Multi-EHR Integration Architecture: Connecting Epic, Cerner, & Allscripts in One Network
One of our clients was using three EHRs: Epic, Cerner, and Allscripts to manage different tasks. Epic was used for managing patient records and exchanging data, Cerner for billing, and Allscripts for specialty practices.
While the intent was to utilize the best in all systems to make work efficient, all this only led to fragmented workflows and siloed data. Many organizations today use multiple EHR systems and often face similar issues.
The reason is that, in the modern healthcare landscape, it is not possible to work on a single EHR system. However, just connecting multiple EHRs is not the right approach. It needs a structured approach that streamlines workflows rather than complicating the integration.
At first, the traditional point-to-point integration and HL7 interfaces may work, but they become expensive and difficult to manage as healthcare organizations scale. That’s why, while scaling, the need to shift towards a multi-EHR integration architecture increases to support interoperability without any operational bottlenecks.
However, it is important to understand how to build a multi-EHR integration architecture. Rather than connecting systems, the goal is to create a unified data layer that keeps data from Epic, Cerner, and Allscripts consistent, normalized, and immediately usable across systems.
That’s why, in this blog, we will break down how to design an Epic Cerner Allscripts integration strategy to build a scalable architecture that supports workflow automation, interoperability, and AI-powered capabilities.
Core Design Patterns: Choosing Your EHR Integration Architecture Design
One of the biggest decisions while designing a multi-EHR integration is to decide which design patterns to follow. Because the pattern you choose defines the scalability, performance, and long-term maintainability of the integration.
| Pattern | Description | Best Use Case |
| Hub-and-Spoke | The central integration hub manages all data flows between systems | Large enterprise health systems |
| FHIR Facade | Unified API layer abstracts vendor-specific differences | Multi-vendor interoperability |
| Hybrid | Combines centralized and distributed models | Complex healthcare ecosystems |
More importantly, there is no one-size-fits-all design, and the choices vary as per the size of practice, number of systems, how data flows, and how scalable the solution must be. With this in mind, there are three main architectural designs that are followed by many healthcare organizations:
- Hub-and-Spoke Model: This model centralizes all the integrations and connects the EHRs to one integration engine. Moreover, the data flows through a controlled central layer, reducing the number of direct system-to-system integration points. If you are a healthcare organization that needs visibility and complete control, then this model works best. However, it can be difficult to upgrade and scale if not designed to scale.
- FHIR Facade Pattern: If you choose this model, it adds an additional layer of unified API to reduce the complexity of multi-EHR integration. Rather than building a different logic for Epic, Cerner, and Allscripts, it creates a single standardized API for applications to interact with. This layer translates requests for vendor-specific APIs, normalizes data structures, and responses so they look the same across systems. Although this does not reduce complexity, it makes scaling easier and brings multi-EHR interoperability.
- Hybrid Architecture: This design is used the most as it combines the best of both models. It brings centralization of hub-and-spoke with API-based access, supporting both modern FHIR-based and legacy systems powered by HL7 interfaces. This approach balances flexibility and control, making it suitable for complex, multi-EHR environments and integrations.
Connection Strategies for Epic, Cerner, & Allscripts
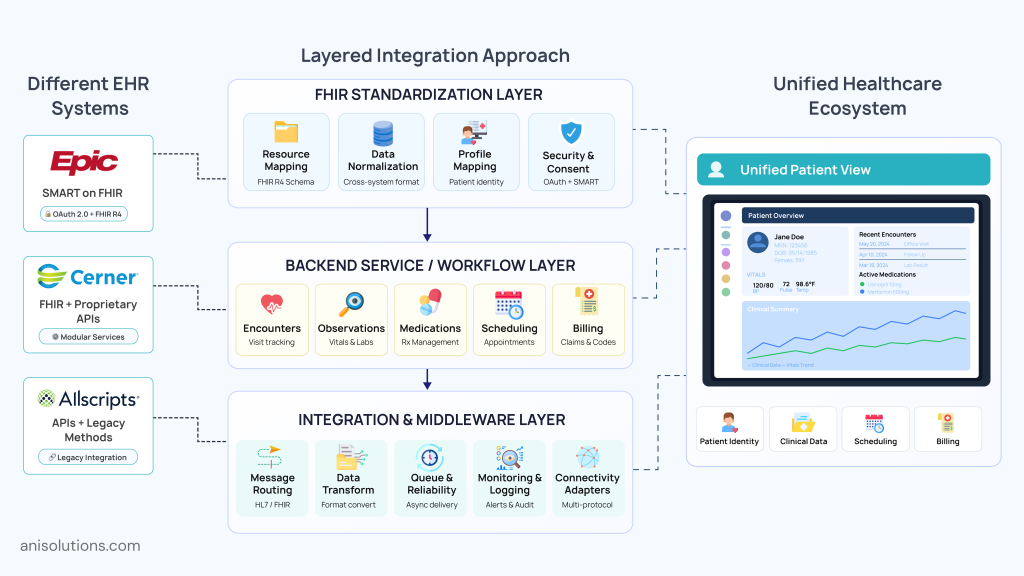
After choosing the architecture design pattern, building an Epic Cerner Allscripts integration is necessary. As each platform has its own architecture, access model, and level of standardization, just connecting APIs is not enough; you need vendor-aware and architecture-driven strategies.
Additionally, while all the EHRs support SMART on FHIR and FHIR APIs, they are implemented differently across multiple platforms.
- Epic systems usually use SMART on FHIR with controlled access through its ecosystem.
- Oracle Health (Cerner) supports a mix of FHIR, proprietary APIs, and modular services.
- Allscripts often combines APIs with legacy integration methods.
Because of these differences, a one-size-fits-all approach does not work effectively.
For connecting Epic Cerner and Allscripts via FHIR, a layered approach is the best choice. In this approach, FHIR APIs standardize the data, backend service integrations handle system-level workflows, and middleware is used for managing communication across systems.
However, maintaining consistency across systems is the biggest challenge in achieving multi-EHR interoperability. Key areas that need synchronization include:
- Patient data and identity management.
- Clinical workflows such as encounters, observations, and medications.
- Operational systems such as scheduling and billing.
With each system may represent data differently, synchronization requires:
- Data normalization.
- Mapping across FHIR profiles.
- Consistent update logic across systems.
That’s why you need to consider all these things to design a well-planned strategy that creates a unified ecosystem rather than fragmented systems.
Architecture Design: Building a Unified Multi-EHR Layer
For any multi-EHR integration architecture, it is important to have a unified data layer and not just connectivity. Without the unified data layer, even well-connected systems remain fragmented, with inconsistent data and disconnected workflows.
However, traditional integrations only focus on moving data between systems, whereas healthcare data integration architecture needs:
- Centralizing data into a consistent format.
- Eliminating duplication across systems.
- Enabling a single source of truth for downstream applications.
Additionally, a centralized architecture for multi-EHR systems is the backbone for all data exchange. It typically includes:
- Data Ingestion Layer: Collects data from multiple EHRs via APIs, FHIR, and legacy interfaces.
- Normalization & Transformation Layer: Standardizes data structures across vendors.
- Unified Data Repository: Stores normalized data for consistent access.
- Access Layer (APIs/Services): Provides clean, standardized data to applications and analytics systems.
And the data is not standardized, even with the FHIR. For example, allergy data in Epic may differ from Cerner or encounter structures may vary across systems. To handle this, organizations must:
- Define internal standard data models.
- Map vendor-specific FHIR profiles to those models.
- Maintain consistency across all integrations.
Finally, when the data is unified, it enables real-time analytics, workflow automation across systems, and AI-driven insights. Because, without a unified layer, these capabilities remain limited or fragmented.
So, a successful multi-EHR integration architecture is not based on how many systems it connects, but on how well it unifies them.
Implementation & Rollout Strategy
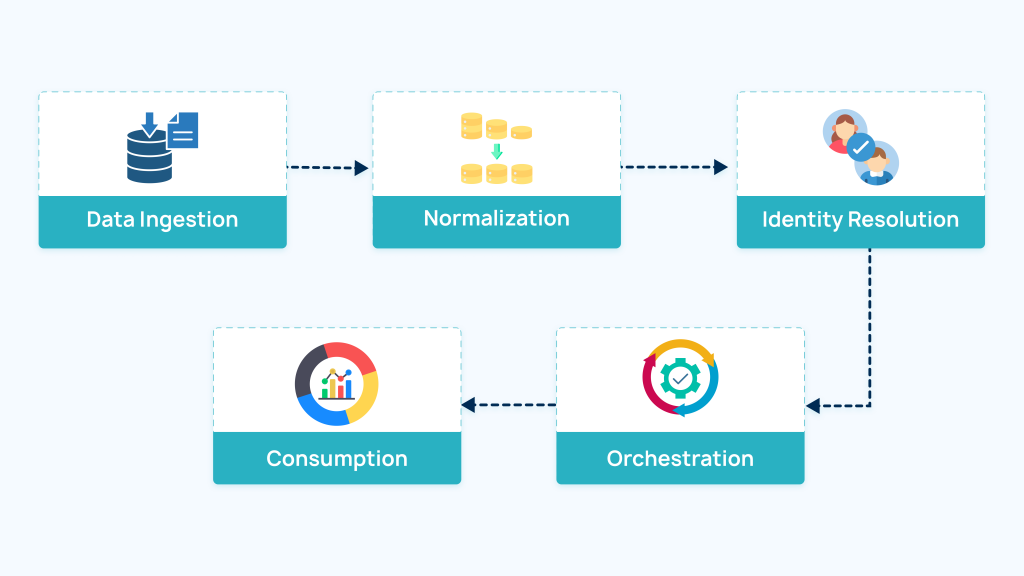
Designing the multi-EHR integration architecture is only the first step, as successful implementation and rollout across systems such as Epic Systems, Cerner, and Allscripts. For it to work, you need to follow a structured pipeline:
Data Ingestion→Normalization→Identity Resolution→Orchestration→Consumption
Where,
- Data ingestion pulls data from multiple EHRs using APIs, FHIR, and legacy interfaces.
- Normalization standardizes formats across systems.
- Identity resolution (MPI) links patient records across platforms.
- Orchestration manages data flow between systems and applications.
- Consumption enables use in analytics, workflows, and downstream systems.
In the implementation, one of the critical components is setting up the Master Patient Index (MPI). This is important because in multi-EHR environments, the same patient may exist in multiple systems with different identifiers, and records must be matched accurately to avoid duplication or clinical risk.
By using MPI solves these issues by deterministic matching and probabilistic matching with rule-based or AI-driven matching. Without MPI, true multi-EHR interoperability is not possible.
Additionally, there are also risks if you implement an entire multi-EHR integration at once, so phased implementation works best. You can start with one system or facility, validate workflows and data accuracy, and expand to additional systems such as hospitals, clinics, and specialties. This reduces disruption and ensures stability during scale.
Technical Challenges in Multi-EHR Systems
In a multi-EHR integration architecture, data consistency is one of the biggest challenges.
Patient identity is often fragmented across systems like Epic Systems, Oracle Health (Cerner), and Allscripts. The same patient may exist under different identifiers, requiring a robust Master Patient Index (MPI) with probabilistic matching to accurately link records.
Additionally, each system follows different data models and terminologies. This creates the need for advanced normalization and mapping strategies to ensure data remains consistent and usable across platforms.
Performance becomes a critical concern as data flows across multiple systems.
- API rate limits vary across vendors
- Response times are inconsistent
- Real-time workflows may experience latency
In high-volume environments, such as large health systems, managing data exchange across facilities requires scalable infrastructure and optimized orchestration to prevent delays and system bottlenecks.
Security in multi-EHR environments is significantly more complex due to multiple systems and access models.
- Each EHR may use different authentication mechanisms
- Centralized OAuth 2.0 token orchestration is required
- Secure data exchange and audit logging must be maintained across all systems
Ensuring compliance while managing distributed access increases architectural complexity and requires careful planning.
Conclusion: Future-Proofing with a Unified Network
In modern healthcare, using a single EHR to do everything is nearly impossible. However, if you are just connecting the systems without a structured architecture, then it becomes fragmented, leading to a disconnect between the EHR systems you are using.
To solve this problem, leveraging a multi-EHR integration architecture can be the best choice. This architecture connects multiple workflows to a centralized point that streamlines operations rather than hindering them.
But for this to work successfully, it is important to choose the correct design pattern to ensure interoperability without compromising scalability. This is where an experienced integration partner becomes essential, and A&I Solutions can help you in designing a multi-EHR integration approach that is reliable, scalable, and interoperable.
To get more information, talk to our integration experts, and let’s get started with your centralized architecture for multi-EHR systems.
Frequently Asked Questions
A multi-EHR integration architecture connects systems like Epic Systems, Oracle Health, and Allscripts into a unified ecosystem. It works by ingesting, normalizing, and orchestrating data across platforms, enabling consistent workflows, interoperability, and a single source of truth for healthcare operations.
Building this architecture involves data ingestion from multiple EHR systems, normalization into a common format, identity resolution using MPI, workflow orchestration, and the exposure of unified data through APIs. The focus is on creating a centralized or hybrid model that supports scalability, interoperability, and consistent data exchange.
Key challenges include patient identity mismatches, inconsistent data formats, partial FHIR implementation, API variability, and legacy system dependencies. These issues make it difficult to maintain accurate data exchange and require robust normalization, mapping, and orchestration to ensure reliable interoperability across systems.
Connecting Epic Systems, Oracle Health, and Allscripts via FHIR involves using FHIR APIs for standardized data exchange. A facade or middleware layer maps vendor-specific data into a consistent format, enabling unified access and cross-system interoperability.
A centralized architecture uses a single hub to manage all data flows, offering control and simplicity. A distributed architecture allows systems to communicate directly, improving flexibility but increasing complexity. Hybrid models combine both approaches, balancing scalability, performance, and adaptability in multi-EHR environments.
Scalability is achieved by using modular architecture, API-driven integration, and event-based data flows. A unified data layer, efficient orchestration, and support for both real-time and batch processing ensure the system can handle increasing data volumes while maintaining performance and reliability.
AI enhances multi-EHR integration by improving data normalization, automating cross-system mapping, and enabling intelligent patient matching. It also supports predictive analytics, workflow automation, and anomaly detection, helping organizations extract more value from integrated healthcare data.
Multi-EHR systems must comply with HIPAA regulations, use OAuth 2.0 for secure API access, and implement role-based permissions. Encryption, audit logging, and secure data exchange are essential to protect patient information and maintain compliance across multiple systems and environments.
- On May 7, 2026
- 0 Comment