
Complete EHR Software Architecture Guide: Components, Layers & Design Principles
Right now, many clinicians are shifting to building their own EHR rather than using a generic system. When we ask why during the discovery phase, we hear a familiar answer — the EHR slows them down and doesn’t work how they do.
While these challenges create usability gaps, the real issue runs much deeper. In most cases, the problem is the EHR system architecture, meaning how the system is architected impacts its performance, compliance, and security.
More importantly, the architecture also decides how successful your EHR system development will be. The reason is that EHR software architecture is the blueprint or foundation for how each software component will work.
For instance, when you build a house, how well it will stand depends on the foundation rather than the interior or how you design it. The same principle applies to EHR software, as the EHR architecture decides how well the software performs.
As a result, each feature or EHR module from databases, user interfaces, workflow tools, and integration depends on the EHR architecture. That’s why knowing how to build a robust EHR architecture for a customizable EHR system significantly improves the chances of success.
This guide walks you through how modern EHR architecture affects clinics, best practices for implementing EHR software architecture, and the key components of EHR software architecture.
Core Layers of EHR System Architecture
Well, as said earlier, EHR software architecture is like the blueprint for the EHR system. This blueprint has layers for each software component, from database to integration. And these layers are what allow EHR to remain stable, secure, and scalable as clinics grow, regulations change, and operational needs evolve.
That’s why understanding these layers is crucial if you want to avoid performance issues, integration failures, and compliance risks. Even if a single layer in the whole architecture remains weak, the whole structure is affected. These layers together form key components of EHR software architecture.
Here is the breakdown of each layer and what they power in modern EHR systems:
| Layer | Purpose | Key Functions | Why It Matters |
| Presentation Layer | User interaction | Dashboards, portals | Impacts usability & adoption |
| Application Layer | Workflow logic | Automation, validation | Controls system behavior |
| Data Layer | Data storage | Records, retrieval | Enables reporting & scalability |
| Integration Layer | Connectivity | APIs, third-party systems | Enables interoperability |
| Security Layer | Protection | Access control, encryption | Ensures compliance |
1. Presentation Layer: Clinician, Admin & Patient Experience
This is the front-facing layer of the EHR systems that powers the user experience. In this layer, the features such as the clinician dashboard, administrators’ interfaces, and the patient portals are located.
The primary goal of this layer is to:
- Capture and display data accurately
- Support role-based user experience
- Enable intuitive workflows without exposing backend complexity
If this layer is not designed accurately, it can impact the whole user experience and EHR adoption.
2. Application & Business Logic Layer: Workflows and Rules
In the EHR application architecture layer, the operational capabilities of the EHR are defined, including how data moves, how workflows function, and administrative rules.
Key responsibilities include:
- Clinical workflow orchestration
- Validation of data and actions
- Automation of routine tasks
- Enforcement of business and regulatory rules
In modern EHR architecture, this layer is separated from the user interface. This allows workflows to evolve without a complete overhaul of the system.
3. Data & Storage Layer: Clinical Records and Content
This is where the patient information is stored, retrieved from, and protected. It handles both structured and unstructured data, such as clinical records and lab reports, along with unstructured data, including images and visit notes.
A strong data architecture supports:
- Data consistency across modules
- Auditability and traceability
- Efficient querying and reporting
- Long-term scalability
If designed poorly, it limits the reporting capabilities and makes future integrations significantly harder.
4. Integration Layer: Internal and External Connectivity
The integration layer is what connects EHR to other healthcare systems, creating a broader ecosystem rather than isolating it.
This layer supports:
- Communication between internal services
- Integration with labs, pharmacies, billing systems, and third-party tools
- Standardization data exchange using APIs and interoperability frameworks
Without this layer, expansion is crucial, for expansion as adding new systems becomes difficult and risky with core-system changes.
5. Security & Compliance Layer: Protection and Governance
This is the protection layer of the whole system with security and compliance. This layer has:
- Role-based access control
- Authentication and authorization
- Audit logging and traceability
- Data encryption and protection mechanisms
This layer needs to be embedded with HIPAA-compliant enforcement consistently across every workflow, module, and integration.
Why These Layers Matter in EHR?
When all architectural layers are brought together, EHR becomes efficient, but it also needs clear separations and interactions. More importantly, this layered structure forms the foundation for the robust EHR system.
If not done right, the EHR becomes hard to maintain, harder to secure, and even harder to scale.
Download A Simple EHR System Architecture Layer Diagram for Better Understanding
Click HereModern EHR Architecture Approaches: Custom vs Off-the-Shelf
As healthcare is evolving with modern technology, EHR software architecture is also changing with it. And in this, there are two approaches, custom and off-the-shelf, and here, architecture becomes a major difference.
Both of these may seem similar at first glance, but how their architecture is built changes how well they support workflows, compliance, and integration. However, the way they are implemented changes between off-the-shelf and customizable EHRs.
Here is how this implementation affects the outcomes over time:
| Aspect | Off-the-Shelf EHR Architecture | Customizable EHR Architecture |
| Workflow Design | Generic workflows for broad use cases | Architecture aligned to real clinical workflows |
| Flexibility | Limited customization without core changes | Modular and adaptable by design |
| Scalability | Growth constrained by vendor architecture | Designed to scale with organizational needs |
| Integration | Dependent on vendor-controlled APIs | API-first, integration-ready foundation |
| Compliance Adaptation | Changes tied to vendor update cycles | Easier architectural adjustments over time |
| System Ownership | Vendor-driven roadmap | Full control over architecture and evolution |
So, when off-the-shelf EHRs are built, they are built for speed and standardization. While this works to some extent, it can’t be used long-term and creates multiple gaps, integration bottlenecks, and limited flexibility.
A custom EHR architecture allows far more flexibility and lets healthcare organizations design a system around how care is actually delivered. This gives a better long-term scalability, security, compliance, and interoperability, building a better foundation for the EHR system.
Security & Compliance Foundations in EHR Architecture

One of the most important aspects of the EHR architecture is security and compliance, and it needs to be built into the core EHR software. If not done right and added later as a layer, after the development process of custom EHR solutions, it becomes costly, risky, and feels incomplete.
In a modern EHR system, HIPAA compliance must be an integral part of development, not an afterthought.
1. Why Compliance Must Be Built Into the Architecture
EHR architectures that treat security as a separate layer often struggle with inconsistent access controls across modules. More importantly, these systems face gaps in audit logging during integration, difficulty proving compliance during audits, and increased risk when scaling the system.
However, when you take a compliance-and-security-first approach, it ensures that security is consistent across workflows, APIs, and third-party integrations.
2. Architectural Considerations That Impact Security
In EHR system architecture, there are many decisions that impact how robust the compliance and security of the system will be. These decisions include role-based access control embedded across services, centralized audit logging, secure data storage, and transmission patterns.
However, what makes this successful is a clear separation between clinical, administrative, and external access, as this keeps sensitive information private and protected.
Want a deeper technical breakdown of compliance-driven system design? Read this blog: Achieving HIPAA-Compliant EHR Architecture.
Access A HIPAA-Ready EHR Architecture Requirements Checklist
Access NowAPI-First Design: Enabling Speed, Flexibility, & Integration
When you want to scale the system, you need to integrate new systems, and that’s where an API-first design plays a critical role. It allows you to develop a flexible system that enables you to adapt without disrupting the workflows.
Furthermore, an API-first approach means deciding how the systems will communicate with each other in real-time. These APIs act as bridges and communication layers between internal modules and external systems.
1. What API-First Means in Modern EHR Architecture
In an API-first EHR system, every major capability, including clinical data access, scheduling, billing, reporting, and notifications, is exposed through well-defined, secure APIs. This allows different components of the system to evolve independently while remaining connected.
This approach keeps different EHR components loosely connected rather than tying them together. Meaning, teams can build or update features at the same time without depending on each other, and new capabilities can be added later without changing the core system.
2. Role of APIs in Integration & Extensibility
APIs are the backbone of modern healthcare connectivity. They enable EHR systems to integrate with labs, imaging, and pharmacy systems, along with billing systems and patient engagement tools. With an API-first foundation, adding or replacing integrations becomes a configuration exercise rather than a risky architectural change.
3. Why API-First Replaces Monolithic EHR Systems
Traditional monolithic EHR architectures bundle logic, data, and workflows into tightly connected components. While this may simplify early development, it shows innovation and increases risk over time.
API-first architecture breaks this dependency. It allows EHR systems to scale, integrate, and modernize slowly without disrupting clinical operations.
If you’re planning a modular and integration-ready system. Read this blog: API-First Architecture for EHR Systems.
Interoperability by Design: Building Connected Healthcare Systems
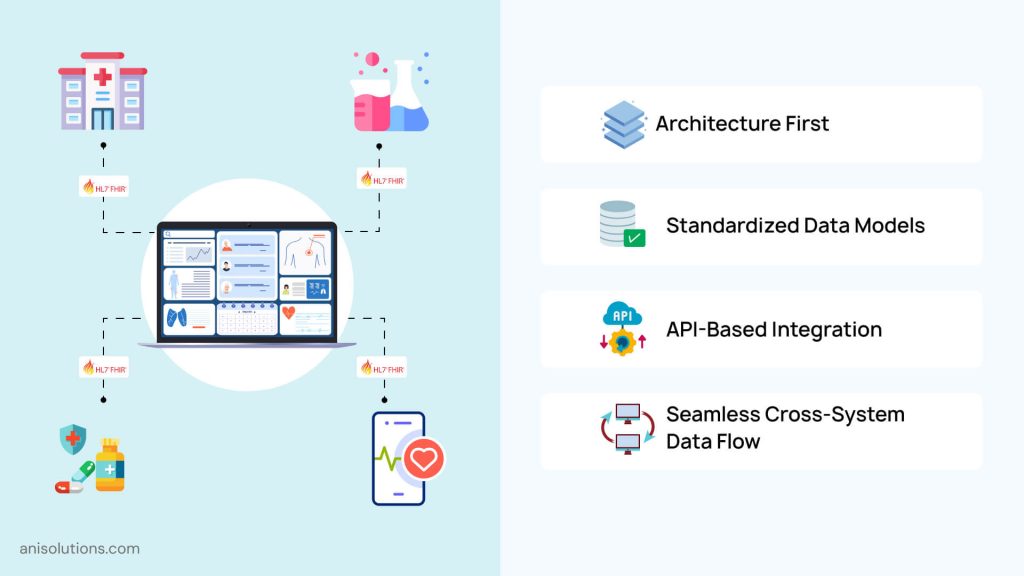
In an EHR, the lack of interoperability is often blamed on missing standards or incompatible vendors. In reality, most interoperability failures stem from architectural decisions made early on. When interoperability is treated as an add-on rather than a design principle, EHR systems struggle to exchange data reliably across care settings.
So, in a modern EHR, interoperability must be designed into the architecture, not added later in the development.
1. Why Interoperability Failures Are Often Architectural
Many EHR systems store and manage data in ways that make sharing difficult, as data models are tightly embedded in internal workflows. Moreover, integration completely relies on custom point-to-point connections, and external data access is limited or inconsistent throughout the network.
These architectural limitations make even standards-based integrations fragile and hard to scale. As systems grow, each new connection increases complexity rather than reducing it.
2. Importance of Standardized Data Exchange Frameworks
When it comes to modern EHR architecture, it relies on standardized data exchange frameworks to enable consistent and secure communication between systems. In EHR, these standards define how clinical data is structured, how it is accessed, and how updates and changes are tracked.
With these frameworks supported at the architecture level, EHR systems can exchange data more seamlessly across hospitals, clinics, labs, and third-party platforms.
3. Designing EHRs for Seamless Cross-System Communication
Interoperable EHRs are designed with clear data boundaries and ownership, along with API-based data access instead of direct database sharing. More importantly, it is designed with consistent handling of external and internal data. And this approach allows EHR systems to participate in broader healthcare networks without compromising performance, security, or data integrity.
To understand the architectural frameworks behind real-time data exchange, read this blog: How to Build a Fully Interoperable EHR.
Scalability & Performance: Designing EHR Architecture for Multi-Clinic Growth
Many EHR systems work well when used by a single clinic, but begin to struggle as organizations grow. With each new location, provider, or service line, the complexity increases and creates architectural weaknesses.
This is why scalable EHR software architecture needs to be addressed at the architecture level, not patched later as operational issues arise. In a scalable EHR system, growth is anticipated and supported by design.
1. Challenges of Scaling Beyond a Single Practice
As clinics grow, EHR systems often face many challenges. The common challenges are slower responses as the number of patients increases, data conflicts between locations, limited visibility, and performance reduction at peak time. These issues are rarely caused by hardware limitations. They are usually the result of an architecture that was never designed for multi-clinic use.
2. Architectural Considerations for Multi-Clinic Environments
When you are building a multi-clinic environment with a ready EHR architecture, there are some things to consider. You have to separate clinic-specific data from shared system services while supporting configurable workflows across locations. Moreover, it allows new clinics to be added without restructuring the core system. This approach ensures that expansion does not introduce instability or excessive technical debt.
3. Performance, Data Isolation, & Centralized Governance
As systems scale, maintaining performance and control becomes critical. Modern EHR architectures balance data isolation, so each clinic operates independently. They also use centralized governance for reporting, compliance, and oversight. They even add performance optimization, so system responsiveness remains consistent.
When these elements are built into the architecture, organizations can scale confidently without compromising reliability or clinician experience.
Planning expansion across multiple locations? Read this blog: Scaling EHR for Multi-Clinic Use.
Best Practices for EHR Software Architecture
Designing a successful EHR system isn’t just about choosing the right technologies; it’s about making sound architectural decisions early. The following best practices help ensure that EHR software architecture remains resilient, compliant, and adaptable as clinical and business needs evolve.
1. Build Security & Compliance Into the Core Design
Security and compliance should be embedded at the architectural level, not added later as features. Role-based access control, audit logging, and data protection mechanisms must be enforced consistently across all modules, workflows, and integrations.
2. Design for Interoperability From the Beginning
Interoperability works best when EHR systems are designed to exchange data from day one. Supporting standardized data exchange and API-based access early prevents costly rework and reduces integration complexity as the system grows.
3. Keep the Architecture Modular & Adaptable
Modular architecture allows individual components, such as workflows, reporting, or integrations, to evolve independently. This reduces system-wide risk when changes are required and makes it easier to introduce new capabilities without disruption.
4. Plan for Scalability Before Growth Demands It
Scalability should be a part of the EHR architecture, rather than a future fix. Designing for increased user, clinics, and data volume upfront helps maintain performance and avoids architectural redesigns as the organization expands.
Choosing the Right Architecture for Your EHR Vision
If you’re reading till now, one thing should be clear: EHR software architecture is not a technical detail; it’s a long-term strategic choice. The architecture you choose will shape how your EHR performs, scales, integrates, and adapts to regulatory and clinical change over time.
Before committing to development or modernization, healthcare organizations need to step back and evaluate whether their architectural direction truly supports their goals.
1. Key Questions to Ask Before EHR Development
Choosing the right architecture starts with asking the right questions:
- Does the architecture align with how clinicians actually work today?
- Can it support future workflows, service lines, or care models?
- How easily can it adapt to new compliance requirements?
- Will integrations and extensions require core system changes?
- Is the architecture designed to scale without degrading performance?
These questions help shift the conversation from features and UI preferences to structural readiness.
2. Aligning Architecture With Clinical & Business Goals
Strong EHR architecture connects clinical efficiency with operational priorities. When architectural decisions are aligned with both care delivery and business objectives, organizations gain:
- Faster adoption by clinical teams
- Greater flexibility to innovate
- Lower long-term maintenance and redesign costs
This alignment is especially critical for organizations investing in architecture for custom EHR solutions, where early decisions have a lasting impact.
3. Avoiding Costly Redesigns Through Early Planning
Many EHR initiatives fail not because of poor execution, but because architectural decisions were made too late or revisited too often. Investing time in architectural planning upfront reduces rework, minimizes risk, and creates a more predictable development path.
Evaluate Your EHR Architecture Readiness Assessment
Get NowConclusion: Why EHR Software Architecture Is a Long-Term Strategic
EHR software architecture is the foundation on which the entire EHR system works. So, if your architecture is not robust enough, then everything from performance to security and compliance gets affected tremendously.
Many common EHR challenges stem from architectural limitations rather than surface-level design issues. Organizations that prioritize architecture early are better able to support complex workflows, integrate new technologies, and respond to regulatory change without constant redesign.
Whether building a customizable EHR or modernizing an existing system, investing in the right architectural approach reduces risk and creates a platform that can grow with your clinical and business needs.
If you are planning to build your EHR, now is the right time to evaluate whether your architecture truly supports your long-term vision. Click here to book your demo and take the first step in building the robust EHR software architecture.
Frequently Asked Questions
Q. What is EHR software architecture, and why is it important for modern healthcare systems?
EHR software architecture defines how an EHR system is structured and how its components work together. It’s important because it directly affects performance, security, interoperability, scalability, and how well the system adapts to modern healthcare needs.
Q. What are the key components of an EHR system architecture?
Key components include the presentation layer, business logic layer, data and storage layer, integration layer, and security layer. Together, these layers ensure smooth workflows, secure data handling, reliable integrations, and long-term system stability.
Q. How does EHR software architecture differ from EMR architecture?
EHR architecture is designed for interoperability and data sharing across systems, while EMR architecture typically focuses on internal clinical documentation within a single organization. EHRs support broader care coordination, integrations, and long-term scalability.
Q. Why does EHR architecture matter more than features when building a system?
Features can be added or changed over time, but architecture determines how flexible, secure, and scalable the system can be. Poor architecture limits performance and growth, no matter how advanced or attractive the features appear.
Q. How does modern EHR architecture support scalability and long-term growth?
Modern EHR architecture uses modular design, APIs, and scalable infrastructure. This allows organizations to add clinics, users, and services without redesigning the system, while maintaining performance and avoiding operational disruptions.
Q. How does EHR software architecture help achieve HIPAA compliance?
HIPAA compliance is easier when security, access controls, audit logs, and data protection are built into the architecture. Architectural enforcement ensures compliance is consistent across workflows, integrations, and system updates—not added later as patches.
Q. What architectural elements are essential for securing patient data in EHR systems?
Essential elements include role-based access control, encryption, centralized audit logging, secure data storage, and controlled APIs. These architectural safeguards protect patient data while supporting clinical workflows and regulatory requirements.
Q. Can poor EHR architecture lead to compliance and security risks?
Yes. Poor architecture often creates gaps in access control, audit trails, and data handling. These weaknesses increase the risk of data breaches, failed audits, and non-compliance—especially as systems scale or integrate with external platforms.
Q. What is API-first architecture in EHR systems?
API-first architecture designs system communication upfront, allowing different EHR components and external tools to connect through APIs. This makes integrations easier, reduces system dependencies, and supports faster updates without disrupting core workflows.
Q. How does API-first design improve integrations and system flexibility?
API-first design allows new tools, services, and workflows to connect without modifying the core system. This improves flexibility, speeds up integrations, and enables EHR platforms to evolve gradually instead of requiring risky system-wide changes.
EHR software architecture defines how an EHR system is structured and how its components work together. It’s important because it directly affects performance, security, interoperability, scalability, and how well the system adapts to modern healthcare needs.
Key components include the presentation layer, business logic layer, data and storage layer, integration layer, and security layer. Together, these layers ensure smooth workflows, secure data handling, reliable integrations, and long-term system stability.
EHR architecture is designed for interoperability and data sharing across systems, while EMR architecture typically focuses on internal clinical documentation within a single organization. EHRs support broader care coordination, integrations, and long-term scalability.
Features can be added or changed over time, but architecture determines how flexible, secure, and scalable the system can be. Poor architecture limits performance and growth, no matter how advanced or attractive the features appear.
Modern EHR architecture uses modular design, APIs, and scalable infrastructure. This allows organizations to add clinics, users, and services without redesigning the system, while maintaining performance and avoiding operational disruptions.
HIPAA compliance is easier when security, access controls, audit logs, and data protection are built into the architecture. Architectural enforcement ensures compliance is consistent across workflows, integrations, and system updates—not added later as patches.
Essential elements include role-based access control, encryption, centralized audit logging, secure data storage, and controlled APIs. These architectural safeguards protect patient data while supporting clinical workflows and regulatory requirements.
Yes. Poor architecture often creates gaps in access control, audit trails, and data handling. These weaknesses increase the risk of data breaches, failed audits, and non-compliance—especially as systems scale or integrate with external platforms.
API-first architecture designs system communication upfront, allowing different EHR components and external tools to connect through APIs. This makes integrations easier, reduces system dependencies, and supports faster updates without disrupting core workflows.
API-first design allows new tools, services, and workflows to connect without modifying the core system. This improves flexibility, speeds up integrations, and enables EHR platforms to evolve gradually instead of requiring risky system-wide changes.
- On February 1, 2026
- 0 Comment


