, and overall outcomes.
Medical Device EHR Integration: The Continuous Care Layer
Care doesn’t end when a patient leaves the clinic—and that’s exactly where most traditional systems fall short. Between visits, there’s often zero visibility into a patient’s condition, especially for those with chronic diseases. This gap is where medical device EHR integration becomes critical.
With the rise of wearables, remote monitoring tools, and IoT-enabled devices, healthcare organizations now have access to continuous streams of patient-generated health data—from heart rate and blood pressure to glucose levels and activity patterns. But without proper integration, this data remains isolated, overwhelming, or clinically unusable.
A workflow-first approach ensures that device data is not just collected—but embedded into actionable clinical workflows.
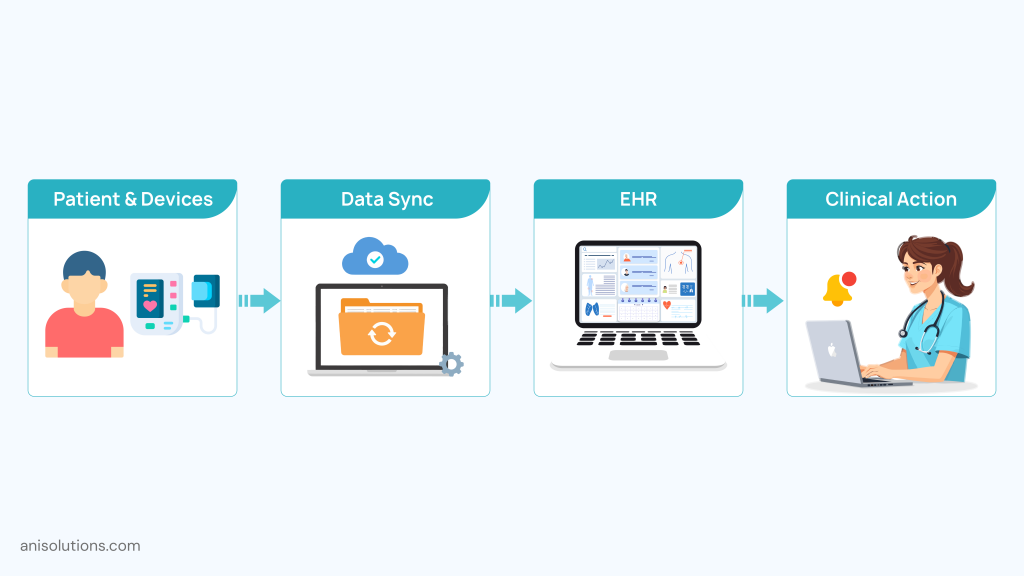
Here’s how effective medical device EHR integration transforms care:
- Real-Time Data Capture & Synchronization: Patient vitals from connected devices are automatically transmitted and recorded within the EHR, ensuring up-to-date clinical visibility.
- Remote Patient Monitoring (RPM) Enablement: Providers can track patient health trends between visits, enabling early intervention and reducing hospital readmissions.
- Intelligent Data Filtering: Instead of flooding clinicians with raw data, systems prioritize clinically relevant insights, flagging anomalies or threshold breaches.
- Automated Alerts & Care Triggers: Abnormal readings can initiate alerts, follow-up tasks, or even escalation workflows—without manual review.
- Integration with Care Plans: Device data feeds directly into treatment plans, helping providers adjust medications, recommend interventions, or schedule follow-ups.
The biggest challenge here isn’t connectivity—it’s signal vs. noise. Without proper filtering and workflow logic, continuous data can quickly lead to alert fatigue and clinician overload.
That’s why modern integration strategies focus on contextualizing device data, ensuring that only meaningful insights drive action.
Implementation Roadmap: How to Integrate Telehealth, Labs, & Billing with EHR
Designing a workflow-first architecture is one thing—executing it is where most organizations struggle. The biggest mistake? Trying to integrate everything at once. That approach usually leads to complexity, delays, and half-functional workflows.
A smarter path is to prioritize integrations based on operational impact and ROI, while building toward a unified ecosystem over time.
Step 1: Start with High-Impact Workflows
Not all integrations deliver equal value. The goal is to begin where fragmentation hurts the most:
- Telehealth EHR integration → Fixes access and documentation gaps
- Lab EHR integration → Accelerates clinical decision-making
- Revenue cycle EHR integration → Improves financial performance
Recommended sequence: Telehealth → Labs → Billing → Patient Portal → Devices
This order ensures you first stabilize care delivery workflows, then extend into engagement and continuous monitoring.
Step 2: Move from Point Integrations to a Unified Ecosystem
Early-stage integrations often connect systems directly (point-to-point). While quick to implement, they don’t scale.
A better approach:
- Use an API-first architecture (FHIR-based)
- Introduce middleware/integration engines for orchestration
- Standardize data formats across systems
This allows you to transition from isolated integrations to a connected healthcare platform where workflows move seamlessly across modules.
Step 3: Focus on Workflow Continuity (Not Just Data Exchange)
At every stage, validate:
- Does this integration trigger the next step automatically?
- Are clinical, operational, and financial workflows connected?
For example:
- Telehealth visit → auto documentation → lab order → billing trigger
- Lab result → alert → follow-up → patient notification
If workflows stop at data exchange, the integration is incomplete.
Step 4: Connect EHR to Third-Party Healthcare Applications
Modern ecosystems require flexibility. You’ll likely integrate:
- Telehealth platforms
- Lab information systems (LIS)
- Billing/RCM tools
- RPM and wearable platforms
Ensure:
- Secure API access (OAuth2, SMART on FHIR)
- Role-based permissions
- Vendor-neutral architecture to avoid lock-in
Step 5: Ensure Compliance, Security, and Performance
Integration expands your attack surface and compliance scope. You must build with:
- HIPAA compliance (data privacy and security)
- Audit logs for every transaction
- End-to-end encryption
- Access control and identity management
Also consider:
- System latency (real-time workflows depend on speed)
- Data integrity across systems
- Failover and error handling mechanisms
Step 6: Scale Toward Intelligent Automation
Once foundational integrations are stable, the next step is optimization:
- Introduce AI-driven documentation and coding
- Use predictive analytics for proactive care
- Automate decision support and alerts
This is where integration evolves into true healthcare workflow automation.
Conclusion: Future-Proofing with an EHR Workflow Integration Guide
Healthcare organizations don’t need more systems—they need systems that work together seamlessly. As we’ve seen, the real challenge isn’t connectivity alone, but the lack of coordinated workflows across the care continuum. Disconnected tools create friction, delays, and inefficiencies that impact both patient outcomes and financial performance.
A workflow-first EHR integration strategy addresses this at its core. By positioning the EHR as the central orchestration layer and connecting key modules—telehealth, labs, revenue cycle, patient portals, and devices—you create a unified ecosystem where workflows move without interruption.
More importantly, it sets the foundation for scalable healthcare workflow automation, where systems don’t just exchange data—they trigger actions, guide decisions, and support continuous care.
As healthcare continues to evolve toward value-based and digitally driven models, this kind of integration is no longer optional. A well-designed EHR workflow integration guide becomes the blueprint for building resilient, future-ready healthcare systems.
Ready to build your own centralized network for improving patient experience and reducing workload? See how A&I Solutionscan help you achieve this.
Frequently Asked Questions
An EHR workflow integration guide outlines how to connect clinical, operational, and financial systems into unified workflows. It shifts focus from data exchange to care coordination, reducing fragmentation, improving efficiency, and ensuring seamless patient journeys. This is critical for healthcare systems aiming to enhance outcomes, reduce burnout, and support scalable, value-based care delivery.
Integrating telehealth, labs, and billing requires a workflow-first approach using FHIR APIs, HL7 messaging, and middleware orchestration. Telehealth visits trigger documentation, lab orders (ORM), results (ORU), and billing workflows automatically. This creates a continuous flow where clinical events initiate financial and follow-up actions without manual intervention.
A workflow-first EHR integration strategy focuses on designing end-to-end care processes before connecting systems. Unlike traditional integration, which prioritizes data exchange, this approach ensures that clinical events trigger actions across systems. It transforms EHRs into orchestration engines, enabling seamless transitions between care stages and improving both efficiency and outcomes.
Healthcare workflow automation eliminates manual handoffs by triggering actions based on real-time events. It reduces documentation burden, accelerates decision-making, minimizes errors, and ensures timely billing. By connecting clinical and operational processes, automation improves care coordination, reduces delays, and allows providers to focus more on patient care instead of administrative tasks.
Key components include scheduling synchronization, real-time documentation, automated workflow triggers, billing integration, and patient data access. Telehealth EHR integration ensures that virtual visits are embedded into clinical workflows, enabling seamless transitions from consultation to follow-ups, prescriptions, and claims processing while improving both provider efficiency and patient experience.
Lab EHR integration uses HL7 ORM messages to send test orders from the EHR to lab systems and ORU messages to return results. This creates a closed-loop workflow where orders, processing, and results are automated. It reduces manual entry, ensures accurate data capture, and enables faster clinical decision-making through real-time result availability.
Revenue cycle EHR integration connects clinical documentation directly to billing workflows. It enables automated charge capture, real-time eligibility checks, and accurate coding. By reducing manual intervention and errors, it minimizes claim denials, accelerates reimbursements, and ensures that healthcare providers are properly compensated for services delivered.
Patient portal FHIR integration enables real-time access to health records, appointments, and billing information through standardized APIs. It supports secure communication, self-service tools, and personalized engagement. This improves transparency, reduces administrative workload, and empowers patients to actively participate in their care journey.
Medical device EHR integration connects wearables and monitoring devices to capture real-time patient data. It enables remote patient monitoring, flags abnormal readings, and triggers clinical actions. By transforming continuous data into actionable insights, it supports early intervention, reduces hospitalizations, and enables proactive, preventive care.
Best practices include using FHIR-based APIs, OAuth2/SMART on FHIR authentication, role-based access control, encryption, and audit logging. Organizations should adopt vendor-neutral architectures, ensure compliance with HIPAA, and implement secure data exchange protocols to protect patient data while enabling scalable, flexible integrations.
Common challenges include data silos, inconsistent standards, integration complexity, workflow misalignment, and alert fatigue. Legacy systems and lack of interoperability further complicate automation. Without proper workflow design, automation can increase noise instead of efficiency, making it critical to align technology with real clinical and operational processes.
Automation improves EHR workflow integration by triggering actions such as documentation, coding, alerts, and billing based on real-time events. It eliminates duplicate data entry, reduces human errors, and ensures continuity across workflows. This allows healthcare teams to operate more efficiently while focusing on patient care instead of administrative tasks.
The recommended roadmap starts with high-impact integrations like telehealth, labs, and billing, followed by patient portals and devices. Organizations should adopt API-first architecture, ensure compliance, and scale gradually from point integrations to a unified ecosystem. Continuous optimization with automation and analytics helps achieve long-term efficiency and scalability.
- On May 11, 2026
- 0 Comment