
Information Blocking Healthcare Rules: What Your Healthcare IT Team Needs to Implement
Healthcare data shifted from being allowed to share to being expected to share. This change is driven by the full enforcement of information blocking healthcare rules under the 21st Century Cures Act.
This also shifted the role of health IT teams from support to legally accountable compliance entities.
Before, the role of health IT teams was to build and maintain EHR systems and integrations. While doing this, they could limit APIs to improve performance, and providers could control how and when to move data.
But now, regulations defined by the Office of the National Coordinator for Health Information Technology (ONC) prohibit any unreasonable interference with access, exchange, and use of Electronic Health Information (EHI), while enforcement by the Office of Inspector General (OIG) has made non-compliance a measurable risk. The most important part of all this is that now impact is greater than intent. That’s why each architectural decision, even unintentional, such as a delayed API or UI change by health IT teams, can be a compliance exposure and not just an engineering decision. If you are a healthcare CTO or EHR developer, this changes everything. Now, real-time data availability, API-first architecture, and seamless third-party integrations are non-negotiable design factors. However, if you don’t address these considerations early, then organizations can face legal actions for compliance exposure and OIG information blocking penalties. In this blog, we will explain their impact on Electronic Health Information (EHI), information blocking rules for healthcare IT teams, what counts as a violation, and how to build a compliance-ready IT strategy. Because health IT teams are not just supporting a team, but also compliance stakeholders in EHR interoperability.
What Are Information Blocking Rules in Healthcare?
First things first, information blocking rules are primarily designed to keep patient data easily accessible, exchangeable, and immediately usable without any unnecessary restrictions.
Currently, under the ONC’s regulations, any practice that interferes with the access, exchange, or use of Electronic Health Information (EHI), without a valid exception, is considered information blocking.
For healthcare IT teams, this means delayed API response, restricted data access, or incomplete workflows that make integrating with third-party applications difficult. So, keep in mind that having real-time access and API-first design is essential for EHR systems.
Moreover, the scope of EHI has also increased under the 21st Century Cures Act. Now, providers must share clinical records, including lab reports, medications, problem lists, and visit notes, without hiding anything.
This means developers need to ensure that data is well-structured, accessible, and available through standardized formats and mechanisms such as LOINC and APIs. Any limitations set on this information can lead to compliance exposure and penalties.
All these information blocking healthcare rules mainly apply to three groups:
- Healthcare Providers
- Healthcare IT Developers
- Health Information Networks (HIN)
For EHR developers and healthcare CTOs, these changes are major because they have become a liable entity for managing system compliance. Their single engineering decisions, such as API configurations, can directly impact compliance.
However, all these changes do not mean giving unrestricted access to patient information; it just means removing any unnecessary barriers that slow down data exchange. That’s why all healthcare organizations are now expected to have real-time data availability, standardized APIs, and seamless third-party integrations.
Information Blocking Compliance Checklist for Health IT Teams
DownloadWhat Qualifies as Information Blocking?
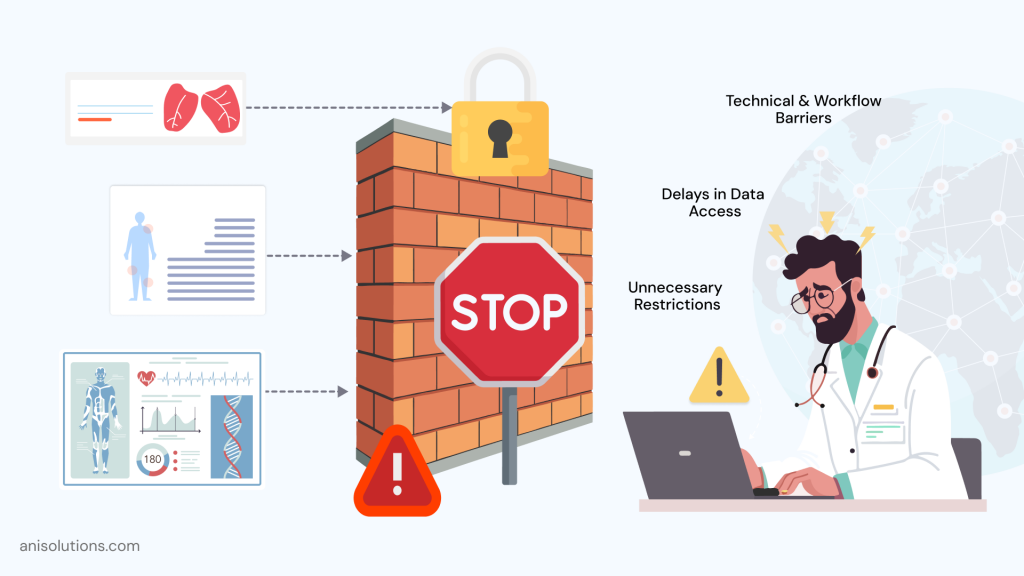
One thing that is important to highlight in information blocking rules is that only the denial of access is not considered information blocking. In practice, anything that restricts data accessibility, including unnecessary delays or barriers, is qualified as information blocking.
Let’s understand what is considered information blocking under the current rulebooks of the ONC:
- Delays in Data Access: The first that qualifies as information blocking is a delay in data availability, even if the data is shared with the app or the patients. That’s why having real-time data availability is one of the core requirements for the systems now. One example of this is API throttling that slows down response times.
- Unnecessary Restrictions on Data Sharing. If the providers or healthcare information networks impose unnecessary restrictions on data exchange outside the exceptions, then it can lead to compliance issues. For example, blocking or delaying third-party application integrations.
- Technical & Workflow Barriers: Some of the crucial but most overlooked information blocking types happen at the design and workflow level. For instance, Complex authentication or authorization processes, or the use of non-standard or incompatible data formats.
To make this healthcare data sharing compliance easier to understand from an EHR developer’s perspective, let’s look at some real-world scenarios. For example, you limit the API to manage the system load and improve performance, and if it delays the data access, then it becomes a compliance violation.
In short, for healthcare IT developers, information blocking is not just a regulatory concept but a design and operational risk. Most importantly, it fundamentally changes how developers build the systems for making data accessible, exchangeable, and usable without adding unnecessary restrictions.
Operationalizing the Eight Exceptions
While it’s true that information blocking rules need open access to patient data, there are some exceptions defined by the ONC where providers can limit data access. If you are a healthcare IT developer, then understanding these information blocking exceptions is essential as they need to implement them on system-level logic, workflows, and governance.
Here is a table that explains how these exceptions apply in particular situations and how an EHR developer should implement solutions for them:
| Exception | When It Applies | IT Implementation Example |
| Preventing Harm | When sharing data could harm a patient or another person | Temporarily restrict sensitive mental health or safety-related data |
| Privacy | When access violates patient consent or privacy laws | Block access if authorization or consent is not properly captured |
| Security | When there is a risk to the system or data security | Enforce authentication, encryption, or block suspicious access attempts |
| Infeasibility | When fulfilling the request is technically not possible | The legacy system cannot support the required data format or API |
| Health IT Performance | When sharing data impacts system stability or maintenance | Temporary downtime during upgrades or performance tuning |
| Content & Manner | When data can be shared in an alternative, reasonable way | Provide data via a standardized API instead of a custom format |
| Fees | When charging is reasonable and cost-based | Apply transparent API usage or data access fees |
| Licensing | When protecting intellectual property is necessary | Restrict access to proprietary algorithms or system logic |
However, one thing that you must understand is that these information blocking exceptions are not loopholes. They are structured safeguards for protecting PHI. That’s why, for healthcare IT teams, the goal is not just to enable data access, but also to ensure there are justifiable restrictions when the mentioned situation arises.
Information Blocking Exceptions Playbook (With Real IT Scenarios)
Get NowIT Implementation: How to Prevent Information Blocking in EHR Systems
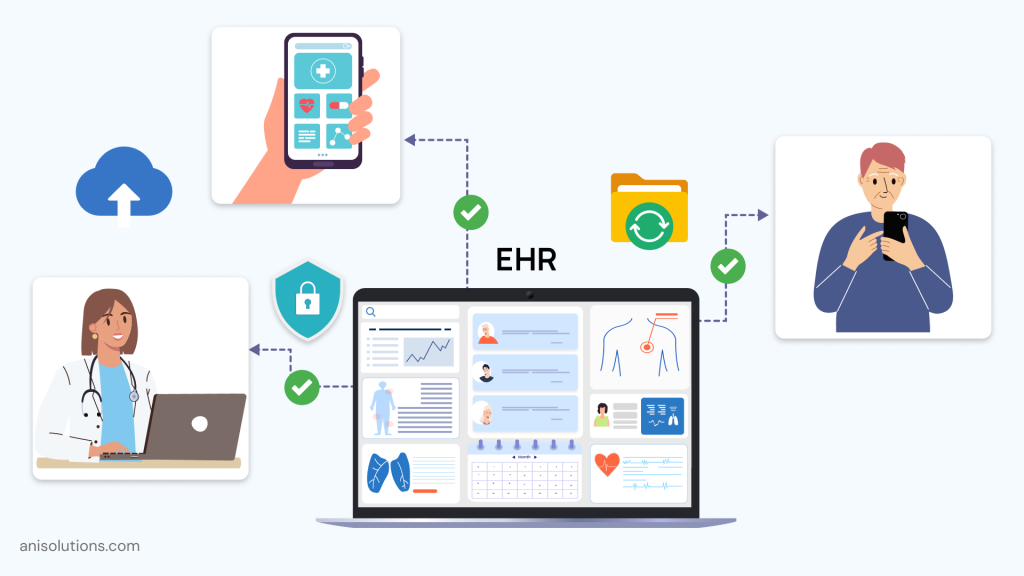
Although information blocking is a critical compliance issue, it can be solved efficiently by building EHR systems that support real-time data availability and standardized access to Electronic Health Information (EHI).
From the healthcare IT team’s perspective, compliance must be built into the architecture, workflow, and integrations. And for this to happen, one of the core requirements is accountability with audit logs to track and justify how data is accessed, shared, and restricted.
Another requirement is to ensure an API-first architecture that can seamlessly integrate with third-party applications of the patient’s choice. More importantly, the ONC is making it compulsory to use FHIR APIs to ensure interoperability and prevent any delays in health information exchange.
The next development consideration is automation of workflows and approval processes to eliminate any unnecessary restrictions due to manual processes. Also, you should regularly test patient portals and all third-party integrations, because the responsibility of patient data privacy and security still lies with healthcare providers.
Finally, it is important to align the system design and architecture with the information blocking exceptions. This creates a balance between data accessibility and regulatory safeguards, reducing risks of compliance violations.
In short, preventing information blocking is not just reacting to regulations; healthcare IT developers need to build systems that are transparent, interoperable, and audit-ready while maintaining their peak performance.
Risk Management: OIG Enforcement & Penalties
While understanding how information blocking healthcare rules work is important, it’s also important to understand how they are enforced and penalized. Most importantly, the ONC only defines the rules; it’s the Office of Inspector General (OIG) that investigates a violation and imposes penalties.
The process is complaint-based, meaning when a patient, provider, or third-party developers report issues, the OIC investigates the violation. In the case of information blocking, all the mentioned entities can file complaints about delayed or restricted access.
This investigation primarily involves reviewing audit logs, system behaviour, and access patterns. By analysing all these factors, the OIC determines whether there has been interference with the access, exchange, or use of Electronic Health Information (EHI).
If found, the OIC information blocking penalties can go up to $1 Million per violation category. Additionally, providers may face disincentives from programs aligned with the Centers of Medicare & Medicaid Services (CMS), affecting reimbursement and value-based care models.
However, most of the violations are unintentional, happening through system design choices. For instance, slow APIs, incomplete data access, or poorly implemented workflows. That’s why healthcare providers and healthcare IT teams need to monitor each choice carefully before implementing it.
OIG Compliance Risk Assessment Toolkit for EHR Systems
Click HereBuilding a Compliance-Ready IT Strategy

Only fixing EHR technically is not enough to prevent any information blocking-related issues; you need to develop an IT strategy aligned with compliance.
So, the first step to this is conducting an internal audit of the system through healthcare IT developers to identify where potential bottlenecks can happen. This includes assessing APIs, workflows, audit logs, and third-party connections to find any delays, restrictions, or inconsistencies in EHI exchange.
After this, it is essential to align all workflows with compliance requirements defined by the ONC. More importantly, the system design should reduce restrictions, whether intentional or unintentional. It is also important to ensure any restrictions are justified under information blocking expectations and documented properly.
Then comes training and governance, as healthcare IT must understand how its decisions can lead to compliance violations. By establishing a clear governance structure, you can observe system performance and minimize the unintentional violations through identifying issues or slow APIs and proactively fixing any issues, reducing compliance risks.
Finally, organizations must move towards building a sustainable compliance framework. This includes continuous monitoring of system performance, regular compliance reviews, and proactive updates to align with evolving regulations and interoperability standards.
Conclusion: From Gatekeeper to Enabler
In a nutshell, the patient data should be available in real time without any delays or unnecessary restrictions. This shift fundamentally changes how EHR systems and integrations were developed and, as a result, changes the roles of healthcare IT developers.
Because now they need to develop API-first and systems that support real-time healthcare data exchange. This makes them the enabler of seamless integration, data access, and exchange. More importantly, even a single architecture choice can impact how data is accessed, exchanged, and used, making them liable for compliance violations.
So, developers now must carefully consider every engineering choice before implementing it to prevent any information blockage penalties.
Are you interested in developing systems that are compliant and allow seamless data accessibility, exchangeability, and usability? Then connect with our EHR integration experts to start your system assessment.
Frequently Asked Questions
Information blocking rules, defined under the 21st Century Cures Act and enforced by the Office of the National Coordinator for Health Information Technology, prohibit practices that interfere with the access, exchange, or use of electronic health data, unless a valid exception applies.
In EHR systems, information blocking includes delays in API responses, restricted data access, incomplete EHI sharing, or complex workflows that hinder usability. Even unintentional system design decisions that create unnecessary friction in accessing or exchanging data can be considered information blocking under ONC guidelines.
Responsibility for compliance is shared among providers, health IT developers, and health information networks. For IT teams, this means system design, API performance, and integration decisions directly impact compliance, making them legally accountable “actors” under ONC information blocking regulations.
Healthcare IT teams should document exceptions related to preventing harm, privacy and security, infeasibility, health IT performance, content and manner, fees, and licensing. Each exception must meet strict criteria and be supported by audit logs, justification, and standardized workflows to ensure compliance during audits or investigations.
Electronic Health Information (EHI) defines the scope of data that must be accessible under information blocking rules. IT systems must ensure EHI is available, complete, and shareable via standardized methods. Any limitation in access, format, or timeliness of EHI can result in compliance violations.
Organizations can prevent information blocking by implementing real-time API access, maintaining audit logs, minimizing manual workflows, and ensuring seamless third-party integrations. Continuous monitoring, performance optimization, and aligning system behavior with ONC-defined exceptions help reduce compliance risks and support interoperable data exchange.
The Office of Inspector General can impose civil monetary penalties of up to $1 million per violation category for health IT developers. Providers may face disincentives through Centers for Medicare & Medicaid Services programs, affecting reimbursements and participation in value-based care initiatives.
Under the infeasibility exception, organizations must demonstrate that fulfilling a data request is technically or operationally impossible. IT teams should document limitations, provide clear justification, and, where possible, offer alternative access methods to remain compliant with ONC requirements while avoiding information blocking violations.
- On April 3, 2026
- 0 Comment


