
Essential Systems Every Modern EHR Must Connect With
In modern healthcare, data is the lifeblood of everything from delivering safe care to getting reimbursed on time. When the right data is not available at the right time, it leads to delays in care, patient experience gaps, operational risks, revenue loss, and compliance issues.
That’s why it’s important to keep data moving smoothly from team to team and system to system. One thing that makes this possible is EHR integration. Through integration, you can connect labs, pharmacies, imaging systems, and billing platforms, and have all the information sync automatically without any delays.
However, if the systems are integrated poorly, rather than connected environments, you end up with siloed data, workflow gaps, and create risks for patient health and daily operations. Moreover, today, interoperability in healthcare is no longer just an economic requirement or just a technical need. It’s an essential regulation required by the Centers for Medicare and Medicaid Services (CMS) , making seamless data exchange a necessity.
This is where robust EHR integration solutions help healthcare organizations meet these requirements. Most importantly, they help them establish essential EHR system connections as they scale and add more systems and value-based care models, without compromising their performance, compliance, and patient outcomes.
However, it’s not just about integrating more systems—it’s about knowing what to integrate with EHR and how those connections support real clinical and operational workflows. Without the right connections, even a well-built EHR becomes fragmented and inefficient.
Modern systems must meet evolving EHR connectivity requirements, ensuring seamless data exchange across labs, pharmacies, imaging systems, billing platforms, and care delivery tools—while maintaining security, scalability, and compliance.
In this guide, we will break down the essential EHR integrations every modern system must have and the benefits of EHR integration in healthcare for smoother operations and better care coordination.
Assess Your EHR’s Ability to Support Seamless Integrations Without Breaking Workflows
Evaluate NowUnderstanding EHR Connectivity Requirements in Modern Systems
When it comes to understanding modern EHR integration requirements, one thing you need to remember is that they are shaped by how care is delivered today. They need to be able to connect across teams, systems, and clinical settings. As healthcare changes, interoperability in healthcare has become essential.
Now every clinician and administrator expects that EHR seamlessly moves data from labs, pharmacies, and billing platforms to EHR and vice versa. But when the EHR fails to achieve this, the data becomes fragmented and duplicated, leading to increased care burden.
From a regulatory point of view, the CMS also mandates the EHR to have interoperability for exchanging patient data and maintain continuity of care. Another EHR integration requirement for seamless data exchange is standards such as FHIR and USCDI (United States Core Data for Interoperability).
These standards are what decide how data is structured, accessed, and exchanged across systems. For example, FHIR enables API-driven EHR integration, connecting multiple systems easily and allowing smooth data exchange. Whereas, USCDI ensures the consistency of patient data across the network.
Finally, the most crucial requirement for the modern EHR integration is to move from reactive to proactive data exchange. Before, the data was exchanged only when asked or during transitioning, but today EHRs need to update data as care happens, keeping records continuous and longitudinal.
With these automated updates, clinicians always have the current data on patient care, reducing repetitive tasks and improving the quality of care. The benefits of EHR integration in healthcare, after proper implementation, include better clinical decision-making and reduced administrative overload.
If you’re looking for a deeper architectural breakdown of how these interoperability standards come together in practice, explore our complete guide on Building EHR Systems With Seamless Integrations.
Essential Clinical System Connections Every EHR Must Support
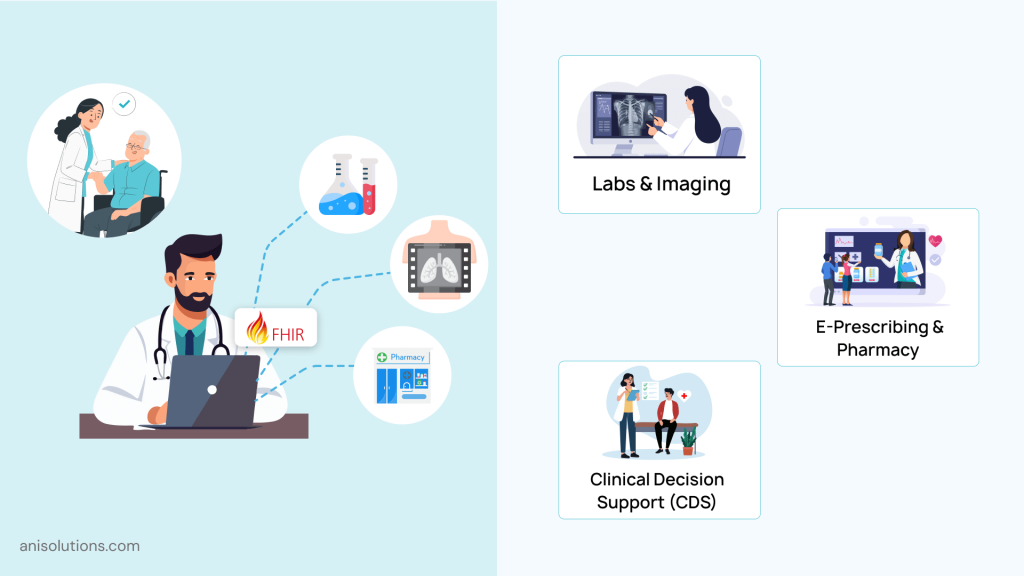
As said earlier, how well the EHR will share data depends on the systems integrated, and the first systems that are required for integration are clinical systems. In these essential EHR integrations for clinics, there are laboratory information systems, imaging systems, pharmacies, and CDS systems.
Here is how these systems benefit healthcare after integration:
- Laboratory & Imaging Systems (LIS, RIS/PACS): Laboratory and imaging systems are the first integrations and are foundational for any robust EHRintegration solution, as they make it possible to get lab results, diagnostic reports, and imaging data directly into the EHR. This reduces the cognitive load on clinicians as there is no need to constantly switch screens and enter data manually in patient records.
- E-Prescribing (eRx) & Pharmacy Integration: One thing that endangers patient health is a medication gap, missed allergy, or a side effect of medicine. However, if you have integrated pharmacy and ePrescriptions, then every change to medication, update in allergy, and care plan is automatically synced in pharmacies. This increases patient safety by alerting to potential drug interactions and improving patient outcomes.
- Clinical Decision Support (CDS): The CDS tools use real-time data and insights for better support of patient care. When this is integrated with EHR, which is connected to labs, imaging systems, and updated patient records, clinical decision-making is much more accurate and on time. It reduces the avoidable errors and helps clinicians transform the raw data into actionable insights.
In short, these systems give healthcare organizations a way to improve patient outcomes and safely deliver care. This is also why these are the essential EHR system integrations for clinics in modern healthcare.
Your Checklist to Integrating the Systems to Improve Interoperability
Get NowWhat to Integrate with EHR for Care Delivery and Administration?
Along with the clinical integrations, you also need to integrate systems that manage how care is delivered and how you get paid. In modern healthcare, care delivery is not just limited to offline mode, and telehealth platforms take care of patients remotely. Moreover, the administration system’s revenue cycle management software must be integrated for smooth claims processing and reimbursement.
Here is how these essential EHR integrations ensure continuity of care and reduce documentation gaps for clinics:
- Telehealth & Virtual Care Platforms: For healthcare, telehealth has become a permanent part, and patients are also preferring it over personally visiting clinics. That’s why it’s important for the data from telehealth to flow naturally into EHR to keep accurate patient records and continue care between in-person and remote care. Having robust integration between EHR and virtual care platforms rather than just adding telehealth as an extension allows clinicians shift between settings seamlessly.
- Revenue Cycle Management (RCM): Along with clinical efficiency, clinics also need financial stability and sustainability. This is where the integration with RCM becomes crucial, as it makes coding and billing easier and more accurate. When clinical documentation is connected to the billing platform, the charge capture and coding become precise, reducing mistakes in claim submission. With this denial rates and revenue losses are reduced, while allowing clinics to scale without hiring new administrative staff.
So, with seamless integration of care delivery and administrative systems, clinics are reimbursed on time while smoothly continuing care in both person encounters and virtual care settings.
How Essential EHR System Connections Deliver Real Value?
Meeting modern EHR integration requirements is not just about connecting healthcare systems, but about bringing value to clinics and growing healthcare organisations. When essential EHR integrations work together seamlessly, they reduce cognitive load, improve decision-making, and help organizations scale efficiently.
Here are the real benefits of EHR integration in healthcare:
| Value Driver | Operational Impact | Healthcare Value Delivered |
| Reduced system switching | Fewer logins and manual handoffs | Lower clinician cognitive load and burnout |
| Unified patient record | Centralized data across systems | Improved patient safety and continuity of care |
| Real-time data synchronization | Instant updates from integrated systems | Faster, more informed clinical decisions |
| Integrated documentation and billing | Accurate charge capture and coding | Improved reimbursement accuracy and reduced revenue leakage |
| Scalable integration architecture | Easier onboarding of new tools and services | Long-term ROI for growing clinics |
| Standardized data exchange | Consistent data flow across platforms | Stronger interoperability in healthcare |
Ultimately, robust EHR integration solutions that seamlessly integrate clinical and administrative systems transform EHR from a documentation tool into a platform connecting healthcare. It effortlessly supports better care delivery while remaining ready to grow with the evolving landscape.
Common Challenges in Meeting EHR Connectivity Requirements
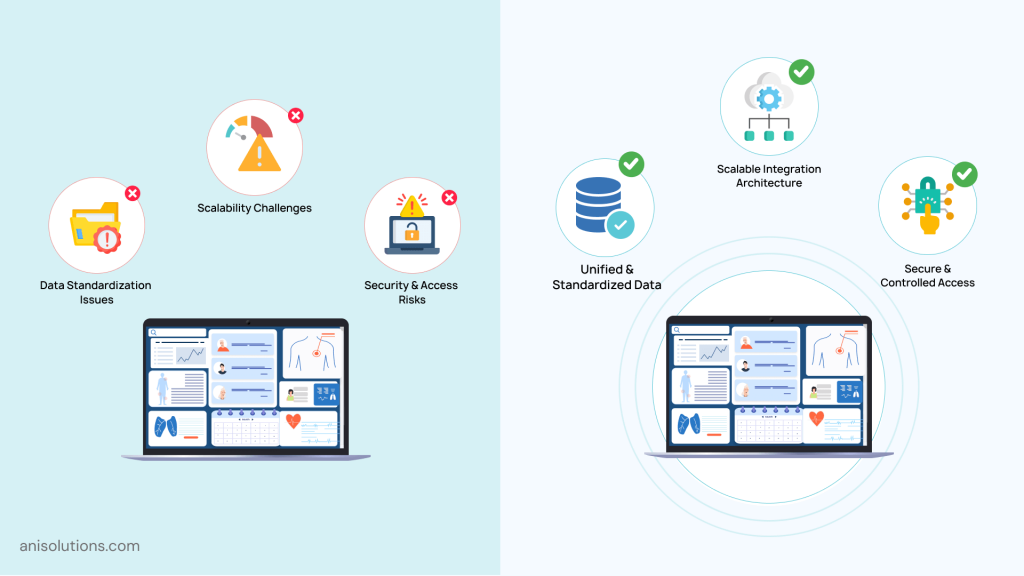
While modern EHR integrations are understood clearly, executing them in clinical settings is not that easy. If not done right, then the organization’s data can be fragmented, and most importantly, their digital ecosystems might be impacted, creating hindrances instead of seamlessly exchanging data.
That’s it’s crucial to understand what challenges are in successfully integrating systems into EHR solutions. This will help you address the problems early, helping in building EHR integration solutions that support growth without introducing new risks.
- Data Standardization Challenges Across Systems: One of the most common issues in EHR integration is inconsistent data standards across connected systems. Each platform, including lab, imaging system, billing, or pharmacy, may have different data structures, making it difficult to maintain clean, usable records. Without proper standardization, even the standards such as FHIR and USCDI can’t fill the gaps in implementation.
- Security & Access Control Across Integrated Endpoints: As integrations increase, so does the attack surface. Each connected system introduces new integration points, and if not secured well, these points can become the entry points for cyber attacks, leading to breaches of patient data. That’s why managing access through role-based access, audit trails, and data-sharing permissions across platforms is a major challenge, especially when sensitive patient data is involved.
- Scalability Concerns as Integration Needs Expand: Many EHR integrations work well initially but struggle as organizations grow. Adding new clinics, specialties, or care models can strain rigid architecture and point-to-point connections. This is why essential EHR system integrations for clinics must be designed with scalability in mind. Without flexible integration frameworks, organizations risk performance degradation, rising maintenance costs, or stalled upgrades.
Overcoming these roadblocks requires careful planning, standardization of data, and integration architectures that can evolve alongside care delivery.
Your Guide to Identify Data, Security, and Scalability Risks In Your EHR Integrations-
Click HereFinal Take: Building Essential EHR System Connections for Growth
In a nutshell, EHR integration is no longer optional in this connected healthcare environment. It is essential to have integrated systems to deliver safe care and a scalable ecosystem. That’s why meeting modern EHR integration requirements eliminates data silos, creates interoperability in healthcare, and helps clinics grow without slowing down care.
However, it’s also crucial to understand and identify the pitfalls in EHR integration. Doing this helps you avoid them early and build integrations that bring value and measurable impacts for clinics and growing healthcare organizations.
If you are thinking about integrating your EHR with external systems, then click here to book your demo and connect with our integration experts for developing robust EHR integration solutions.
Frequently Asked Questions
Q. What are the essential EHR integration requirements healthcare organizations must meet today?
In modern EHR, healthcare organizations must support real-time interoperability, secure data exchange, API-first design, and role-based access control. However, most importantly, they must comply with regulatory requirements. Modern EHR integration requirements focus on seamless connectivity, data accuracy, scalability, and continuous updates to patient records across systems.
Q. Which clinical integrations are considered mandatory for a modern EHR system?
For the EHR system, the mandatory clinical integrations are labs, imaging systems, e-prescribing, pharmacy platforms, and clinical decision support tools. These essential EHR integrations ensure timely access to diagnostic data, lab reports, and imaging data and turn raw data into actionable insights for clinicians.
Q. How do EHR integrations support interoperability using FHIR-based APIs?
FHIR-based APIs enable standardized, real-time data exchange between EHRs and external systems. They support interoperability in healthcare by enabling the secure sharing of structured patient data, such as medications, labs, and notes, across platforms without custom point-to-point integrations.
Q. What security risks should be considered when integrating external systems or devices with an EHR?
Key risks include unauthorized access, data breaches, insecure APIs, and weak endpoint controls. Strong authentication, encryption, audit logging, and role-based access are critical to ensure EHR integration solutions remain secure and compliant as integrations expand.
Q. How does revenue cycle management (RCM) integration impact the long-term sustainability of an EHR system?
RCM integration connects clinical documentation with billing workflows, reducing errors and revenue leakage. This alignment improves reimbursement accuracy, supports financial sustainability, and allows healthcare organizations to scale operations without increasing administrative complexity.
Q. What challenges do clinics face when scaling EHR integrations as patient volume grows?
As clinics scale, they face performance bottlenecks, data standardization issues, and rising integration maintenance costs. Without flexible EHR integration solutions, adding new systems or locations can strain workflows and limit long-term scalability.
In modern EHR, healthcare organizations must support real-time interoperability, secure data exchange, API-first design, and role-based access control. However, most importantly, they must comply with regulatory requirements. Modern EHR integration requirements focus on seamless connectivity, data accuracy, scalability, and continuous updates to patient records across systems.
For the EHR system, the mandatory clinical integrations are labs, imaging systems, e-prescribing, pharmacy platforms, and clinical decision support tools. These essential EHR integrations ensure timely access to diagnostic data, lab reports, and imaging data and turn raw data into actionable insights for clinicians.
FHIR-based APIs enable standardized, real-time data exchange between EHRs and external systems. They support interoperability in healthcare by enabling the secure sharing of structured patient data, such as medications, labs, and notes, across platforms without custom point-to-point integrations.
Key risks include unauthorized access, data breaches, insecure APIs, and weak endpoint controls. Strong authentication, encryption, audit logging, and role-based access are critical to ensure EHR integration solutions remain secure and compliant as integrations expand.
RCM integration connects clinical documentation with billing workflows, reducing errors and revenue leakage. This alignment improves reimbursement accuracy, supports financial sustainability, and allows healthcare organizations to scale operations without increasing administrative complexity.
As clinics scale, they face performance bottlenecks, data standardization issues, and rising integration maintenance costs. Without flexible EHR integration solutions, adding new systems or locations can strain workflows and limit long-term scalability.
- On February 7, 2026
- 0 Comment


