Reducing Double Data Entry in EHR with Integration
Have you ever had to enter the same data in multiple systems after completing a visit?
Well, if your answer is yes, then you are not alone, as most of our clients have similar issues. Even with the EHR connecting their labs, pharmacies, billing, and other external systems, they have to manually enter data into each system every time.
This is exactly why reducing double data entry in EHR integration has become a top priority in modern healthcare systems.
Duplicate data entry doesn’t just waste time—it increases clinician workload, introduces inconsistencies, and directly impacts patient safety. When the same data exists in multiple versions, even small discrepancies can lead to incorrect diagnoses or billing errors.
To eliminate duplicate entry in EHR systems, organizations must move beyond basic integrations and focus on real-time data synchronization, workflow automation, and standardized data exchange.
A strong focus on integration efficiency in EHR ensures that data is captured once and seamlessly reused across systems—without manual intervention.
In this guide, we’ll break down how to reduce double data entry through smarter EHR integration, automation, and interoperability.
Check Your Systems Integration Readiness with Our EHR Integration Readiness Checklist
Check NowWhy Double Data Entry Still Exists in EHR Integration?
For many clinics, entering data by hand has become normal, despite having an EHR that connects labs, pharmacies, and billing systems. Although the EHR connects systems, the data doesn’t seamlessly flow across systems, remaining fragmented. This is why clinicians have to bridge this gap by manually updating the patient records.
Moreover, if the system relies on batch-based data exchange instead of automated data uploads, the problem becomes even more complex. Because in today’s fast-paced healthcare environments, waiting for systems to sync at fixed intervals can slow down care delivery. To avoid this, the staff duplicates entries, and this increases workload and chances for errors.
Additionally, a lack of real-time EHR data synchronization means systems operate in different timelines. The data created in one system is not instantly synchronized in another, leading to different versions of the same patient records.
With all these issues, patient records become inaccurate, and rather than supporting care, they hinder smooth care delivery. That’s why reducing double data entry in EHR systems is challenging, and to solve it, proper integration and EHR workflow automation are necessary.
The Enter Once, Use Everywhere Integration Model
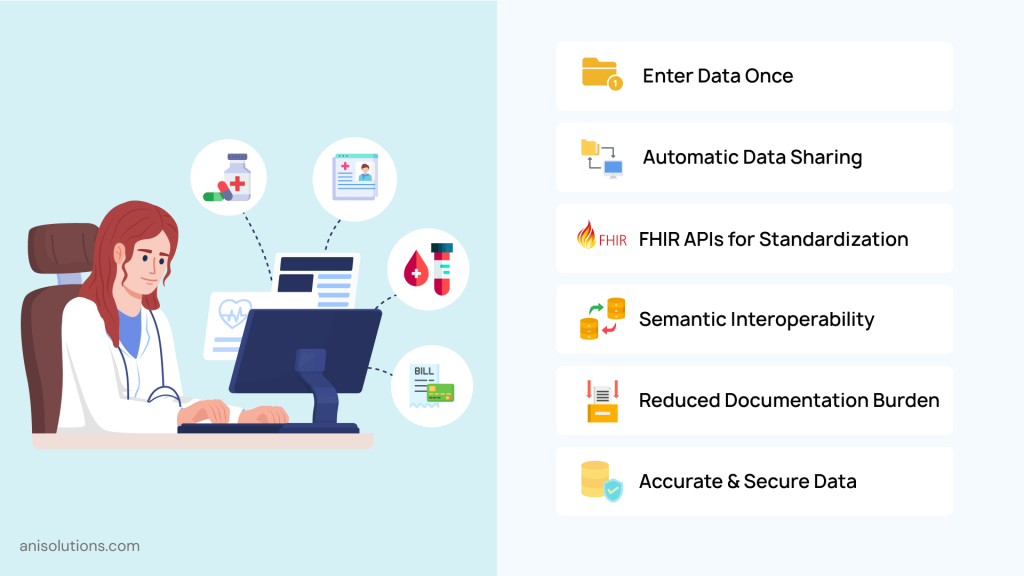
In modern healthcare, repetitive data entries are not practical, but when the systems lack effective EHR integration, things shift to manual. However, the “enter once, use everywhere” model changes this as it updates data automatically in all connected systems, reducing clinician burnout through EHR automation. Here is how the model helps clinicians get out of repetitive data entries:
- Capturing Data a Single Time & Reusing It Across Systems: This keeps the records consistent and unified across the systems by creating a single source of information and creating data at the point of care. When patient data, such as demographics, vitals, and diagnoses, is captured during a visit, it is automatically available across the system without any manual intervention. This keeps data consistent and accurate without any duplication.
- Role of FHIR APIs for Data Entry Reduction: The FHIR API plays a crucial role in double data entry reduction by enabling standardization across the system. Rather than relying on custom integration for each system, FHIR APIs standardize the healthcare data for each connected system. With this, the data is updated in all the systems, regardless of the data format they use, significantly reducing the need to manually enter data for different formats and saving time for clinicians.
- Importance of Semantic Interoperability in EHR Systems to Prevent Re-Coding: These are the standards that help clinics in keeping data meaningful across systems. Without semantic interoperability, the context of data can change in different systems as the data formats are different in each system. By using semantic interoperability, terminologies are aligned across systems, ensuring lab results, diagnosis reports, and clinical observations are understood consistently without requiring manual correction.
In short, the biggest advantage of this model is that it reduces documentation burden without changing the workflows. It automates data reuse by integrating systems and implementing workflow automation. This way, organizations can eliminate repetitive documentation, improve data reliability, and reduce clinician burnout without compromising productivity and security.
For a detailed breakdown of how seamless integration helps in improving productivity and reducing clinician burnout, read our blog, Building EHR Systems with Seamless Integrations.
How EHR Integration Improves Billing Efficiency and Reduces Rework?
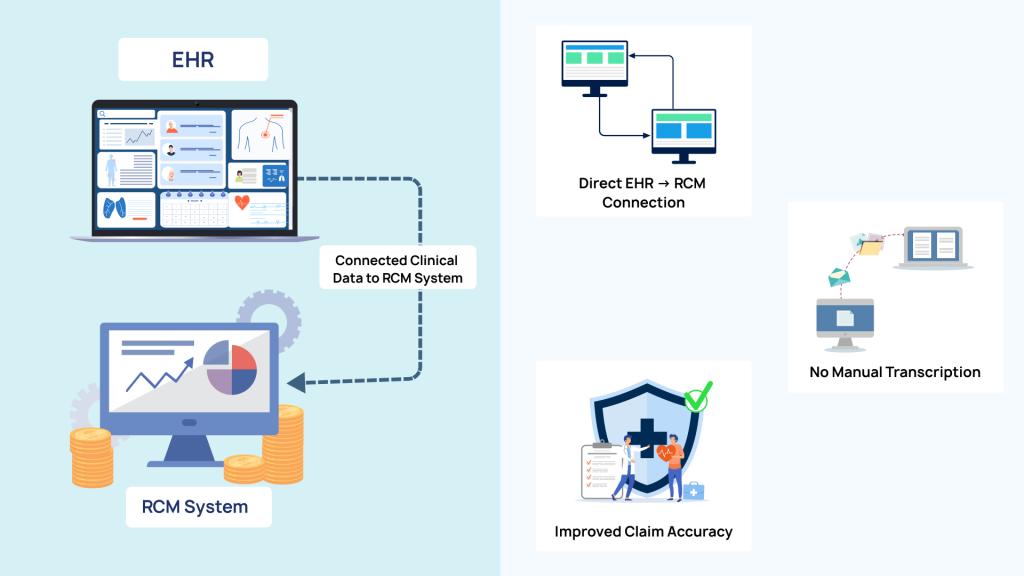
One of the services impacted visibly by disconnected EHR systems is billing. When clinical data does not automatically flow into the revenue cycle management software, administrators have to manually enter the data. This slows down the billing process, along with creating inaccuracies and inconsistencies, which directly impact reimbursement and compliance.
- Connecting Clinical Documentation Directly to RCM Systems: Automated integration ensures that clinical documentation captured during patient encounters feeds directly into RCM systems without manual intervention. With automated medical billing integration, diagnoses, procedures, encounter details, and provider notes are made available to coding and billing teams in real-time. This direct handoff reduces delays and accelerates the billing process significantly.
- How Automated Medical Billing Integration Reduces Manual Transcription: Manual transcription is a major source of billing inefficiency and error. Automated medical billing integration removes the need for staff to copy information from clinical systems into billing platforms or spreadsheets. Instead, structured data flows automatically between systems, preserving accuracy and context. This reduces administrative burden, shortens billing cycles, and allows revenue teams to focus on validation.
- Improving Claim Accuracy by Removing Human Re-Entry Errors: When billing data is entered multiple times by hand, errors are inevitable, such as incorrect codes, missing modifiers, or mismatched patient information. Automated integration significantly reduces these risks by eliminating human re-entry altogether. Claims generated from a single, consistent data source are more accurate, easier to audit, and less likely to be denied. The result is higher first-pass claim acceptance rates and a more predictable revenue cycle.
See How Much the Manual Data Entries are Costing You
Click HereUsing AI to Reduce Double Data Entry in EHR Workflows
Even with well-integrated systems and automated workflows, manual documentation can still linger at the point of care. Clinicians are often required to type notes, review labs, and reconcile orders while navigating time pressure and cognitive overload.
This is where AI becomes the final layer, transforming documentation from a manual task into a background process that supports, rather than interrupts, clinical workflows. AI-driven documentation shifts providers away from constant typing toward ambient and assisted data capture.
Rather than manually documenting every detail during or after a visit, clinicians can rely on AI tools to listen, observe, and assist in real-time. This allows providers to focus on patient interaction while documentation is captured passively and reviewed later, reducing both time spent on notes and mental fatigue.
| Documentation Area | Traditional EHR Workflow | AI-Enabled Workflow |
| Clinical notes | Manual typing during or after visits | Ambient, assisted documentation |
| Data structuring | Copying narrative text into fields | AI-generated structured records |
| Labs and orders | Manual review and re-entry | AI summarizes and maps data automatically |
| Documentation effort | High cognitive and time burden | Minimal disruption to care delivery |
| Data reuse | Limited, inconsistent | System-wide reuse across workflows |
In short, AI lowers cognitive load and frees clinicians to spend more time on patient care. When combined with EHR workflow automation and real-time data synchronization, AI helps in reducing clinician burnout through EHR automation, without forcing providers to change how they work.
Final Take: Improving Integration Efficiency in EHR Systems
In a nutshell, reducing double data entries in the EHR is an integration issue and needs to be solved by implementing FHIR APIs and semantic interoperability. This integration-first approach eliminates redundancy by ensuring data is captured once and reused everywhere across the systems.
The result is connected systems with seamless data flow and automated workflows that update data without any manual intervention. Most importantly, this integration makes systems scalable and interoperable for data exchange.
Are you ready to stop entering data by hand? click here to connect with our team to start your free assessment.
Frequently Asked Questions
Q. How does AI-enabled ambient documentation reduce manual data entry in 2026?
AI-enabled ambient documentation captures conversations and clinical context in real time, converts them into structured notes, and auto-populates EHR fields. Clinicians review rather than type, dramatically reducing repetitive data entry and post-visit documentation time.
Q. What is the role of FHIR APIs in eliminating repetitive clinical documentation?
FHIR APIs allow structured clinical data to move seamlessly between systems as events occur. Data entered once—such as vitals or diagnoses—can be reused across modules, eliminating re-entry and ensuring consistency across connected healthcare applications.
Q. How does real-time data synchronization between EHR and billing modules prevent claim errors?
Real-time synchronization ensures billing systems receive accurate, up-to-date clinical data instantly. This removes delays, prevents mismatches in codes or missing details, and reduces claim errors caused by outdated or manually entered information.
Q. What are the security standards for automating data flow between fragmented healthcare systems?
Secure automation relies on HIPAA-compliant encryption, role-based access controls, audit logs, and secure APIs. Standards like OAuth 2.0, TLS, and data minimization ensure patient information moves safely across systems without increasing security risk.
Q. Can automated EMR workflows directly lower clinician burnout rates?
Yes, automated EMR workflows reduce documentation time, eliminate duplicate data entry, and minimize interruptions. By shifting administrative work to background systems, clinicians spend more time on patient care, directly lowering cognitive load and burnout risk.
Q. How do integrated patient portals reduce the administrative burden of initial data intake?
Integrated patient portals allow patients to enter demographics, history, and consent data before visits. This information flows directly into the EHR, reducing front-desk workload, eliminating re-keying, and speeding up check-in processes.
AI-enabled ambient documentation captures conversations and clinical context in real time, converts them into structured notes, and auto-populates EHR fields. Clinicians review rather than type, dramatically reducing repetitive data entry and post-visit documentation time.
FHIR APIs allow structured clinical data to move seamlessly between systems as events occur. Data entered once—such as vitals or diagnoses—can be reused across modules, eliminating re-entry and ensuring consistency across connected healthcare applications.
Real-time synchronization ensures billing systems receive accurate, up-to-date clinical data instantly. This removes delays, prevents mismatches in codes or missing details, and reduces claim errors caused by outdated or manually entered information.
Secure automation relies on HIPAA-compliant encryption, role-based access controls, audit logs, and secure APIs. Standards like OAuth 2.0, TLS, and data minimization ensure patient information moves safely across systems without increasing security risk.
Yes, automated EMR workflows reduce documentation time, eliminate duplicate data entry, and minimize interruptions. By shifting administrative work to background systems, clinicians spend more time on patient care, directly lowering cognitive load and burnout risk.
Integrated patient portals allow patients to enter demographics, history, and consent data before visits. This information flows directly into the EHR, reducing front-desk workload, eliminating re-keying, and speeding up check-in processes.
- On February 10, 2026
- 0 Comment